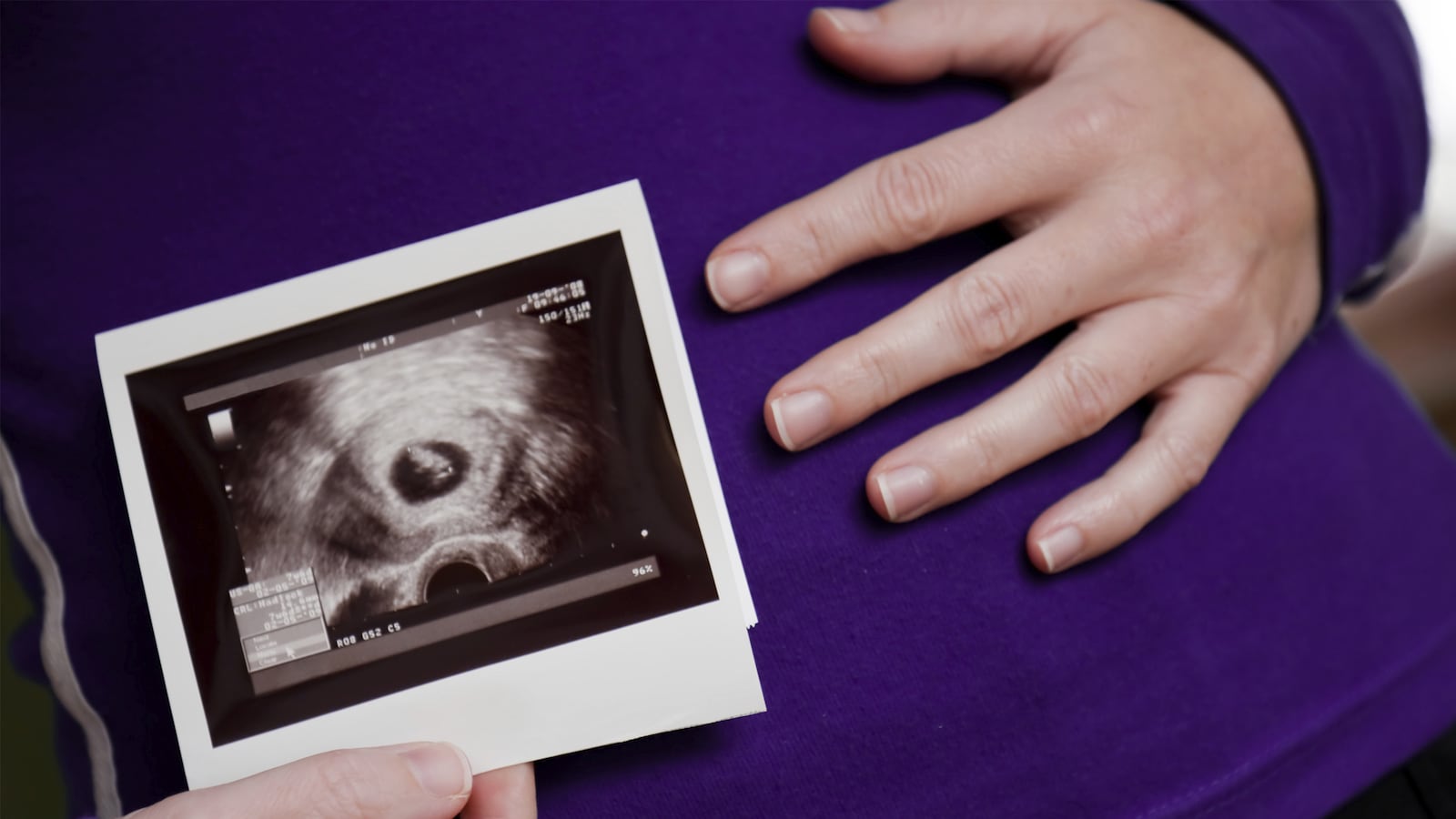
After three miscarriages, Colleen Abbott*, a 37-year-old New Englander, finally had what doctors told her was a viable pregnancy. Parents to a son already, Colleen and her husband, John*, hoped for a girl. When two sonograms confirmed the baby’s gender, they went out and bought pink dresses and looked forward to each new doctor’s visit.
Because of her age, and what appeared in a sonogram to be larger than normal ventricles in the baby’s brain, Colleen was scheduled to undergo a number of tests to screen her fetus for disorders and abnormalities. Doctors performed an amniocentesis, collecting a bit of amniotic fluid via a needle through her uterus. Full results take about two weeks, but Colleen got quick answers from what is known as a FISH test, which analyzes the fluid for only the most common abnormalities and for gender.
The news was good. The baby was fine in terms of chromosomal defects, but the test showed that the baby was a boy, not a girl as Colleen had been told. A follow-up ultrasound brought more upsetting information: The baby, while genetically male, had genitals that were “ambiguous.” He might have a deformed scrotum, or fused labia. He either had a small penis, or an enlarged clitoris.
It wasn’t just abnormal genitalia that Colleen had to worry about—there were a number of disorders associated with such a diagnosis, which could cause hormonal abnormalities and organ dysfunction. They scheduled an immediate meeting with the genetic counselor.
What happened at that visit depends on whom you ask. According to Colleen, the counselor told them their baby—not really a girl or a boy as they understood it—would have a tough road ahead. Along with social trauma, the child could suffer from liver and kidney failure, or even an early death. Colleen says the counselor told her that they were lucky to have caught the defects in time to abort.
“They gave her a choice: Abort the baby or take the chance of having a monster,” David Johns, the family’s lawyer, told me. The Abbotts did not return calls and emails for comment.
In the genetic counselor’s version, which is more in line with medical ethics and which was later considered by a jury to be a more probable scenario, Colleen had already decided to terminate the pregnancy by her visit. Far from suggesting an abortion, the genetic counselor says, she advised Colleen that she still had two weeks before the state’s 24-week abortion deadline, and asked the couple whether they might want to wait until the final, complete chromosomal analysis was in before they made a decision.
The two versions notwithstanding, what is clear is that after the genetic counseling, on Nov. 16, 2009, Colleen was admitted to the hospital, where doctors stopped the baby’s heart. Two days later, Colleen gave birth to a dead child.
In what can only be described as tragic timing, a day after the procedure to stop the baby’s heart and a day before Colleen would go into labor, the lab where Colleen’s amniocentesis had been analyzed called to report there had been a mistake. A secretary had mistakenly typed “XY” instead of “XX” in the gender field, an error that Colleen’s lawyer contends “was the first step in the long slide downward.”
An autopsy of the fetus showed none of the defects mentioned during the ultrasound.
The Abbotts sued the lab, the hospital, her doctors, and the genetic counselor, alleging the decision to terminate her pregnancy had been caused by the negligence of each, and was set in motion by the improperly transcribed FISH results. The jury found the lab and its director had been negligent, but stopped short of attributing fault for the abortion itself, refusing to award damages for the Abbotts’ physical and emotional injuries. The verdict was upheld in an appeals court in February.
While no pregnancy comes with a guarantee, there are an increasing number of tests that promise to identify the kind of abnormalities that keep expecting parents up at night. What happens when those tests turn out to be wrong, from a legal standpoint at least, all depends on the outcome.
The Abbotts are the most recent in what legal scholars call “wrongful abortion” cases, in which a woman, guided by inaccurate information about the health of her fetus, decides to abort an otherwise healthy and wanted baby. There is no real way to gauge just how often women terminate healthy pregnancies based on inaccurate medical diagnoses, but anecdotal evidence suggests it’s more common than we hear about.
Most parents who abort healthy children will likely never know that they’ve done so. As Dr. Ronen Perry and Dr. Yehuda Adar explain in a 2005 paper in the Yale Journal of Health Policy, Law, and Ethics, “Something exceptional must occur before they infer that anything went wrong.” To detect a wrongful abortion, a mother would have to suspect that the initial diagnosis was incorrect—which is not likely to be the case if a woman decides on an abortion precisely because of a genetic test or a doctor’s advice—and to have access to some proof, also problematic considering the fetus is usually disposed of after the procedure.
More than two-thirds of pregnant women in the U.S. go through prenatal genetic screening for abnormalities such as Down syndrome, or Trisomy 21. Studies estimate that between 80 and 90 percent of parents who receive a diagnosis of Trisomy 21 choose to terminate their pregnancies. A smaller share, but still a majority of women choose abortion when their fetuses are diagnosed with a sex chromosome abnormality, like the Abbotts. Depending on the study, somewhere between 68 and 81 percent of mothers terminate pregnancies with a SCA diagnosis. Since newer, non-invasive prenatal tests flooded the market in 2011, more women than ever are lining up to receive screenings. But some women are taking screening results—which can be wrong up to half of the time—as a confirmed diagnosis and, like Colleen Abbott, are terminating healthy pregnancies before further testing can be done.
According to an investigation by the New England Center for Investigative Reporting, possibly hundreds of women have aborted fetuses based on these initial screenings. One test maker reported that more than 6 percent of women who were told their pregnancies were high-risk for fetal abnormalities aborted without further testing. At Stanford University, there were three cases of women aborting healthy fetuses after receiving abnormal results.
Though the effects of terminating a wanted pregnancy can be shattering, the law hasn’t yet found a way to make these mothers whole. In fact, only a handful of cases have made it into the courts.
In 1990, a service member sued the U.S. government after doctors at Walter Reed Medical Center diagnosed her with AIDS. Her doctors told her the fetus she was carrying would almost certainly have AIDS, too, and not live past his fifth birthday. Only after terminating the pregnancy did she learn that there had been a paperwork error and she never had AIDS.
More recently, in 2002, the Georgia Court of Appeals overturned a lower court ruling that Linda Breyne’s decision to terminate her pregnancy was a direct result of her doctor’s misreading of lab results. He had incorrectly diagnosed her fetus with Down syndrome when the fetus in fact had Trisomy-X, manifestations of which vary from child to child, but which is generally milder and without the physical abnormalities associated with Down. Breyne won her appeal, but the court was clear that it found her case to be a medical malpractice claim, not a wrongful death—because no law exists in the state to recover damages for the life of a fetus.
The seminal wrongful abortion case is 1987’s Martinez v. Long Island Jewish Hillside Medical Center. A deeply religious woman, Carmen Martinez, agreed to an abortion after being told that a medication she had taken would cause major birth defects, which turned out to be untrue. The court ruled in her favor, not for the pain that came from losing a wanted child, but as a result of the anguish that came from violating her religious beliefs. The appeals court further explained the unnecessary role of the actual baby in the judgment: “The emotional distress for which she seeks recovery does not derive from what happened to the fetus; it derives from the psychological injury directly caused by her agreeing to an act which, as the jury found, was contrary to her firmly held beliefs.”
That’s about all there is when it comes to wrongful abortion cases.
In the 2005 paper in the Yale Journal of Health Policy, Law, and Ethics, the authors called the lack of legal recompense for the potential life lost as a result of medical errors “a significant and disturbing anomaly in American law” and declared that wrongful abortions are a unique problem to which the current law has not found a solution.
The law has managed to find a solution to wrongful abortion’s counterweight. In what are known as “wrongful birth” suits, doctors have been found liable for disabled babies born to parents who would have terminated their pregnancies had they been informed of their child’s condition. In 2013, a Washington jury awarded a couple $50 million for the “wrongful birth” of their 5-year-old child, whose rare genetic defect the doctors had failed to catch.
Though wrongful birth and abortion are variants on the idea of informed consent—“If I had known this about my fetus, then I would have made a different decision”—the law is heavily weighted in the direction of wrongful birth.
This may be a result of courts that are uncomfortable awarding damages purely for emotional distress, but accept problems with a measurable economic cost, said Sonia Suter, a former genetic counselor and current professor of law at George Washington University Law School.
“When parents give birth to a child who has severe birth defects, they really are going to be paying extraordinary damages in the medical costs and educational costs of that child,” Suter said. “You could argue that the courts aren’t being so unreasonable in the sense that they’re allowing for these really potentially devastating economic costs in having a child that these people wouldn’t have had, and that’s concrete and measurable and the court doesn’t have to worry about fraud or about the difficulty of proof.”
Still, Suter is worried about the implications of these court decisions, which she says just lead to the overincentivizing of genetic counseling.
“You don’t test for something that is diagnosable and leads to significant economic costs to the family? That’s a huge liability risk. But your chances of being found liable for wrongful abortion are pretty slim.”
“We are pushing people down a path of far too much information that leads to all sorts of dilemmas and confusion,” she said. “It will be interesting to see if in the next five years we don’t start seeing more of these cases.”
*Names have been changed out of respect for the family’s request for privacy.