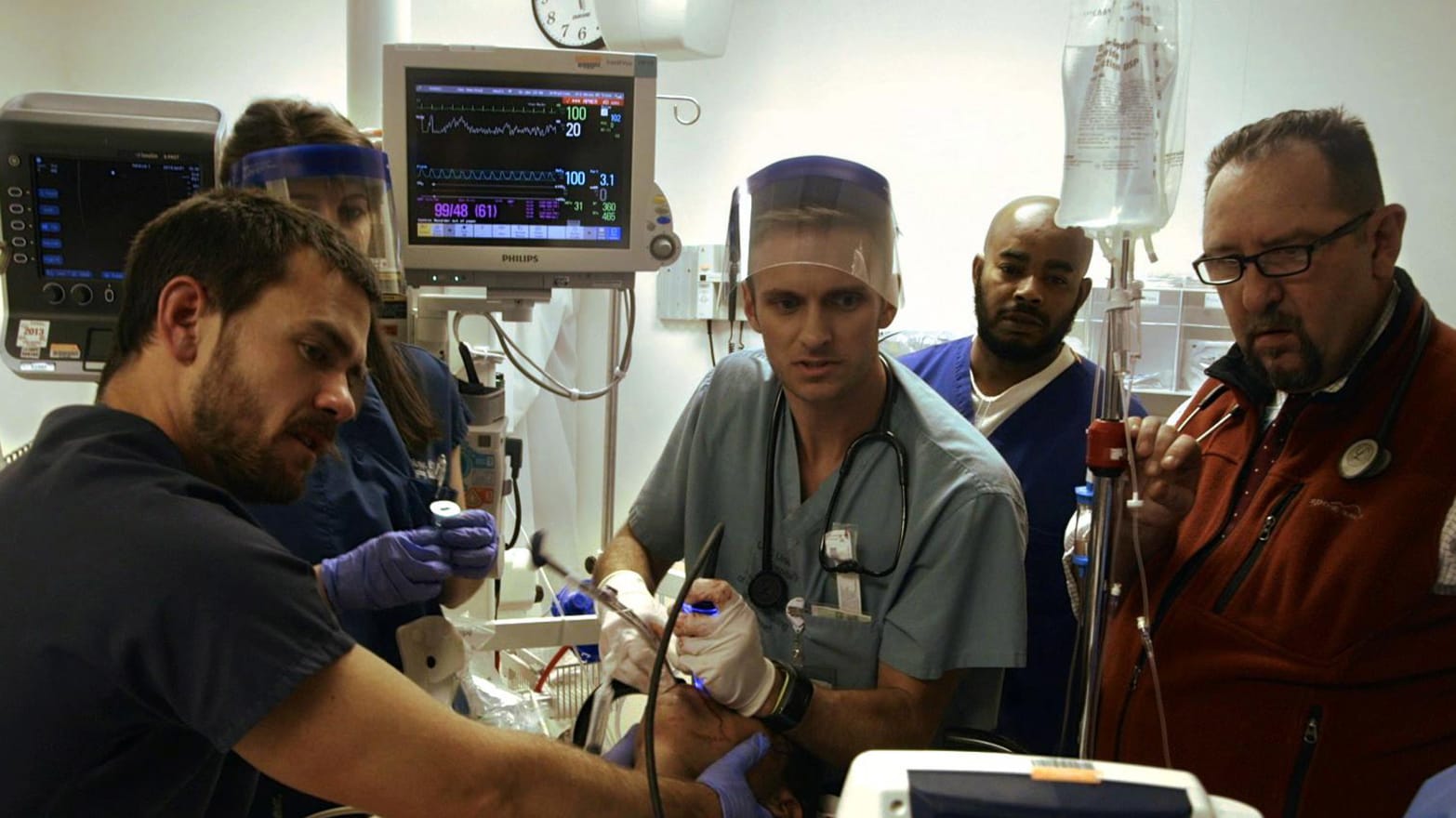
Chances if you’re reading this, you’re young, healthy and you think about health insurance like you do car problems—it’s not really on your mind unless something is wrong. Yet I would argue your experience at the car mechanic might be better than the American ER, which is where I work as a 32-year-old physician. Here’s why:
You end up at the ER in the first place when probably you needed a Midas.
The ER, at least in theory, is for the equivalent of needing a major transmission repair, engine block problem—something ominous that needs major attention immediately. And maybe you do have a perforated appendicitis. But chances are your problem, while urgent, is not an emergency.
So then why end up here versus the primary care equivalent of a Midas for a simple checkup? The answer, we all know, and I’m not blaming you, is that making a doctor’s appointment is a huge pain in the ass. In fact, you may not even have an established primary care doctor and to find one involves a crappy insurance company website, availability worse than banking hours (if they can take you at all), and the unpalatable likelihood that you’ll have to take a full day off of work. The ER—at least on the surface—is a mirage to many of these inconveniences. But then you arrive and…
Your car isn’t the only one in the lot.
Actually there’s 100 here. Or more. We’re starting to see that post-Obamacare, ER visits are going up nationwide. Maybe this seems counterintuitive? Obamacare definitely gives a lot more Americans insurance cards and technically this should mean more health care access. But here’s the issue—those cards aren’t always premium. And we are already in a system where many specialists won’t take sub-premium insurance plans because on those plans, you are seen as not profitable enough. So many insurance-carrying, hard-working people still must go to the ER, often at a public hospital, just to get non-emergent specialty care. So take a number, but when it is finally called, don’t expect highly personal attention because…
We can’t really look at you right now.
Seriously. My doctor and nurse colleagues have to fight for eye contact with you. I swear we all went into this because we like people and most importantly the idea of healing you is very rewarding. But of the 10, maybe 15 minutes I have with you (don’t forget, there’s 100 people out there, and another 30 in here), I have to type the equivalent of this entire article on you and every other patient I see. How many times did we ask about your allergies? Medication lists? You already gave that info when you walked in the door, but your local car shop probably has a more advanced electronic records system than most hospitals do, and that information doesn’t always import to me, your doctor. “EMRs,” the very PC-sounding acronym for the now required electronic medical record systems (which are required by all hospitals and doctors offices), are almost always like using Windows 95—in 2014—when pretty much everyone else is using a Mac. But let’s say your experience has actually been good, we fixed your issue, and now you ask the entirely reasonable, completely rational question of “How much will this cost,” and…
We literally have no idea how much we just charged you.
Even the most sketch-ball, scheming car mechanic knows how much those brake pads cost. But here’s the thing—and truly in defense of any medical conspiracy you may think is going on at the provider level—we have no freaking clue how much that EKG or X-ray costs you. Partly because, it’s a different price for everyone depending on your plan (might even be “free”), but also because, we really don’t know, and even our bosses don’t know. Recently a LA Times columnist wrote a brilliant article on the degree of paper trail it took to find out how much a bag of saline cost. Somebody definitely knows. But the lack of transparency is almost the same for me as it is for you. Happily we are taught as medical students and residents to a) never harm you and b) explain to you what you need and what you don’t need, and sometimes I like that the idea of money, when it comes to your life, is not a first-tier consideration in that equation. But let’s not forget the reason you’re here in the first place. You came to the ER because you want service and answers now, not in two weeks…and while I may not know the exact prices, the ER is the dealership mechanic—everything here is more expensive.
This is a pretty dismal assessment. I will say that I’m proud to be in the specialty of Emergency Medicine because I think, by and large, you car will leave tuned up (so to speak) and we do this as a specialty at more uncompensated rates than any other. But I wish the experience was better; not just in the ER—health care in general. If I can successfully compare a doctor’s visit even loosely to a trip to an auto shop (no offense, Pep Boys!), then there are clearly issues here. It’s your health, not a carburetor.
How do we solve this? I think the first step, albeit unsexy and untextable, is to be vocal. Much of this I would argue is my responsibility as a physician, not just yours. Doctors and nurses and providers have to take back some control of the patient experience. We feel regulated, not remotely in charge, yet we’re by far the most invested in your health and experience. It frustrates me that I plunged $300K into debt and missed every weekend of my 20s to be a physician, but a “suit” with an online MBA is often deciding what’s best for you.
The good news is, I think this generation of doctors and nurses can leverage our so-called millennial entitlement for the patient’s benefit. The patient-provider experience should be entitled. It should be the most ideal exchange, not the most haphazard. Our health is worth that much. The key now is demanding that expectation and as medicine continues to change, providers can’t just be providing—we have to be fighting, for you. And that’s something you don’t expect at the auto shop.