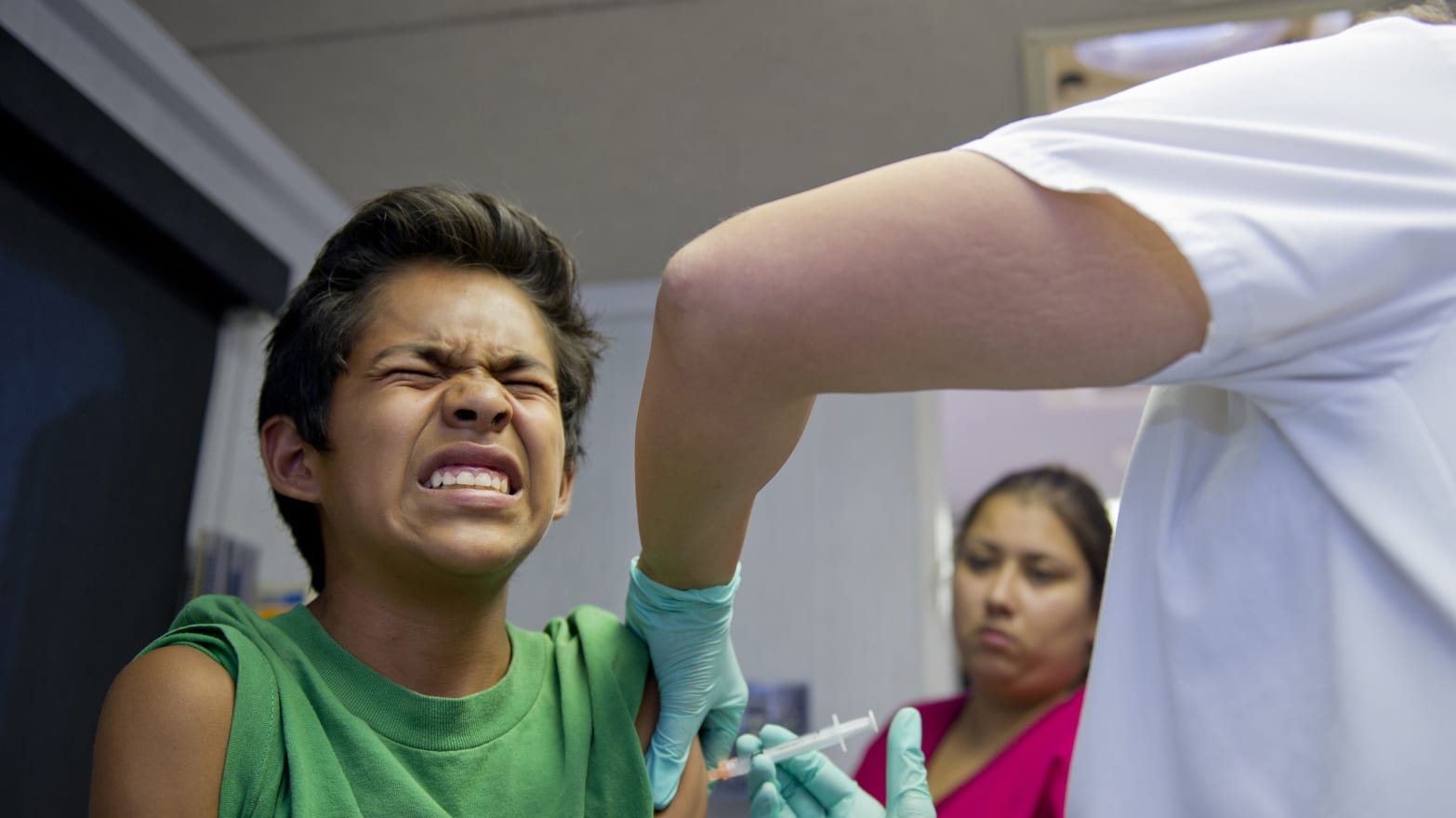
Between 1989 and 1991, the U.S. was in the throes of an unexpected measles outbreak that spread over 49 states, sickened more than 55,000 people, and claimed over 100 lives—mostly children.
Unlike the current anti-vaccination movement driven mostly by middle-class, college-educated, white women, these cases were concentrated predominately in poor, urban places and the virus’ victims were mostly Black and Hispanic.
As Richard Krieg, Chicago’s health commissioner, said at the time, “When mothers have to worry about money for food, it’s understandable that they don’t get immunized.” One dose cost about $16. Congress funded the Center for Disease Control and Prevention’s (CDC) Vaccines for Children (VFC) program, which provided free vaccinations to kids on Medicaid and those without insurance.
In the twenty years since the VFC’s 1994 implementation, The CDC estimates in a report released Thursday that for the 78.6 million children born since 1994, the country’s immunization program has prevented 322 million illnesses (roughly four per child) and 21 million hospitalizations, and saved 732,000 lives. Vaccinations, the agency reports, have also saved the U.S. $295 billion in direct costs and $1.38 trillion in total societal costs. The vaccine program stopped 70 million cases of measles alone.
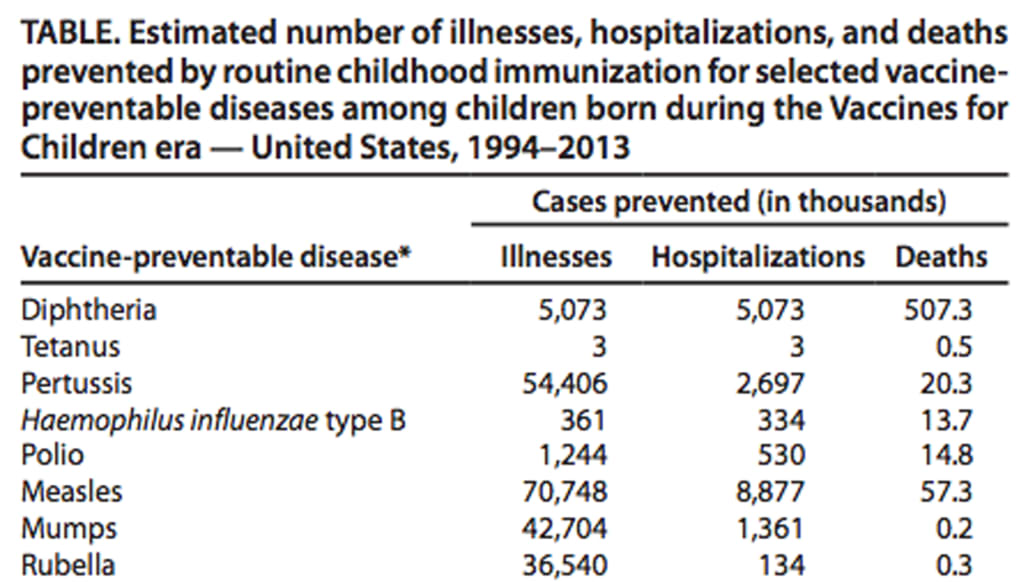
The findings should be a reminder of the ongoing threat of disease and should serve as a wake up call for parents for the importance of childhood vaccinations, CDC Director Tom Frieden said in a call with reporters.
To come up with their estimate of coverage and impact in the post-VFC era, researchers used data on children aged 19 to 35 months from several nationwide surveys that relied on both parental recollection of vaccines and provider reports.
In addition to the success of the original program, the CDC report notes that the five new vaccines that were added to the routine infant schedule since 1995—varicella, hepatitis A, pneumococcal disease, influenza, and rotavirus—have increased the number of diseases prevented to 14.
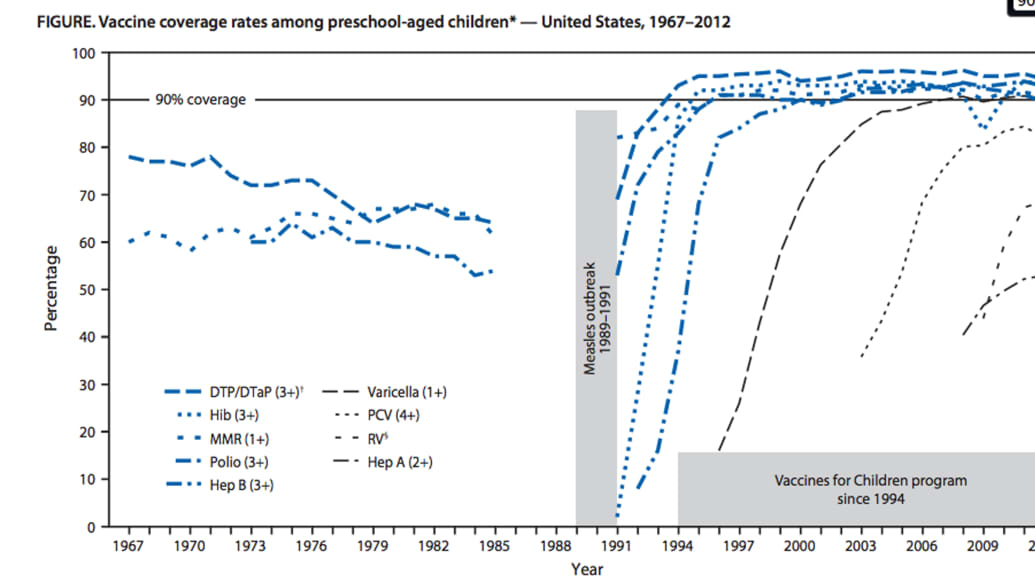
Vaccination coverage has remained near or above 90% for most vaccines, but measles has gotten off to an early and active start this year; 129 cases have been reported from 13 states—the most reported in the first four months since 1996. California (58), New York City (24), and Washington state (13) have seen the majority of outbreaks, defined as three or more related cases.
The 90s outbreak was a result of poor people missing out on vaccines. Today’s outbreaks “are the result of opting out,” Assistant Surgeon General, Dr. Anne Schuchat said on the call. She noted 84 percent of the recent cases were not vaccinated or didn’t know their status. Of the unvaccinated, 68 percent had personal belief exemptions or opted out.
The most at risk from measles, she noted, are infants too young to be vaccinated. “We need clinicians and parents to do their part,” she said.
Schuchat also commented on celebrities like Jenny McCarthy and Kristin Cavallari who have been vocal in their vaccine skepticism.
“Celebrities do get a lot of attention, but the most important influence are their clinicians,” she said. With less than one percent of toddlers receiving no immunizations, she said, “vaccinating your children is still a social norm in this country and we think that’s a good thing.”