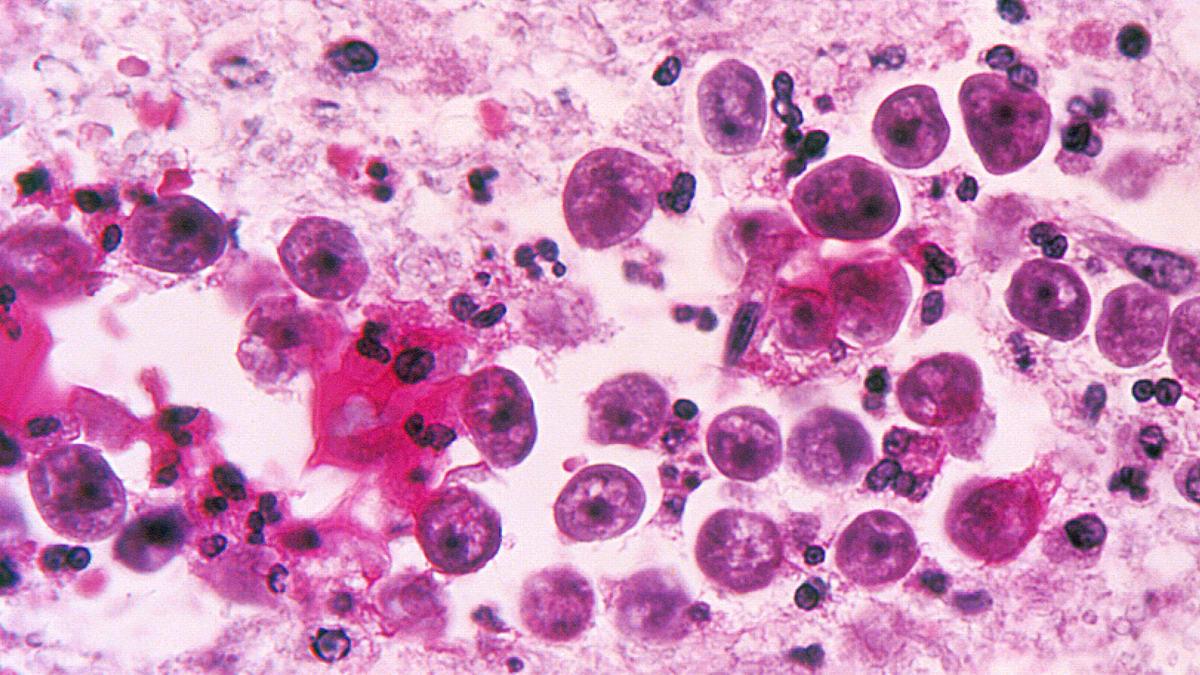
For sheer terror, “flesh-eating bacteria” can’t hold a candle to “brain-eating amoeba.” So it is little wonder that two recent fatalities in Louisiana in people who were killed by the amoeba after they used neti pots to flush their nasal passages with (apparently amoeba-contaminated) water has sinus sufferers in a panic. Until now, the only known cases of infection by the brain-eating parasite Naegleria fowleri have occurred when people swam in warm rivers, lakes, or other bodies of freshwater where the single-celled organism lives. If the two deaths in Louisiana were indeed the result of exposure to drinking water from a chlorinated municipal supply, that is worrisome. “We’re not exactly sure why this tragic situation occurred,” says Jonathan Yoder, a scientist in the U.S. Centers for Disease Control and Prevention’s division of parasitic diseases. “We’re working with authorities in Louisiana to understand the characteristics of the water system that might have allowed this.”
What is known is that the two victims used neti pots, little ceramic devices that relieve congestion and facial pain and pressure by irrigating the nose and sinuses. (Their popularity soared after Oprah featured them on her TV show.) Yet that simple act apparently condemned the victims to a horror-movie death, with amoebae racing up their noses and into their brains, there to munch on gray matter. While that may sound like standard press hysteria, the concern is justified: almost all previous deaths from brain-eating amoebae have come from people swimming or diving in contaminated waters, not dribbling tap water into the nose. And almost all cases of infection by N. fowleri are fatal.
Louisiana’s Department of Health and Hospitals is warning people to use only distilled, sterile, or boiled water in their neti pots, and to rinse the pot after each use. That should kill any N. fowleri in the water. Using water filters with one-micron pores should also work, says Yoder, since the amoeba in all stages of its lifecycle, including spores, is larger than that. Drinking N. fowleri-containing water is, perhaps surprisingly, safe: drinking sends water into your stomach, not your brain. Getting the water into your nose, however, can transport it into the brain. The organism, explains the CDC on its excellent website, “travels up the nose to the brain where it destroys the brain tissue.”
Scientists have some idea of how N. fowleri kills—it causes a brain infection called primary amebic meningoencephalitis (PAM)—but a lot remains mysterious. The organism enters the brain via the olfactory nerve. Once inside, it kills brain cells, but as South Korean scientists reported in July, “the mechanism by which N. fowleri induces ... cell death is unknown.” One possibility is that when the organism comes in contact with the brain’s microglia—resident immune system cells—it causes them to release cytokines, molecules that cause inflammation and cell death. Another is that the organism causes the microglia to release highly reactive oxygen radicals, which tear into brain cells like acid. The amoeba can also kill cells by—to put it bluntly—eating them, or as scientists in South Korea described in 2010, by “a process of piecemeal ingestion of target cells by food-cups.” (Food-cups are formed when the amoeba extrudes part of its protoplasm to form a sort of arm that engulfs the food and then reels it back in to digest.) Watching the amoebae’s effect on cells growing in lab dishes, Thai scientists observed that “the amoebae attached to the cell membrane and ingested the target cells.”
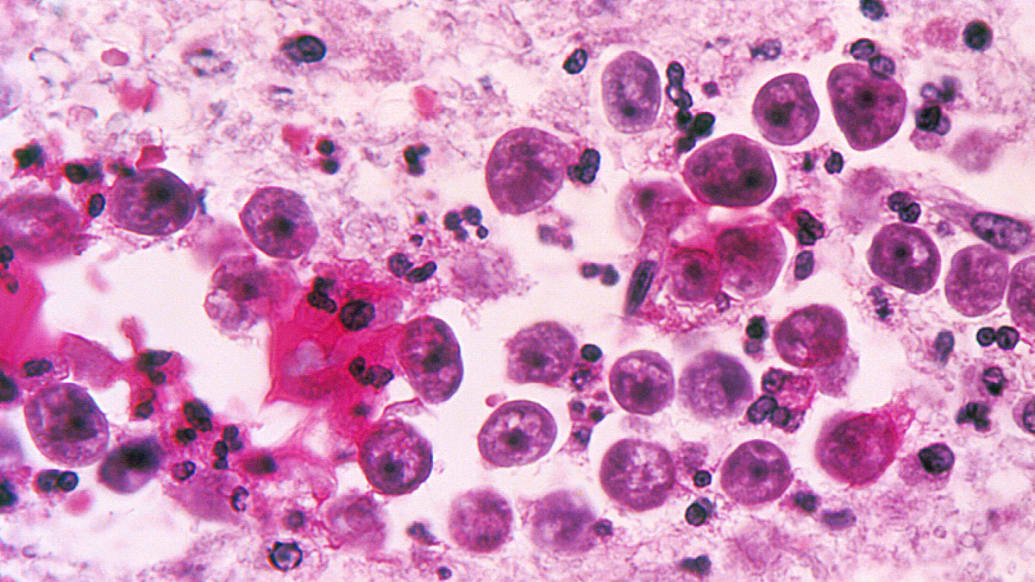
Within a week of infection, the victim develops symptoms akin to those of meningitis: headache, fever, nausea, vomiting, and a stiff neck, which progress to confusion, loss of balance, seizures, and hallucinations. Death almost always follows, usually within 12 days. There is no effective treatment. “Most patients do not survive the infection,” Belgian scientists reported this year.
N. fowleri lives in warm freshwater throughout the world, including “hot springs, lakes, natural mineral water, and resort spas frequented by tourists,” Travis Heggie of the University of North Dakota wrote in a 2010 paper. As Yoder and his colleagues reported in 2010, “N. fowleri infections occur primarily in previously healthy young males exposed to warm recreational waters, especially lakes and ponds, in warm-weather locations during summer months.” The amoeba also lives in warm water discharged from factories, swimming pools that are not properly chlorinated, and, as the Louisiana cases show, drinking water.
Despite this near ubiquity, N. fowleri infections are few and far between. In one 2007 survey of global outbreaks of protozoan parasites, N. fowleri accounted for just 1 in 325 cases. In the U.S., there were just 32 infections in the last decade or so, reports CDC, 30 from swimming and two from a geothermal drinking water supply that was not chlorinated. But infections may be rising. “Previously thought to be a rare condition, the number of reported PAM cases is increasing each year,” said Heggie.
Not all scientists agree with that, but two things are clear. First, the Louisiana cases seem unrelated to swimming; if treated drinking water now poses an N. fowleri threat, that is both new and alarming. Second, says Yoder, the amoeba’s “climate range is changing. In 2010 we had a case in Minnesota, and this year we had one in Kansas, states where it had never been seen before. In Virginia, we just had the first case since 1969. That may be due to climate change,” with N. fowleri able to live in more northerly climes as the world warms. Regardless of the cause, “it’s a concern that we’re seeing cases in places that never had them before”—and that in addition to swimming, the threat of brain-eating amoeba now comes from shooting warm water up the nose.