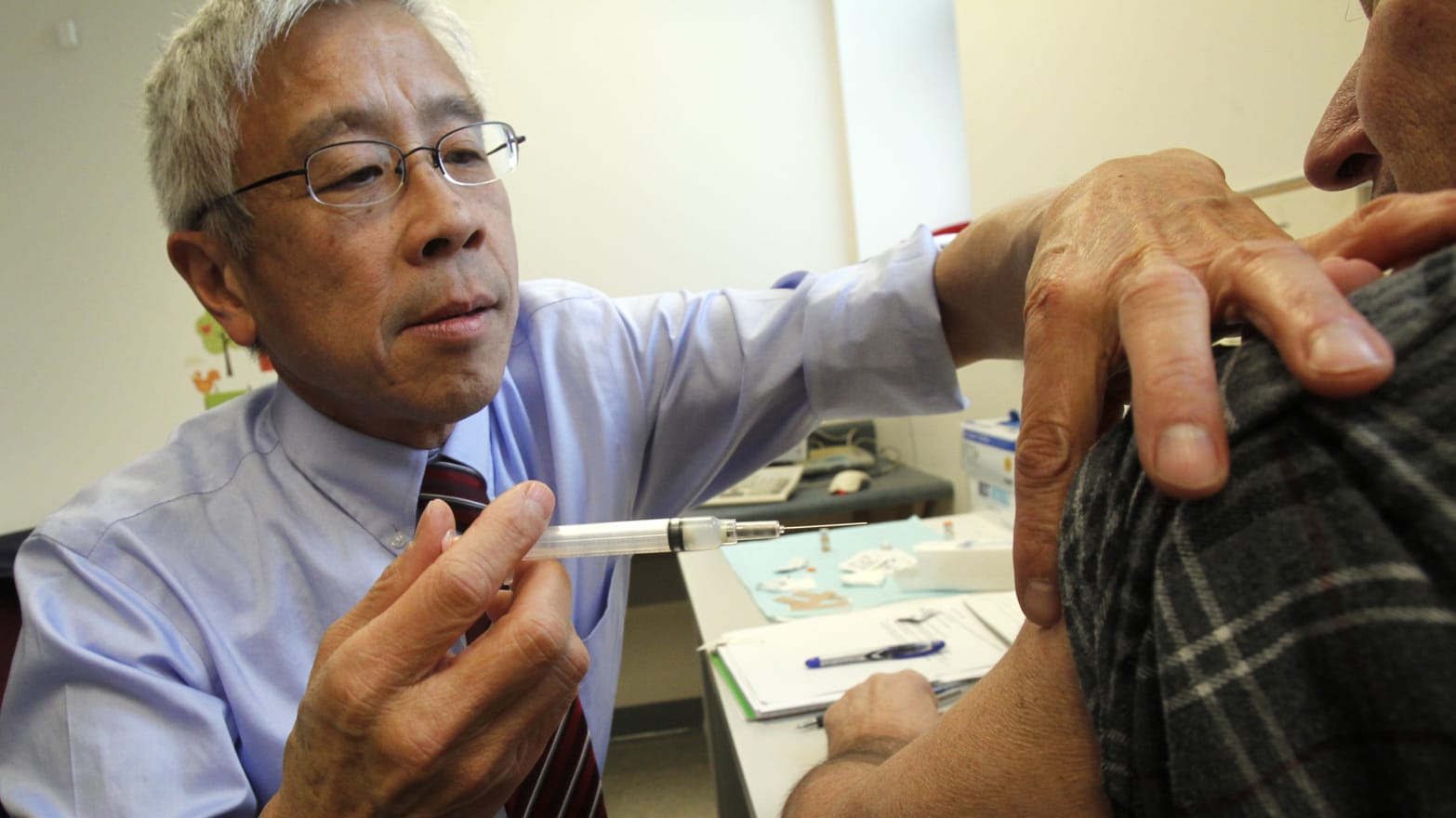
Earlier this month, the New England Journal of Medicine published an eye-catching report, noting that new strains of whooping cough had turned up in 11 patients in North Philadelphia. Since then, dozens of news spots, blog posts, and even resources for doctors have fretted over the emergence of “vaccine-resistant pertussis.”
There’s only one problem: these headlines are all wrong.
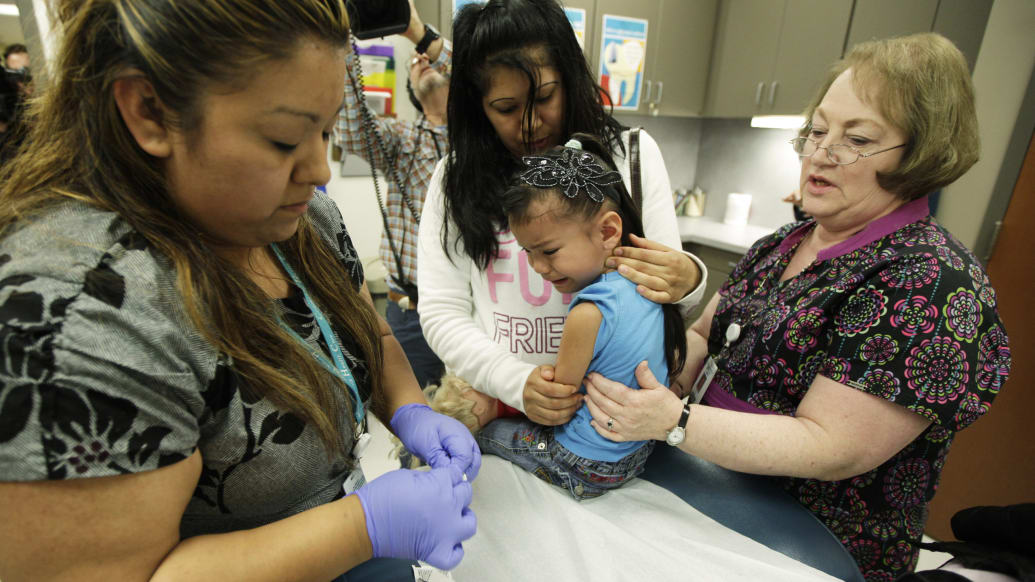
The vaccine almost certainly offers protection against the new strains. The problem raised by the authors of the report is that the protection might not last as long as it would against the older variants of whooping cough, leaving people vulnerable to infection sooner. No one knows yet whether these mutant strains in Philadelphia are circulating elsewhere in the country—or how much they’ve contributed to the national surge in whooping cough cases in the past few years. The protection offered by the current vaccine also wanes more rapidly than researchers once thought. But until someone makes a better version, the best we can do is immunize to the hilt, making the most of the only real tool we have.
To see why the Philly mutants are causing such confusion, some vaccine science is in order. Bear with me. The original whooping cough vaccines, introduced in the 1940s, were a messy soup, made from dead whole cells of bacteria. They were highly successful against a dreaded childhood killer. But they also tended to cause reactions, like high fevers, in some kids. So in the 1990s, the United States and other countries switched to acellular versions, which rely on just a few bacterial components (typically either three or five), rather than whole cells, to stimulate the immune system. These components include a deactivated form of the pertussis toxin (thought to cause the characteristic awful coughing) and a protein called pertactin, which the actual bug uses to attach to the respiratory lining.
The big surprise with the Philadelphia strains, however, is that they don’t make pertactin. In other words, they don’t wave one of the flags that the immune system has been trained (by the vaccine) to recognize and attack. That is probably why so many observers have called them “vaccine-resistant,” or said that they wear an invisibility cloak.
But the immune system can still see the new strains, thanks to the other ingredients in the vaccine, especially the deactivated pertussis toxin. The strains are “definitely not ‘vaccine-resistant,’” as Dr. Alan Evangelista, director of microbiology at St. Christopher’s Hospital for Children in Philadelphia, and one of the authors of the New England Journal paper, told me. The omnipresence of the phrase is disturbing, too. As Tom Clark, a pertussis expert at the Centers for Disease Control and Prevention, put it: “We don’t want people to start believing that the vaccine doesn’t work.” It does.
Still, the vaccine’s protective effect may wear off faster when it comes to the new strains. That’s because the longest-lasting benefit may come from the ability to recognize pertactin, according to Jan Poolman, the global head of bacterial vaccines for Janssen pharmaceutical companies. (In technical terms, antibodies to pertactin seem to remain at higher levels in the bloodstream for longer than antibodies to pertussis toxin or other vaccine components.) So it’s possible that four or five years after vaccination, a strain that doesn’t announce itself with this protein might be harder for the body to combat. Clinical studies are needed, however, to know for sure.
The biggest question, of course, is how much this matters to recent epidemic levels of the disease. No one knows yet whether pertactin-negative strains are circulating widely in the U.S., beyond Philadelphia. It seems likely that they are, especially since other such strains have been found in France, Finland, and Japan. But the national surveillance data are not yet in. Researchers at the CDC have also begun to probe their collection of the pertussis-causing bacteria. So far, they have analyzed 666 samples, gathered from 1935 through 2009, and have not found any that lacked pertactin, Dr. Clark told me. But they’re still working on more recent ones. (The strains identified in the New England Journal paper were from 2011 and 2012.)
Waning immunity to the vaccine is already a hot topic, quite apart from the new strains, as experts try to explain surges in the disease. They note that the acellular vaccine does not offer as long-lasting protection as the old whole-cell versions did. Which appears to be why children who received acellular shots as babies, starting in the late 1990s, have been especially hard-hit in recent years. (Children get shots at 2 months, 4 months, 6 months, 2 to 3 years and 4 to 6 years of age. But as they reach older childhood, their risk of pertussis seems to steadily climb, until they receive their 11- to 12-year-old boosters. Teenagers are also at risk, as are adults.)
An influx of pertactin-negative strains might or might not be making matters worse, by making even vaccinated people vulnerable to disease more quickly than they otherwise would be. But either way, our best bet for now is to roll up those sleeves.