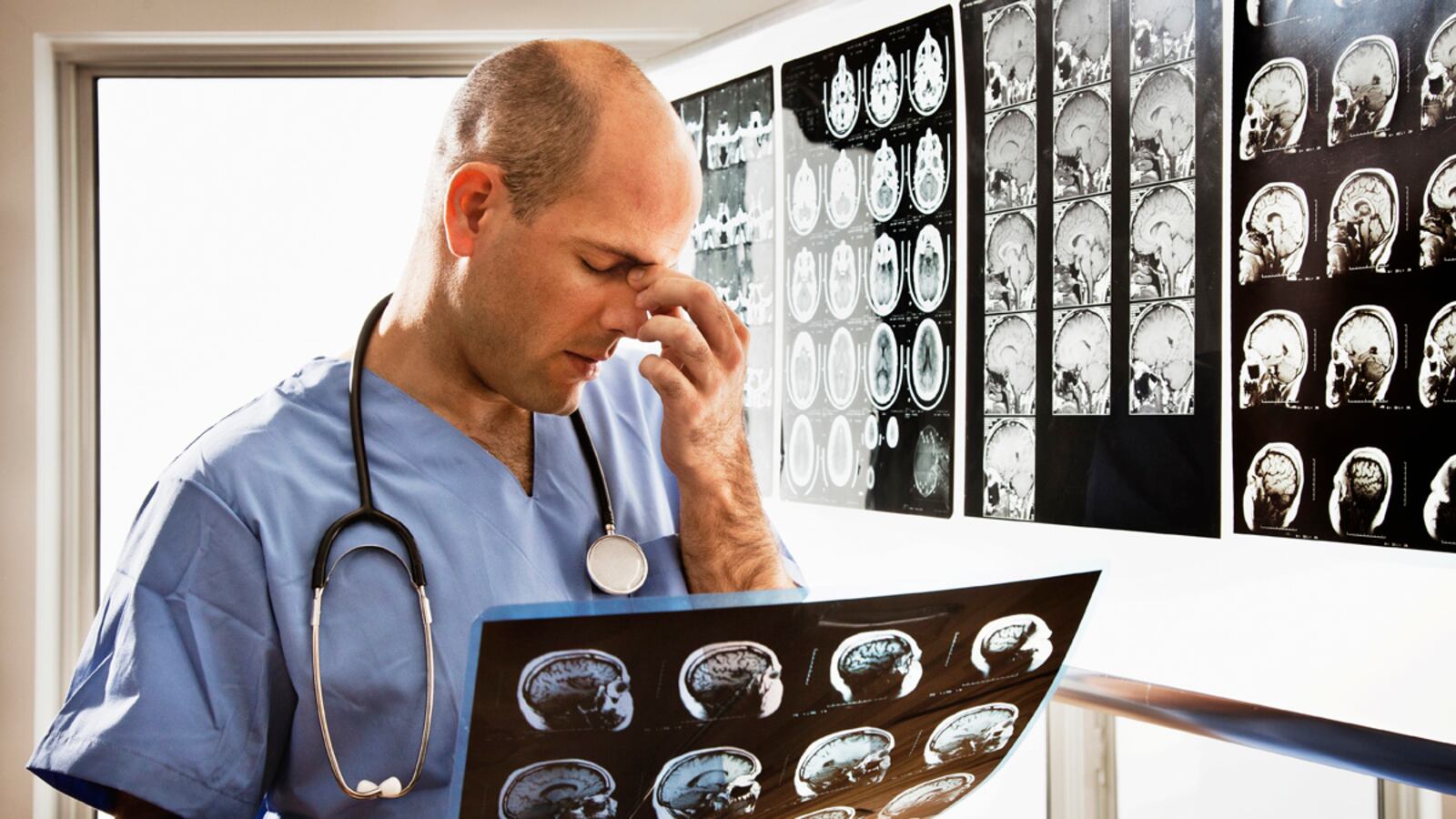
Perhaps more than any other professional group, doctors like to write about their wretched plight. Certainly we have enough room. These days, there are thousands and thousands of print and online medical journals with acres of space for that latest study, whether it is about a gene in the fruit fly, the effect of aspirin on a group of farmers, or best of all, a study about—what else—ourselves.
Therefore, the appearance of a recent article/pity party entitled “Burnout and Satisfaction with Work-Life Balance among U.S. Physicians Relative to the General U.S. Population” comes as no surprise. Doctors have a vast platform to investigate, tabulate, and disseminate just how miserable they are. Furthermore, using the tricks of the trade (and the fact that they own the playing field, i.e., run the medical journals), they can compete against any number of other groups of potentially miserable professionals to see just who is suffering more. (We are, I promise).
Coming up with a measure for misery is always tough; the National Weather Service has perhaps the best-known yardstick which, though understood by no one, is widely embraced: the wind-chill index. People refer to it all the time with toothy glee as a way to convey just how grim the great outdoors looms. For professional misery, aka burnout, there is a less widely known, but well-respected, measure—the Maslach Burnout Inventory or MBI, developed by Stanford Professor Christina Maslach. It examines three “domains” of potential misery—emotional exhaustion, depersonalization (“I am just a number here.”), and thwarted personal accomplishment—in a simple, 22-item questionnaire. The results can quickly be converted to a Solomonic judgment as to whether someone is burnt.
In the study, investigators compared how doctors fared on the MBI, then rubbed it against the results for the general U.S population, that hulking non-physician mass of citizens who were game enough to answer a cold call and respond to the toned-down version of the 22-question barrage (just a few questions long). On the doctor side, they invited 27,000 to participate in the survey, and heard back from about a quarter, raising a worrying issue: were the respondents more (or less) burned out than the three-quarters who opted not to respond? As someone who almost never responds to dopey “We Want to Know How We Did” surveys from hotels or airlines—except when I am extremely annoyed about something—I imagine the responders had a substantially larger bone to pick with medicine, working, and life in general than the silent majority who decided against clicking.
Plus, there was an imbalance between the populations sampled, that old apples-oranges problem that bedevils so many well-intentioned studies.
The non-doctor respondents were significantly younger, more likely to be single and female, and worked many fewer hours than the doctors. And who’s to say that the type of person drawn to medicine isn’t a born whiner, someone who would feel burned out even if he were playing for the New York Knicks. The investigators, decent folk who were very determined to see it through, certainly knew all these limitations, but still thought the kicker—a burnout rate of 38 percent for doctors versus 28 percent for the younger, more female, and less overworked hoi-polloi—was worthy of reporting.
Maybe. After all, is there any real harm in these sorts of “how we doin’” surveys? Burnout is a real problem, with real downstream effects—poor employee performance, higher turnover, clinical depression. I sure know what they’re talking about; there are days, many, and increasingly frequent days, when I am burned or burning—I hate my life or my patients or am convinced they hate me. I can’t believe someone scheduled me for a meeting. Sometimes the painful absurdity of the modern, non-log cabin life (I have to fill out a form for a box of paper clips?) is just too goddamned much. Surely as the Baby Boomers continue to age, we will see even more of these studies from all quarters—the latest incarnation of the generation’s insatiable comparison-shop-till-you-drop addiction: from the best schools to send your kids, to best nursing homes to send your parents, soon it will be a race to determine if you are more miserable than your neighbor.
Burnout surely needs better elucidation—of course people should be treated like people, not interchangeable sacks of potatoes with smart phones and tired feet; and management should do their best to lift morale even when it bites into company profit. But the burnout described in this and so many other articles is not really a malady. We have once again taken a basic, normal human situation—call it crankiness or a bad day or a bad week—that occasionally tips a few people over the edge and pathologized it for the rest of the population.
Burnout joins an already crowded waiting room filled with so many other problems: shyness, restless leg syndrome, provider fatigue, drooping body parts. This expansion of the doctor’s market share has a real consequence—busier doctors who in turn gripe more and write even more articles about their busy-ness and their inalienable right to gripe.