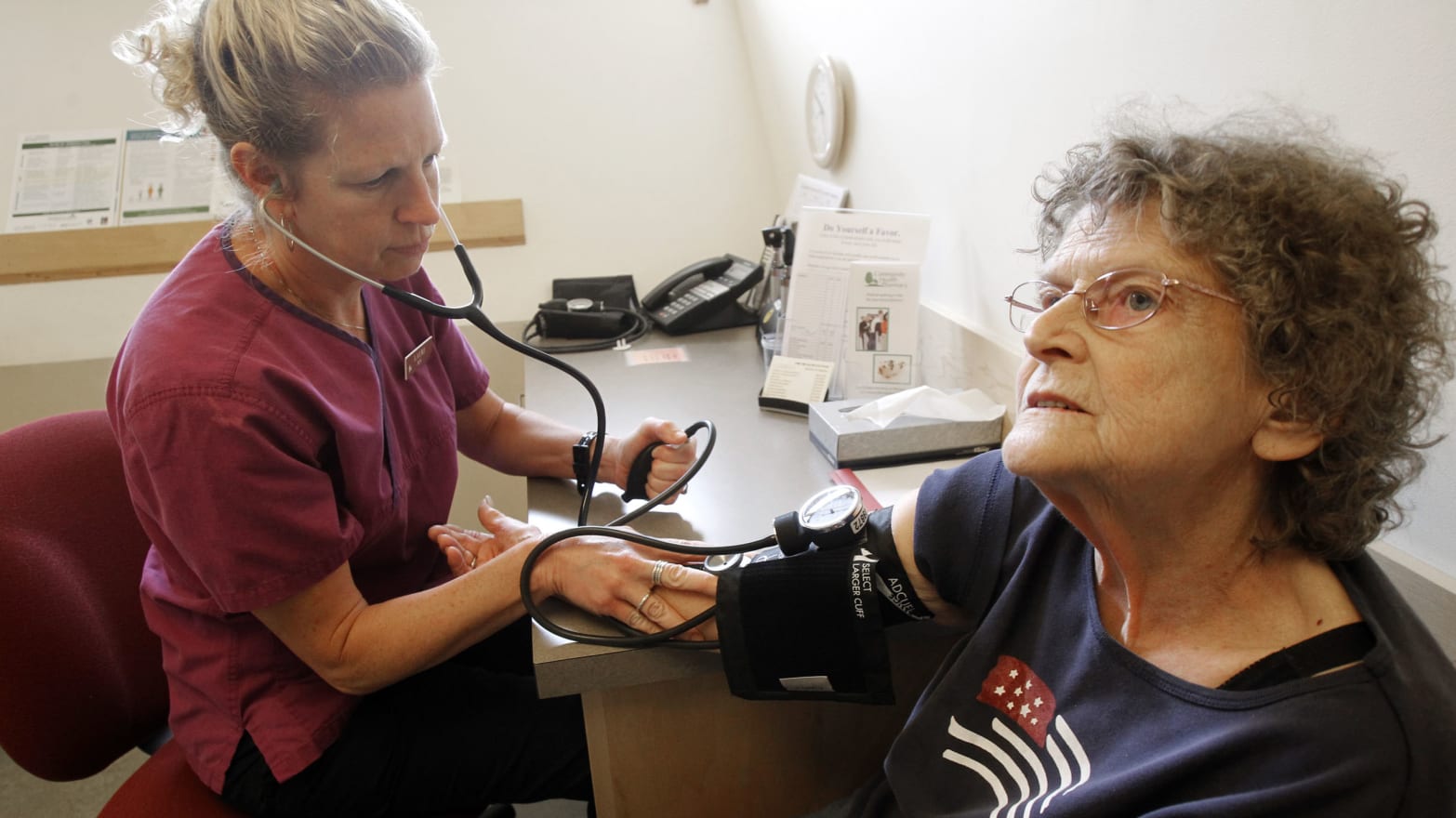
After more than two weeks of dysfunction, it is clear that the rollout of the $400 million federal health-care exchange at HealthCare.gov has been an unmitigated disaster with no end in sight. Enrollment is far lower than hoped for, projected, or needed, in part due to a cascade of technical website design and testing failures.
The good news for the ACA is that the conventional wisdom now being adopted is that the 16 states that opted to create their own exchanges are functioning far better. If only conventional wisdom were reliably true.
Take Maryland, for example, the would-be poster child for the success of the ACA with the unwavering support of Gov. Martin O’Malley and the majority of citizens in the solidly blue state. Two weeks into the launch of their state exchange, a whopping 1,000 people had enrolled through the state’s online portal that is riddled with “glitches” that likely won’t be resolved until late November or early December.
But maybe Maryland just did a lousy job. What about a smaller state, one that overwhelmingly supported the president’s election and reelection, is progressive in its politics, and even had a vibrant and extensive state-run health-care program already in place prior to the ACA? That would be tiny Vermont. Surely with its Democratic governor and Democratic and Socialist senators, it can serve as a laboratory for Obamacare implementation, leading the way through the darkness of those “glitches.”
But, alas, not so, at least not yet. The reality is that Vermont’s health-care exchange website may be even a bigger mess than the federal-run HealthCare.Gov. And health care in Vermont may be headed for a unique train wreck due to its efforts to become the first state in the country to implement a single payer plan.
One of the president’s key selling points of the ACA was the promise that if you liked your plan, you could keep it. We’re learning that’s often not the case as Obamacare is implemented across the country. And in Vermont, there has been no pretense of such assurance.
As of January 1, 2014, in Vermont, the ability for individuals or employers with 50 or fewer employees to purchase health insurance from private insurance companies ceases to exist. As for policies already covering those businesses and individuals? Those cease to exist, as well. In other words, in Vermont, a good percentage of its population will have no choice but to buy health insurance through the state exchange.
But despite the urgency of getting the exchange launch right and the givens that should make it easier rather than difficult—small state, high rate of literacy, 98 percent English speaking—Vermont’s website seems as bad or worse than the federal system. I’m not a Vermont resident, but I have been in the past and still spend a lot of time in the state. In the past week, I’ve spent hours on the state’s health-care system and have experienced nothing but a series of maddening problems reminiscent of computer life 15 years ago. On a half-dozen occasions I’ve fought my way through the system to register, only to return to discover the system has no trace of my registration. I expect that each of these visits and each of these “registrations” have been recorded as unique visits and registrations, which could help explain in part the disparity between “visits” and “registrations” versus “enrollments.”
Recognizing the website isn’t working well, the state has increased efforts to register applicants by paper. Adjusting to reality is admirable, but it’s hardly fair to be canceling insurance for tens of thousands of Vermonters and then mandating they buy new insurance through a system that just isn’t working.
With a budget of $172 million to get its exchange up and running, the state is now in the process of spending $2.8 million on public relations and marketing of the exchange. Educating customers about a product that is working makes sense. Spending money to push customers to use a product that doesn’t work is, well, problematic. It’s a perfect example of government doing stuff that just doesn’t make sense in the business world. You’ve had this feeling a million times standing in the DMV.
Vermont now has the fifth highest health insurance premiums in the country, in part because of state regulations limiting competition. There’s no reason to believe that will improve, as only two companies are offering plans under the exchange. At this stage, unsubsidized rates in the exchange have increased considerably. Any models showing a decrease in premiums are based on a high percentage of enrollees qualifying for subsidies. In addition, the viability of that model is dependent on a large number of the young and healthy paying into the system.
Vermont utilizes the “community rating” method to determine health insurance premiums. The intention of this method is to ensure that rates on particular policies are the same for everyone regardless of age or health. That means that a 57-year-old man will pay the same rate for an individual policy as a 27-year-old woman. Good for the 57-year-old man, not so good for the 27-year-old woman. Cynthia Cox, a health-care economist at the Kaiser Family Foundation, explains, “Younger people will have higher premiums in Vermont than they might if they lived elsewhere, whereas older people might have lower premiums than if they lived elsewhere.”
In other words, without a pool of younger, healthier participants, it’s difficult for any insurance plan to survive.
As this great health insurance experiment proceeds, Vermont bears watching. If this small, healthy state can’t make Obamacare work to a high degree of satisfaction, it doesn’t bode well for more difficult challenges.