Purdue Pharma’s attempt to stem a mushrooming opioid crisis by reformulating OxyContin is the reason why heroin replaced it and took off, causing the crisis to explode into a full-blown epidemic, according to a new working paper.
Not only that, the paper’s authors—economists William N. Evans and Ethan Lieber of the University of Notre Dame, and Patrick Power of Boston University—narrow down the switch to August and September 2010. Once OxyContin’s formula changed, it became too expensive to get high off the drug, making heroin the obvious choice as its replacement, they write in the paper, published online with the National Bureau of Economic Research.
It’s not necessarily the first paper to come to this conclusion—another NBER paper from January 2017 cites similar results—but the new paper manages to pinpoint down to the month when the dramatic change occurred. Perhaps more important, as the paper states in its abstract, the “reformulation did not generate a reduction in combined heroin and opioid mortality—each opioid death was replaced with a heroin death.”
And then some, it appears from data.
Lieber, an assistant professor of economics at the University of Notre Dame, said it’s clear a substitution effect of sorts was occurring. “What we were doing when we came across this data was asking two questions: Is something changing somewhere in this time line? And if so, when is it changing?”
The substitution effect will likely be a familiar term for anyone who’s ever taken an Economics 101 course. It’s a pretty simple concept: When the price of a good rises, the consumer will redirect their purchase of said product toward a cheaper alternative. If, for example, the price of name brand, gourmet string cheese goes up, consumers will veer towards the generic, less fancy but cheaper mozzarella stick as a substitute.
Lieber and his colleagues found evidence of the substitution effect with OxyContin and heroin.
Indeed, Lieber said it came down to a single month. “In August 2010, something is changing in opioid use,” he pointed out. “And in September 2010, something is changing for heroin use.”
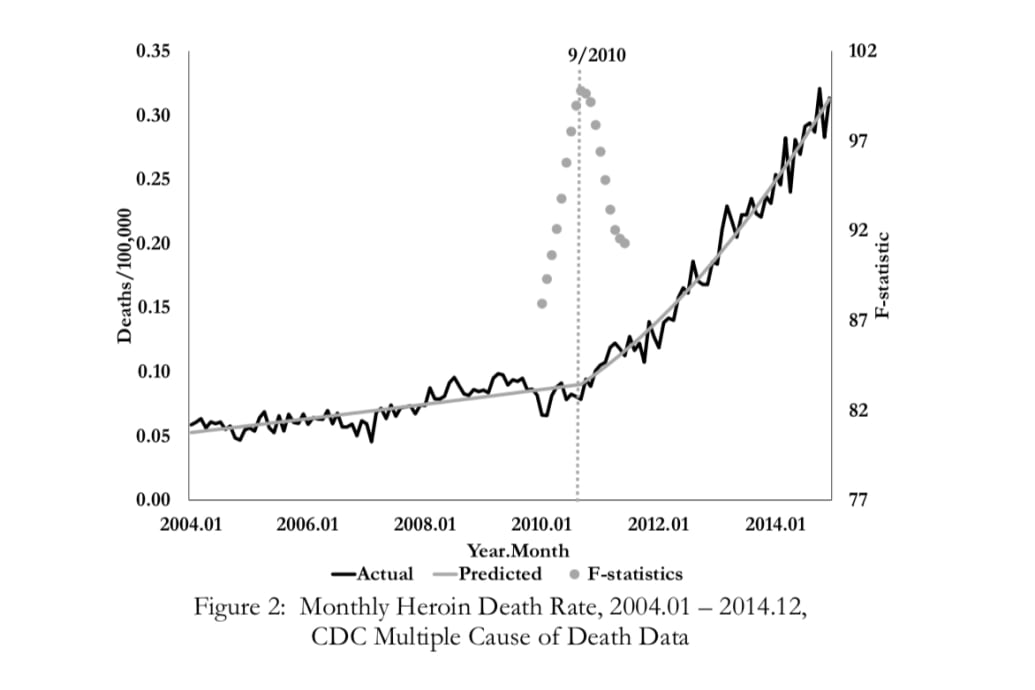
Courtesy Evans, Lieber, Power / NBER
And the causes of death almost immediately followed suit, with death rates from oxycodone peaking right around August 2010, then flattening. Heroin deaths starting spiking around September 2010.
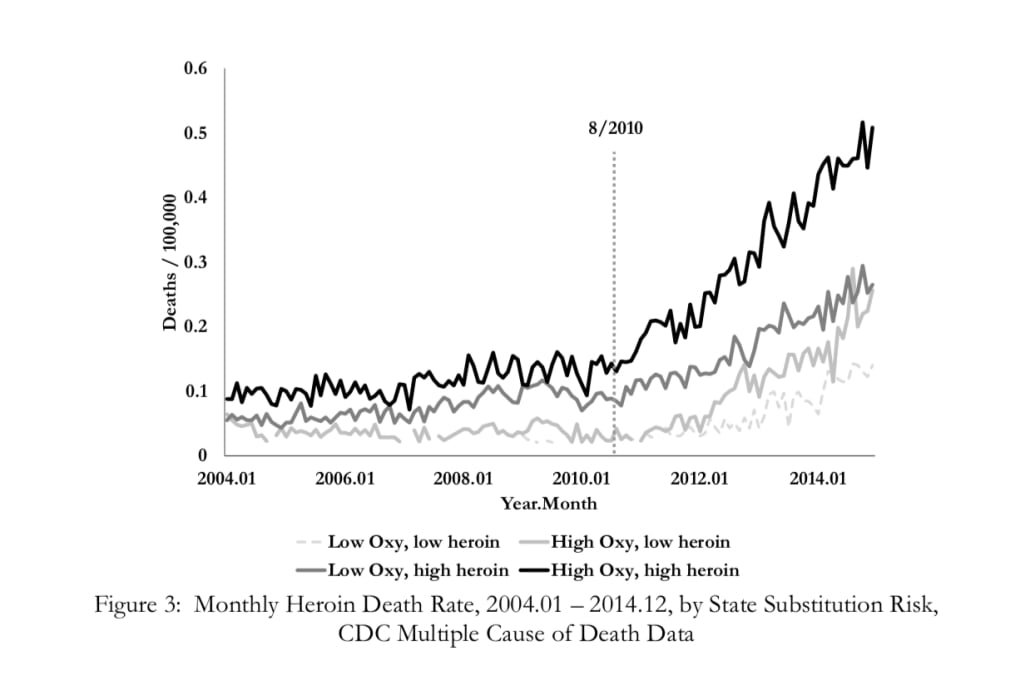
Courtesy Evans, Lieber, Power / NBER
To understand why the late summer and early fall of 2010 was pivotal for the opioid epidemic requires a bit of a back story on OxyContin reformulation, the FDA, and pill smashing.
Almost exactly five years ago, the Food and Drug Administration made a decision that helped plunge Americans into what has evolved into an unprecedented epidemic: Unlike other pharmaceuticals, it would not allow Purdue Pharma’s blockbuster narcotic, OxyContin, to go generic.
By 2013, OxyContin had already developed a reputation as an addictive narcotic, a drug that, on paper, helped ease chronic pain, but could become highly habit forming, particularly when combined with alcohol. Approved in 1995, its undeniable ability to treat moderate to severe pain helped boost it to superpower status.
But patients and their doctors soon noticed that a huge problem with OxyContin’s composition made users more likely to become addicted. When crushed, the pill would become a powder, potentially flooding its total narcotic capabilities into the bloodstream rather than in bits and pieces, as intended.
That meant OxyContin was primed to become a dangerous drug, killing more people than it was saving. In 2010, Purdue Pharma—founded by the powerful, wealthy Sackler family—adjusted its formula, so that when a user attempted to pound the pill into a powder, it was impossible. What should have become a powder instead became a gelatinous mass.
That fundamental change was supposed to help stem the worrisome spike in patients who were becoming addicted to OxyContin. But as Lieber and his colleagues point out in their paper, it had the accidental effect of making heroin a more attractive drug.
“When oxycodone was in the illicit market, the price was about a dollar per milligram,” Lieber explained. “For two pills a day, it came out to about $160 per day.” Lieber said he didn’t have the exact pricing for heroin because of its variability but said “you can achieve the same high for much cheaper with heroin on a daily basis.”
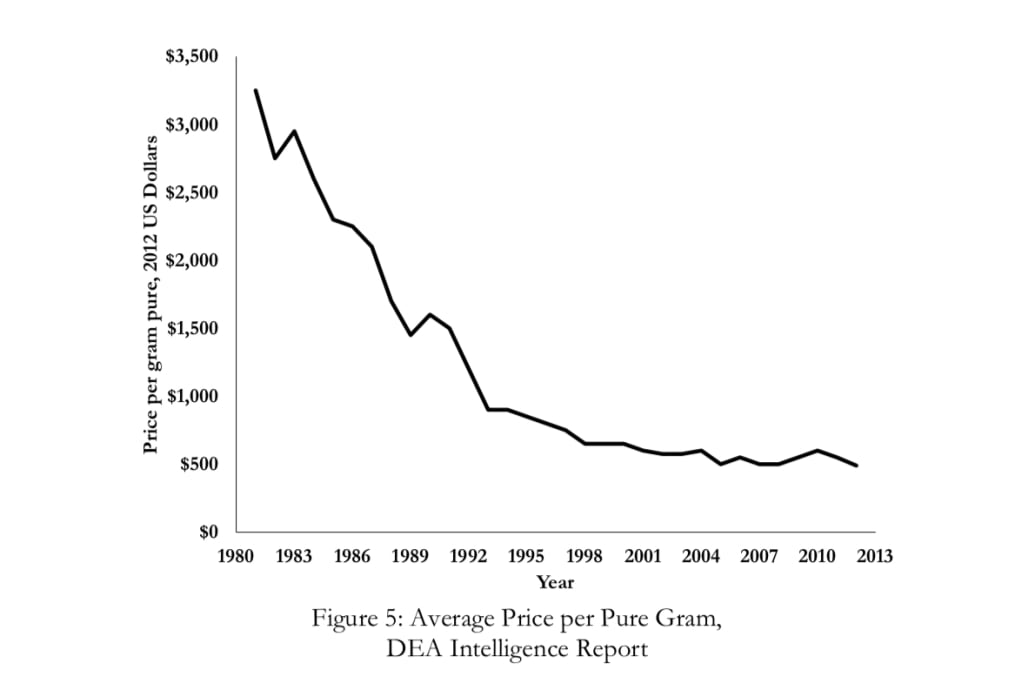
Courtesy Evans, Lieber, Power / NBER
But even those heroin deaths are starting to flatten, thanks to fentanyl. In recent years, fentanyl has become increasingly popular as a substitute for heroin. And that’s something that didn’t escape the notice of Lieber and his colleagues.
That heroin delivered the same high as OxyContin for much cheaper meant it appealed to people across all demographics and socioeconomic classes. In a now frequently cited paper that traced why the mortality and morbidity of non-Hispanic white men in America is climbing—a pattern that is not just worrisome but the exact opposite of what is otherwise happening in every other advanced, industrialized country—Anne Case and Angus Deaton coin the term “deaths of despair.”
Case and Deaton found that the combination of poor health, job loss, and opioid use to ease the stresses of trying to attain a middle-class life without the resources and job guarantees that previous generations found so abundant made for a fatal trio of factors that killed off middle-aged white men across the country—especially white men along the Rust Belt.
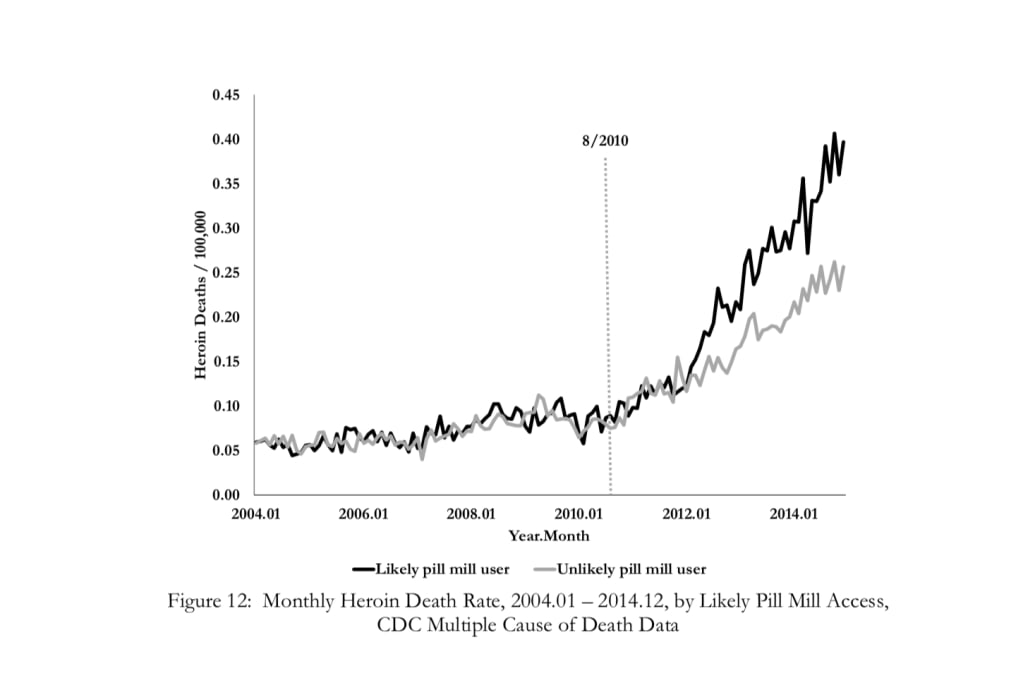
Courtesy Evans, Lieber, Power / NBER
Lieber said the “deaths of despair” pattern shows up again in their data set, with clear spikes in heroin use in states like West Virginia, Kentucky, Indiana, and Michigan. He also said Alaska fell into this camp, despite not geographically falling into what is known as the Rust Belt.
Just last month, the CDC released a report that showed drug overdose deaths had jumped 11.4 percent in the United States between 2014 and 2015, from 46,640 people to 52,404. The vast majority of these deaths—63.1 percent of them, or 33,091 deaths—were due to opioids, with huge increases in deaths from non-methadone synthetic opioids.
“For who’s dying from opioids and who is buying heroin, we didn’t do a specific study. Our data was just not good enough,” Lieber said. But their data was good enough to show that the OxyContin-to-heroin switch was nationwide and that it was bad news for middle aged white men in economically struggling Heartland economies.
In January 2017, Abby Alpert, David Powell, and Rosalie Liccardo Pacula wrote a paper that came to a similar conclusion as Lieber and his colleagues: that the rise of heroin deaths could be attributed to the change in OxyContin’s formula. Other analyses have also hinted at the reformulation as being the possible culprit of the modern epidemic.
Powell told The Daily Beast via email that in general, the team’s paper agreed with those of the new group’s findings. “We found their results generally complementary with our earlier findings,” Powell said, citing “some differences” in categorizations of states and how “exposed” these states were to OxyContin versus heroin. “Our paper showed that the legal supply of oxycodone is correlated with nonmedical use of OxyContin, so both measures should produce similar results… [but] overall, we believe that their paper offers some useful confirmation of our findings.”
Both papers present data clearly indicating that government programs aiming to ease the opioid crisis by pushing for pharmaceuticals to create deterrent formulas, or changing pill recipes so they aren’t so easy to get high off of, is clearly not going to work, Lieber said.
“In theory, this sounds like a good idea,” he said. “But when you have something else that people can switch to, it’s clear that not a lot of people will get benefits.”