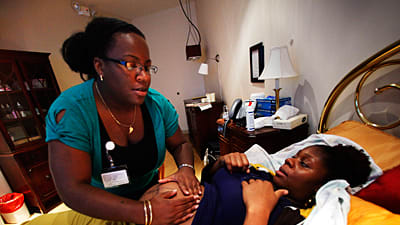
Ask your average American what a midwife is and you'll probably get a puzzled stare in return. Midwife? Isn't that a kind of witch doctor, discarded by society with the dawn of modern medicine? Do midwives still exist today?
They do, of course—and I am living proof. Midwives have attended women in pregnancy and childbirth for thousands of years, across cultures. Yet midwives are far too rare in this country, particularly compared with nearly every other country in the world. The fact that they seem outmoded here illustrates a deeper problem: not only is the profession of midwifery at risk of dying out, but also the very process of giving birth the way nature intended seems on the brink of extinction. These are just a few of the disturbing trends women will be fighting when they take to the streets today, in honor of the International Day of the Midwife.
In the U.S., one in three babies is now born surgically, despite the World Health Organization’s recommendation that rates not exceed 10 percent in hospitals serving the general population, or 15 percent in hospitals serving high-risk cases. When C-section rates are too low, women and babies will pay with their lives, but the same result occurs when C-section rates climb too high. This is a lesson we have yet to learn in the U.S.
According to the Centers for Disease Control, a woman giving birth today is more than twice as likely to die in childbirth as her mother was. The recent leading cause of maternal death in New York was pulmonary embolism, a complication whose incidence rises significantly after C-section. Equally concerning, far more babies than ever are born after a host of technological interventions such as induction and the use of pitocin to speed up labor, which bring along their own risks. Statistics like these compelled Amnesty International to publish a damning report in 2010 titled Deadly Delivery: The Maternal Health Care Crisis in the USA, which outlined various failures in the way our health-care system treats pregnancy and birth.
How has it come to this? A century ago, when the specialty of obstetrics was in its infancy in the U.S., its founders decided that they could only succeed in promoting their profession by demonizing midwifery. Using racist and anti-immigrant slogans and caricatures, they organized a campaign to make midwifery illegal in every state possible and to frighten women away from choosing midwives by portraying them as dirty, ignorant, and evil.
As a result, when birth moved into hospitals, there were no midwives around to counter the tendency for ignorant, frightened young doctors to try to hurry a birth that would have proceeded without problems if they had just allowed a laboring mother to relax or to assume a more effective position. Only in the U.S. did obstetricians become convinced that birth was so potentially dangerous to mother and baby that they could accept the doctrine that two thirds of all babies should be pulled out of their mothers with forceps—our forceps rate in the mid-'60s, when I gave birth the first time. Because midwives remained an integral part of maternity-care staff in every other wealthy country, obstetrics in those countries never took on the fear of natural processes that has afflicted maternity care here in the U.S. for the last century.
A century ago, the founders of obstetrics decided that they could only succeed in promoting their profession by demonizing midwifery.
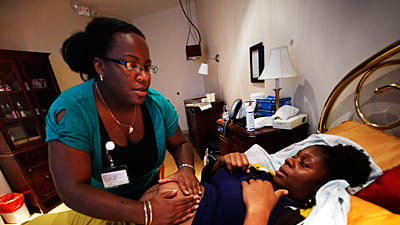
At medical schools around the country, the time-tested skills that are central in the education of midwives are no longer valued. In November 2007, in Cape Fear, N.C., a news report from a local television station caught my attention: a woman was subjected to a C-section during which the obstetrician, who cut into her abdomen, discovered that she wasn’t even pregnant. According to that obstetrician, “several doctors had examined and attempted to induce labor on the patient for several days before the C-section incident.” Not one of them seems to have manually checked the accuracy of the diagnosis of pregnancy; the intern who looked at the woman’s ultrasound and found no heart beat had assumed that “the baby” had died—failing to take into account that sometimes there is no baby inside a woman who thinks she’s pregnant and has some superficial signs of pregnancy.
Electronic discussion of this bizarre group mistake guessed that the intern who “diagnosed” the pregnancy had probably mistaken retained fecal material for a baby. I found that comment amusing, since I’ve never once felt an accumulation of poop in the shape of a baby. However, I have diagnosed two false pregnancies, one of them during my first few months of caring for pregnant women. Hands are still useful—even in the era of ultrasound.
With this radical shift, more and more doctors and nurses finish their training without ever observing an undisturbed vaginal birth—a situation that tends to send C-section rates even higher. And one that could be improved if more hospitals relied on midwives to balance medical leaders’ tendency to treat every labor as a disaster about to happen.
Many U.S. obstetricians themselves lament our collective history as much as I do, and they are rightly embarrassed by the loss of traditional skills in their profession. I know this, because I am getting more invitations to lecture obstetrics faculty and residents at teaching hospitals than ever before. They know that we midwives recognize the necessity for obstetrics, but at the same time, they know that obstetrics also needs midwifery if it wants to stop pathologizing every pregnancy and birth. More and more doctors themselves are voting with their feet by choosing midwife-attended births. In fact, the last birth I attended was for an obstetrician who chose not to give birth where she worked.
Instead of creating safer births and healthier moms and babies, our overuse of technology has caused a host of problems. My friend, Dr. Tadashi Yoshimura, a Japanese obstetrician, talks about how he suddenly became aware of how terrifying standard hospital routines can be to women in labor when he looked at a television monitor showing the face of a laboring woman who was hooked up to various devices and left alone. As he began to substitute routine use of technology with a caring and observant midwife for each woman, he got to see what he termed "the mystic beauty" of a laboring woman who is not frightened and is thus powerful in bringing forth life.
I know exactly what he is talking about because I saw that on the face of the first woman I ever observed giving birth. He learned what I learned: that for the most part, nature gets it right in birth. Women's bodies are not lemons. The creator is not a careless mechanic. The same process that has brought hundreds of thousands of years of human beings to earth can continue to do so today. The human species is no more unsuited to give birth than any other of the 5,000 or so species of mammals on the planet. We are merely the most confused.
What makes midwives special and indispensable is their respect for women, for women’s choices, and their awe at the beauty of birth. Today, on the International Day of the Midwife, I would like to recognize all the midwives and other birth professionals who have put themselves on the line to provide the best possible care for women and babies. I hope that, through their guidance, we can make birth in the U.S. safer and more empowering.
Ina May Gaskin, called the “midwife of modern midwifery” by Salon, has practiced for nearly 40 years at the internationally lauded Farm Midwifery Center. She is the only midwife for whom an obstetric maneuver has been named (Gaskin maneuver). She is the author, most recently, of the new book Birth Matters: A Midwife’s Manifesta.