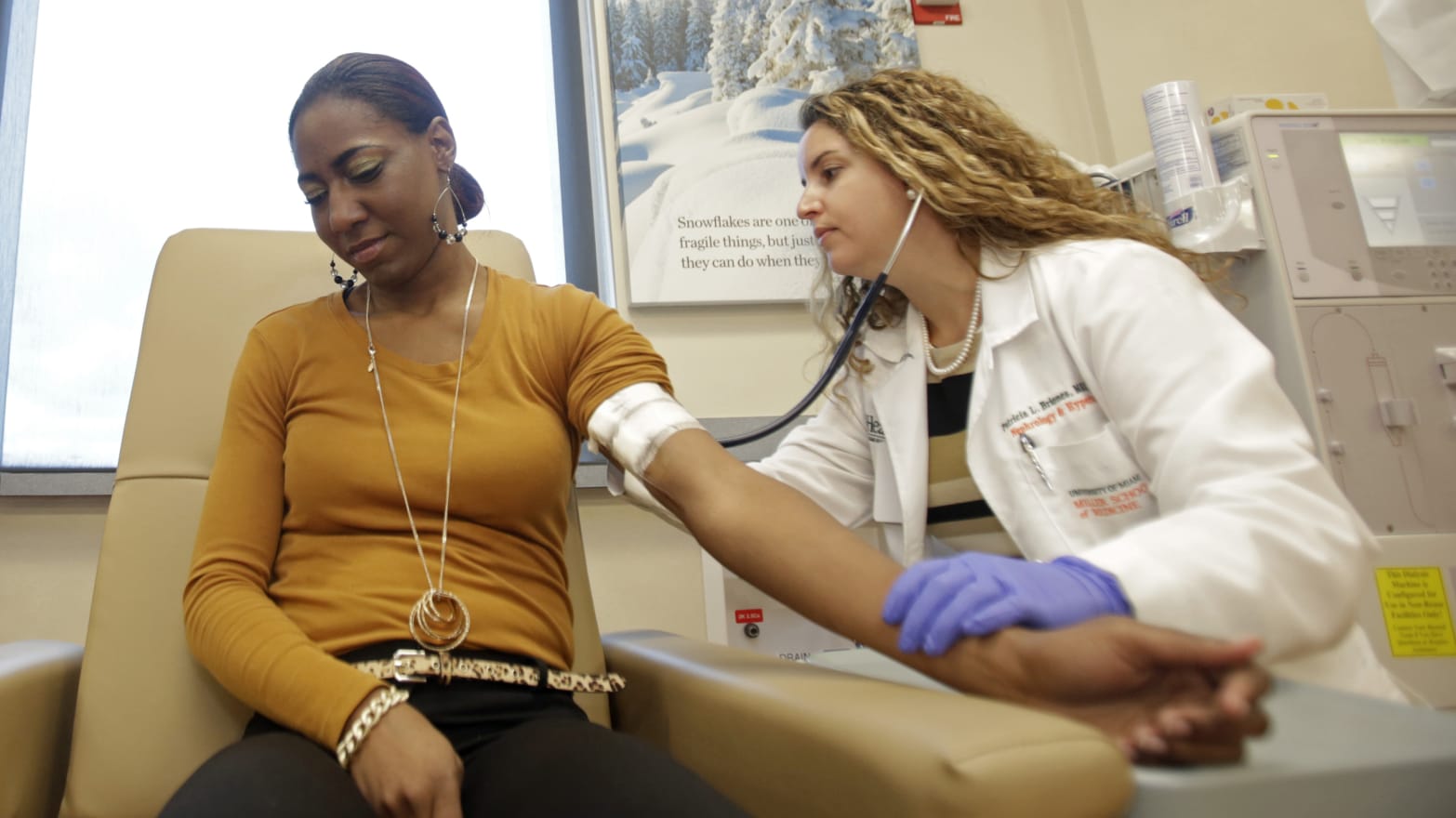
I have worked with nurse practitioners (NPs) ever since I graduated from medical school: during residency, when I did an additional fellowship, and at both my previous and current practices. These experiences have included caring for very premature infants, treating children with cancer, managing the reproductive health of adolescents, as well as primary-care pediatrics. On a few occasions I’ve had to transfer an ill child to another facility, and sometimes the medical provider who arrived with the ambulance to assume care was an NP. I was always grateful when they got there.
With an exception or two, these NPs have been wonderful to work with. (Show me a profession that doesn’t have a few sub-par members. Lord knows I can list plenty of clunker physicians.) I have the utmost respect for them as colleagues, and value the work they do immensely. When I have a patient with a weird rash I want someone else to look at, or when I feel like running a treatment plan I’ve put in place by another person, I am as apt to grab one of the NPs in my office as a physician.
It has been projected that tens of thousands of additional primary-care physicians will be needed to meet the nation’s health-care demands within a little more than a decade. While increasing the number of residency slots has been proposed as one solution to this problem, allowing NPs to practice with minimal restriction is another possible option. Though many states permit NPs to practice without physician supervision, the majority—including the state where I practice—put some kind of restriction on the care NPs can deliver autonomously.
I am wholeheartedly supportive of allowing NPs to practice without physician supervision. However, not all doctors share my perspective.
In a recent New York Times op-ed, Dr. Sandeep Jauhar lamented New York becoming the latest state to give NPs freedom to practice without oversight from doctors. He cited a study from 1999 that found NPs ordered more tests and consultations than their physician colleagues, and posited that this discrepancy is due to their inferior training and resultant lack of clinical confidence or acumen. He went on to speculate about a two-tiered system in which under-trained and unsupervised NPs would deliver care that is not as good as that delivered by doctors.
I do not believe such a two-tiered system will come to pass. As was mentioned subsequently in a letter to the editor dissenting from Dr. Jauhar’s views, a 2010 report by the Institute of Medicine found clinical outcomes for patients treated by NPs were comparable to those for patients treated by doctors. That finding is entirely in keeping with my own observations of NPs delivering excellent care over the years, both as co-workers and as health-care providers for various members of my family—kids included.
Did I receive more training during residency than the NPs in my office did during their training? Yes. However, they all spent years as nurses on the wards before they went on to become NPs, and surely that experience is worth considering. (When I spoke to one of them about this article, she did express some reservations about NP programs that do not require a minimum of clinical nursing experience for entry.) Further, while the time I spent in the neonatal intensive care unit or on the oncology service was valuable, it has little bearing on the care I deliver as a primary-care physician today.
Dr. Jauhar believes the ability to discern subtleties in clinical presentation and find the occasional anomaly in a sea of normal appearances requires a doctor’s care. I disagree. I believe such skill comes more from experience than training, and would much rather be cared for by a seasoned NP than a physician just out of residency. That isn’t to say that the additional training I received doesn’t add value to certain, more complex patients’ care. But NPs are quite capable of delivering skillful primary care without my looking over their shoulders.
Speaking frankly, I believe Dr. Jauhar’s sentiments and those I have heard from other physicians along the same lines have more to do with protecting the status of doctors than with protecting patients from sub-standard care. To a certain extent I can understand the desire to shore up the public’s perception of our ongoing relevance. Given the numerous pressures that continue to build up around the practice of medicine and the erosion of patient respect for our expertise, it is easy to see why doctors would stridently object to the notion that non-doctors can do the same kind of work that we do.
But NPs are not looking to replace physicians, and nobody is suggesting they start applying for positions where the additional training a physician receives is clearly necessary for the provision of appropriate care. Letting them practice without the unnecessary burden of supervision from a doctor will better allow them to fill a gaping void in patient access to medical treatment. Making vague insinuations about their purported inadequacies as providers when there is ample evidence to the contrary is little more than professional protectionism, and is out of keeping with the respect physicians ought to have for evidence-based practices in general.
Nurse practitioners aren’t doctors—nor are they claiming to be. But they are medical providers in their own right, ones who can demonstrably provide quality care. I love working with them, and hope the medical establishment makes progress toward welcoming them as colleagues rather than treating them as competitors.