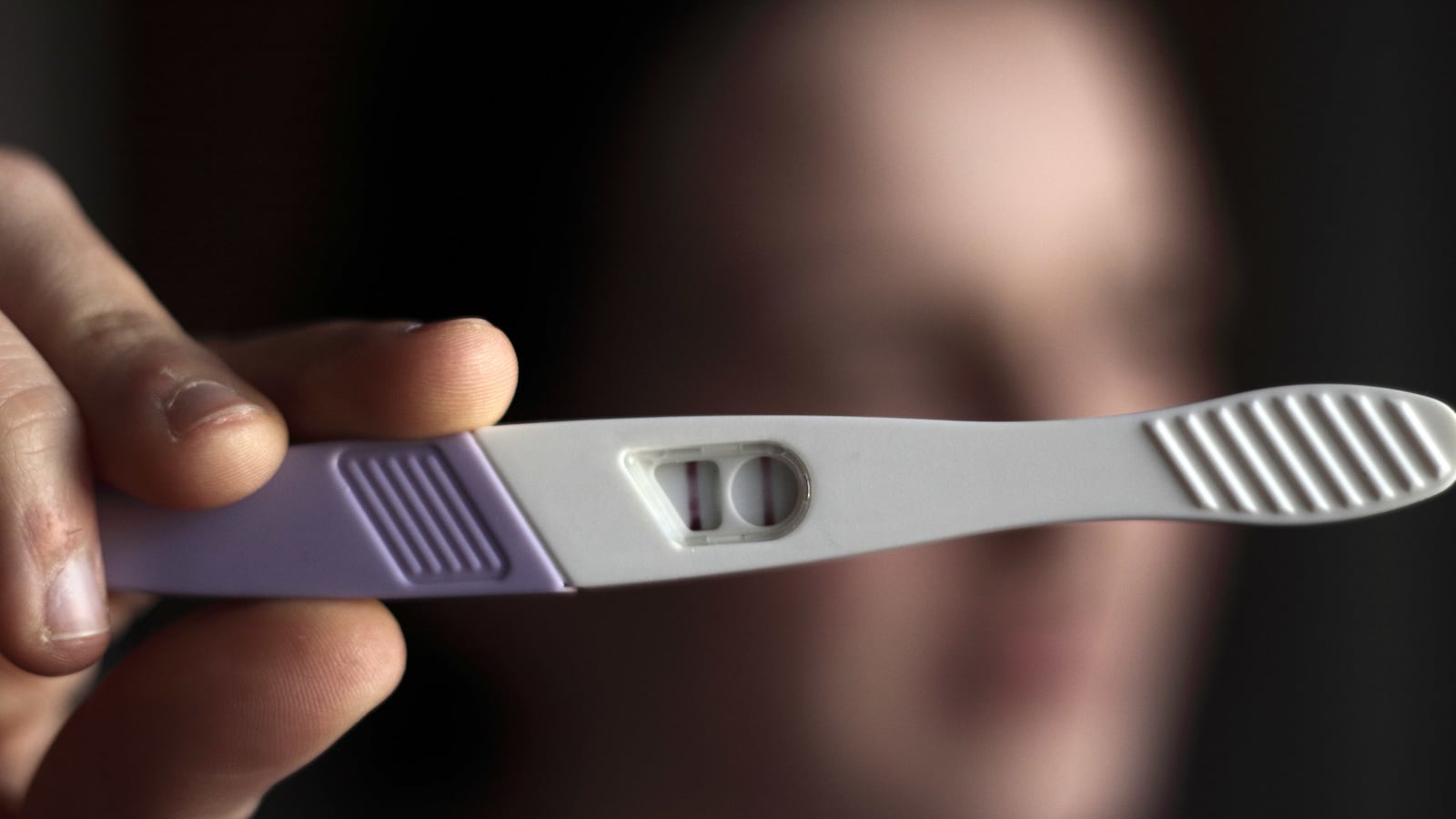
Pregnancy test dispensers will soon be affixed to 20 bar bathrooms in Alaska for a noble cause—to educate women about the dangers of Fetal Alcohol Spectrum Disorders, Fetal Alcohol Syndrome (FAS) being the most severe and easily diagnosed. Alaska’s population is ripe for this experiment, as alcohol consumption, binge drinking, and FAS rates there are among the country’s highest.
The discreet dispenser’s tests are free, courtesy of a two-year, $400,000 government program that will track vends and chart the effectiveness of anti-drinking campaigns aimed at Alaskan women of childbearing age—who are 20 percent more likely to binge-drink than the average women in other states.
This visceral prod is not an anomaly. Jody Allen Crowe, an educator from Mankato, Minnesota, who has worked with generations of families afflicted with these diseases and their stigmas for 25 years, spearheaded dispensers in bar bathrooms in his home state nearly two years ago. There, women can purchase $3 tests with cash or credit cards.
Like with Minnesota before it, there is opposition to the proposed Alaska program, which sprung from a partnership Crowe forged with Republican state Senator Pete Kelly. Some women would prefer broader access to condoms in public places; and much of the program’s coverage has focused on Kelly rejecting similar measures for dispensing birth control. Others resent being proselytized to by seeming teetotalers.
The program has been called “absurd,” and shouldered judgments for its male-devised provenance. Assumptions that the initiative’s goal is to corral and discipline floozy drunk women prevail: “Bars in Alaska to Offer Pregnancy Tests to Drunk Women,” declared Vocativ. “[A pregnancy test] is ‘probably not on the night-on-the-town prep list of the average American woman,’” wrote Takepart.org.
Twitter’s morality police has lobbed insults at imagined users: “If you need to take a pregnancy test in a bar bathroom you shouldn’t be a parent.”
“Surely there are more appropriate places to take pregnancy tests [than bars].”
“If you’re in a bar and taking a pregnancy test clearly you’re already wasted.”
“In our field any discussion is better than no discussion,” Crowe says of such smears.
FAS occurs relatively infrequently, between 0.2 and 1.5 cases per 1,000 births, according to Centers for Disease Control and Prevention data, and slightly more by other counts. But researchers like Edward Riley, who studies the effects of alcohol on children’s brains at San Diego State University, says not only are FAS cases on the rise, but behavioral disorders caused by fetal alcohol exposure are rampant and underdiagnosed. They are tougher to peg, he says, because they can function like problems with motor skills or ADHD, and are often misdiagnosed as such.
“A lot of kids get an ADHD diagnosis and they do meet those diagnostic criteria, but the cause of the ADHD is the alcohol they were exposed to,” Riley says.
The connection between alcohol in utero and behavioral disorders can elude doctors, and maternal alcohol use histories required to make a diagnosis can be difficult to pin down. An FAS diagnosis is simpler, Riley says, because facial modalities like small eyeholes and a thin upper lip are near-instant signifiers. FAS can and has cost states, like Alaska, millions per child in medical bills.
Another hurdle for educators is that the behavioral disorders associated with prenatal alcohol exposure have yet to be officially classified. Neurobehavioral Disorder Associated with Prenatal Alcohol Exposure is for the first time mentioned in the Diagnostic and Statistical Manual’s 5th edition published in 2013, but just in the appendix, citing more research is needed before a full-fledged entry is warranted.
Some scientists assert there are three times as many cases of Fetal Alcohol Spectrum Disorders than FAS cases. Still, because researchers do not know which women are sensitive to alcohol, or what factors determine fetal reactivity to it, many doctors as well as the CDC, the American College of Obstetricians and Gynecologists and the Surgeon General claim there is “no safe amount” and therefore recommend the conservative tact, which is to drink nothing at all.
And yet, pregnant women do drink. Many have undoubtedly read the several recent studies that found moderate drinking presented no risk to children, including two out of the United Kingdom and Denmark. The United Kingdom Department of Health discourages drinking during pregnancy, but says if women choose to drink they should limit themselves to “one to two units of alcohol once or twice a week” and avoid “getting drunk.” Plenty of American doctors do not discourage pregnant patients’ habitual glass of wine each night, especially after the completion of the first trimester, when the most critical fetal formations have taken place.
Those most likely to drink during pregnancy are actually white, college-educated, and middle class, according to recent findings out of the UK. Binging on how-to baby books and evangelical pregnancy tomes does not preclude the nightcap in a culture that positions drinking alcohol as inherent to being a socialized adult. It makes sense, then, that the pregnant women most likely to drink are not poor and uneducated, but women likely to have wine with dinner and read recent scientific findings: 35-44 years old, white, with comfortable incomes and college degrees.
“It was good wine—I never thought of myself as an alcoholic,”’ is a line Kathleen Mitchell, vice president of the National Organization on Fetal Alcohol Syndrome (NOFAS) says she hears often from mothers whose children suffer from prenatal alcohol exposure problems.
Anecdote and family history are powerful influencers. Fetal alcohol syndrome was only first identified in 1973, and many pregnant women before that time and after it still took their scotch before dinner and wine during it, not to mention smoked cigarettes, all during pregnancies. Many of us imagine that our parents, and we, too, “turned out fine.”
And yet, we may not be all fine, according to Riley. Alcohol intake during pregnancy was said to be “the leading preventable cause of mental retardation in the United States,” in a Harvard Medical School report. Crowe likens knowledge about the damages of fetal alcohol exposure to the early days of car seats; when they were invented nobody knew to use them, now everyone does. “We’re at the very beginning stages of preventing prenatal exposure to alcohol,” he says.
As public debate continues and the science crawls forward, Crowe’s hopes his pregnancy test dispenser effort will work more quickly on the ground, where some 50 percent of American pregnancies are unplanned.
Despite appearances, Crowe admits that the bar bathroom dispensers aren’t likely to reach chronic alcoholics, who he admits aren’t his target, while they very well may be Alaska’s. Teens facing unplanned pregnancies are his real target. Pregnancy tests are a popular shoplifted good, hence some Alaska machines will land in “bar and grill” spots for those underage to reach.
“The goal of the entire initiative is to expand access to pregnancy tests. But placing them in bar restrooms gets the most attention,” Crowe says.