The only thing more terrifying than the spread of Ebola is when the hemorrhagic fever spreads to pregnant women. It’s not just a likely death sentence for the mother and fetus. It also can ravage entire public health systems meant to bring children safely into the world.
Part of the gripping story of Thomas Eric Duncan, the first person with Ebola diagnosed in the U.S., includes a detail about how he likely contracted the disease. According to reports, he probably became infected four days before flying to the U.S. after helping a friend and neighbor who was dying from Ebola.
Because of intense interest in how Duncan got to the U.S. and whether doctors in Dallas handled the diagnosis in a timely fashion, the most poignant detail in the story has been mostly glossed over: The source case, a 19-year-old woman named Marthalene Williams, was seven months pregnant. A few hours after the prolonged exposure to Duncan, Williams and her fetus died of overwhelming Ebola infection.
Little is known about the effect of Ebola on pregnancy, but what we do know seems particularly grim. Only one study, a 1999 report from an outbreak in the Democratic Republic of the Congo in 1995, has examined the condition. Belgian and local researchers reported on the outcomes of 15 pregnant women who were among the 105 women who developed the disease. Of these, 14 (96 percent) died. As did their fetuses, including those of the four women who were in their last trimester.
The cause of death for many was bleeding—not a surprise given the intense blood vessel richness of the placenta and the pregnant uterus. Combining that dense mat of small arteries and veins with a disease that is among the hemorrhagic fevers is asking for trouble, even with a young and healthy group of patients. Indeed, all 15 women in the study had severe bleeding and, in addition to the death of the mother, many miscarried before perishing.
The extremely high death rate is surely alarming. By comparison, the overall death rate in those earlier years, before the utility of supportive care with IV fluids was fully appreciated, was 77 percent—a statistically trivial difference. A recent 2014 review by the Centers for Disease Control and Prevention (CDC) of risk to obstetricians from Ebola viruses also considered the issue and leaned on the same 1999 data, repeating the same sad news and adding the equally grim fate of the fetuses.
Now with a death rate of about 55 percent for the more than 7,000 cases diagnosed to date, the survival differences, if present, will stand out more sharply and significantly. It is uncertain, however, whether pregnancy is a condition recorded by local health authorities, who are busy with a thousand other tasks. In other words, we may never know the exact increment of increased risk for pregnant women who contract the infection.
But a second risk to pregnant women has emerged. A recent flurry of attention has been aimed at the collateral problems to anyone with a medical condition in Ebola-strapped countries, including those without infection: the deleterious impact of packed hospitals, filled beds, and overwhelmed, frightened doctors and nurses. This lack of predictable prenatal care may have a larger public health impact than the deaths of so many during this frightening, historic epidemic. This is a testament to both the remarkably salutary effect of prenatal care, even at its bare-bones most simple, and the fragile, now- tottering health care systems of the three countries who may lose an entire generation should the disease not be stopped.
Arthur Pratt, a Sierra Leonean filmmaker working in Freetown to spread education about Ebola, came face to face with this immediately. In August, with all health centers closed to non-Ebola patients, he was forced to drive his eight-month pregnant wife to her mother’s village, hours away. “A lot of women are having to give birth in the house now,” said Pratt in an August interview. “All of the hospitals are closed. They have nowhere to go.”
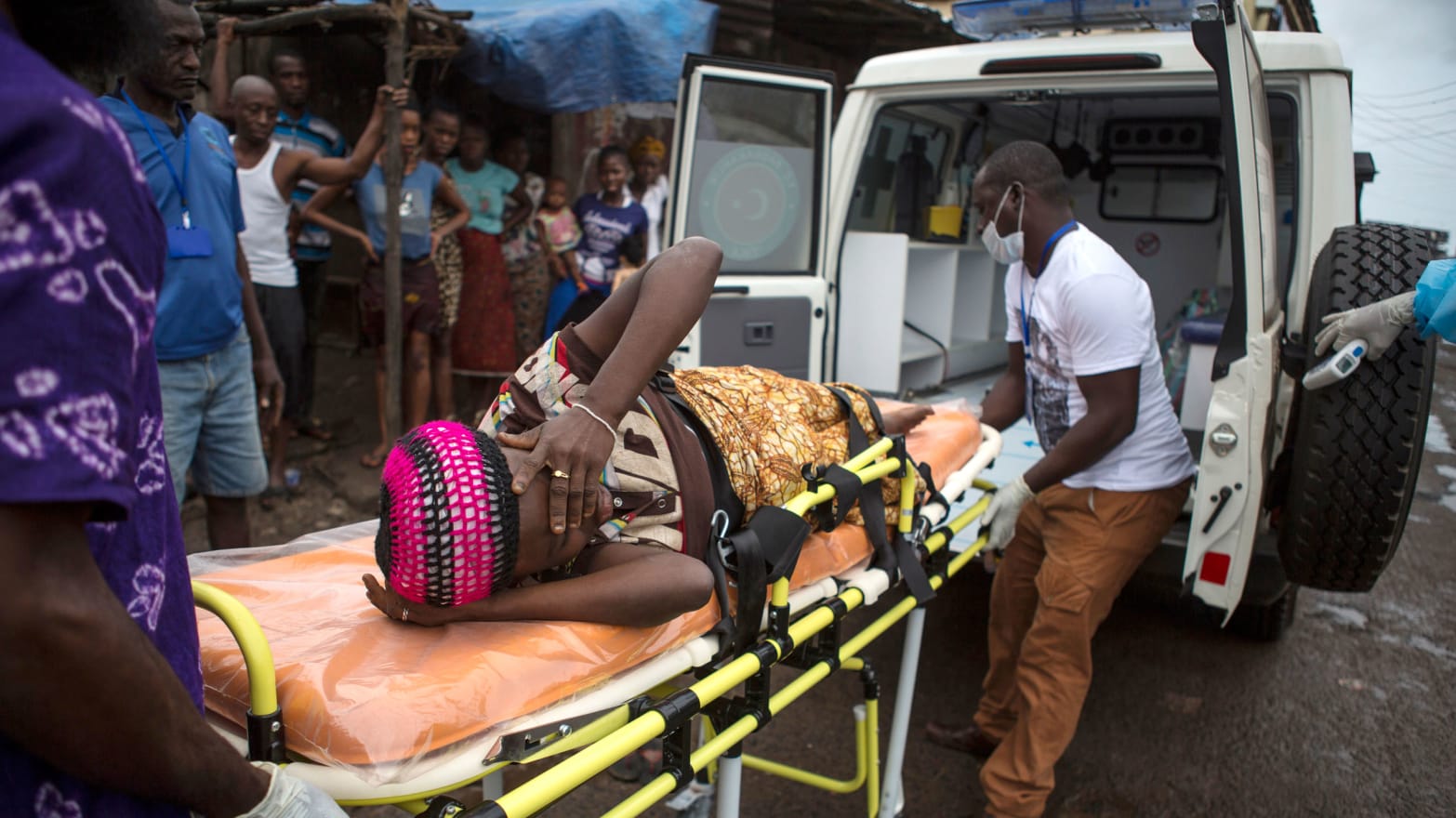
In August, the United Nations Population Fund reported that ambulances in Bong, one of Liberia’s biggest cities, were being used strictly for Ebola patients, and that the two major wards of JFK Hospital used for childbirth closed. “As a result of the outbreak, there has been an increase in pregnant women dying from preventable causes, including ante-partum and post-partum hemorrhage, ruptured uterus, as well as hypertensive disease,” said Dr. John K. Mulbah, chairman of the obstetrics and gynecology department at the University of Liberia.
According to a report from the World Health Organization, pregnant women most often die in childbirth from five major complications: hemorrhage, infection, unsafe abortion, eclampsia (very high blood pressure leading to seizures), and obstructed labor. Abby McDaniel, a child survival specialist at IRC, spent years in Liberia working to build up the country’s primary care health system to prevent and manage these complications.
“We would work with communities and community-level Traditional Trained Midwives to make sure women were delivering at health facilities where they could deliver more safely and receive ambulance referrals to Basic and Comprehensive Emergency Obstetric and Neonatal Care centers for complications arising during pregnancy,” McDaniel said. At the time of her arrival in 2011, many of the facilities in Liberia lacked even a single midwife, let alone trained OB/GYNs. During McDaniel’s time in Liberia– some estimated that there were only six national OB/GYNs in the entire country, many of whom working concurrently in administrative roles.
By the time McDaniel left Liberia in 2013, the country’s health care system had come a long way. “We worked with Liberian training institutions and the Ministry of Health to recruit, train, and place health professionals capable of providing appropriate levels of support. We also worked with the county- and district-level ministry of health officials to ensure ongoing on-the-job training and supervision of these staff. ” she said of beefing up the maternal care program. “We wanted to reinforce the fact that we were there to help these women.”
When Ebola began spreading through Liberia, these new lifesaving programs were abandoned. “It’s heartbreaking to see that the primary impact of Ebola isn’t just the people who contract it, or even the health-care workers,” says McDaniel. “It has completely crippled the health care system—brought it to a halt. You’re talking about facility-based deliveries, pregnant women who need help, children getting born who need care. It’s so discouraging.”
Dr. Emmanuel d’Harcourt, the senior health director of the International Rescue Committee, has seen the severity of this situation firsthand. While on a recent trip to Liberia, he spoke with a doctor in an Ebola treatment unit about the issue. “When a typical patient comes to the staff at the Ebola treatment center, they have real hope,” said d’Harcourt. “With a mortality rate at about 60 percent, there is a great chance that they will live,” he continued. This is not a feeling that is shared for those who arrive to the centers with child. “Doctors and nurses who have been working on the Ebola ward have told me that, from what they have observed, women who are pregnant are a lot more likely to die. When they arrive, there is not the same hope.”
In d’Harcourt’s eyes, the abandonment of pregnant women in this epidemic is particularly painful. “It’s heartbreaking on so many levels,” he said. “They were already taking a risk in a country where a pregnancy isn’t always a safe thing—with a thing that would bring a lot of joy to a lot of people.”
The trend, he explained, extends further than West Africa. “There are so many ways we as a global community have failed pregnant women, who play such an important role in society,” he said. “We all have a responsibility, in a way, for their safety and we have failed in so many ways.”