Marc Koska had always wanted to dig up one great idea, one major strategy for helping people in a global way. He didn’t know what it would look like or where it would come from. Like any cloud-headed student or barstool idealist, he just wanted to change the world.
For the first 23 years of his life, Koska didn’t look around especially hard. The day after he graduated from the prestigious Stowe School in Buckingham, England, already set to forgo college, Koska became a garbage man. Just to pick up some money through the summer, not because of any calling in public sanitation. When he’d had enough of collecting trash, he looked at his options again and thought, “Well, I could go do something normal, which wasn’t really me. Or I could follow my nose and get on a train first.”
He chose the latter. For the next four years, aimless wandering carried him around the world, at times working on yachts and in ski resorts, until it landed him in front of a newspaper article one day in 1984. “It simply said, ‘One day syringes will be a major cause of the spread of HIV,’” he said in a telephone interview from England. “Sadly, that’s come horrifyingly true. Now we have a situation where, potentially, AIDS is spread as much by medical devices and poor practice as anything else.”
Indeed, unsafe injections are as serious as any epidemic in the developing world. According to a 2009 World Health Organization report, some 40 percent of injections worldwide are given with syringes and needles that are being reused without sterilization, causing an estimated 1.3 million deaths every year. HIV, Hepatitis B, and Hepatitis C are the main offenders. Educating patients to demand new needles is still a critical issue, as is the prevalence of dangerous medical practices—doctors who convince their patients they are breaking out fresh ones by rustling wrappers under their desks or nurses simply following orders.
“We’re told to,” one nurse in Faridabad, India, told the Times of London in 2009. “They tell us to use the syringes sometimes two times, three times, 10 times. I have seen them reused 30 or 40 times.”
“They are accustomed like this,” she added, referring to the doctors at her hospital. “They have practiced this way always, and they will continue. It may be they think if they reuse [syringes] they will save money.”
But the problem does not only stem from the economic interests of health-care providers.
"In developing countries, people go see the doctor and you can't get them out unless you give them an injection," said Dr. Ernest Drucker, an adjunct professor of epidemiology at Columbia University's School of Public Health. He cited a study dating as far back as the 1960s that showed that 80 percent of households in Uganda had a syringe, adding, "They feel like they haven't been treated if they don't get an injection. 'Magic shots,' they call them."
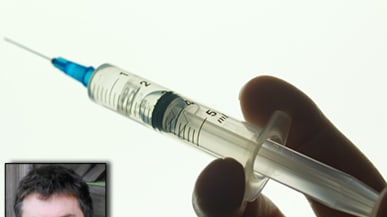
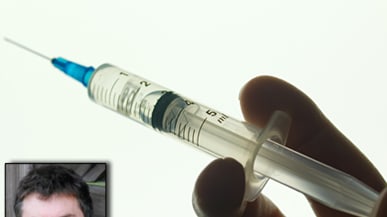
It is with these conditions unfolding throughout the developing world, that the idea Koska had been looking for began to crystallize 26 years ago. And by 1997, it turned into a patent for one of the first auto-disable syringes that also worked for curative injections. The name may sound complicated, but the idea is beautifully simple. How do you make sure people don’t use syringes twice? Make them impossible to refill. The K1, as Koska dubbed it, is equipped with a locking ring in the bottom of the barrel, so that when the plunger is fully depressed it stays there. Trying to pull the plunger back would snap the ring and effectively break the syringe.
The K1 model is not the only auto-disable syringe out there. When he first started working on it, there were more than 250 other patents around, and by the time he registered his, that number had grown to about 1,000. Of those, however, Koska says only about 20 had been made into prototypes and all of them were designed specifically for the small doses used in immunization. His design was also suitable for curative purposes, meaning the K1 could handle a whole range of doses.
Ultimately, it was a low-tech solution in a medical environment that is growing ever more expensive and sophisticated. Koska’s answer wasn’t a revolutionary apparatus, it was a small adjustment to existing technology with potentially massive impact. Not to mention a price tag for the developing world—K1 syringes sell for 5 cents, while many others go for as much as a $1 apiece.
“I always understood that what I was doing when I first came up with the design concept was going backward against the stream of thought,” says Koska. “The 270-odd patents, even 25 years ago, were all more complicated. I realized that none of them were going to get off the ground, because they were over-engineered. And over-engineering costs money to produce. I deliberately went to the simple end of the spectrum.”
Before he could even begin considering a design, Koska had to figure out exactly what he was dealing with. All he had in 1984 was a high-school science background and a newspaper clipping. So he spent over two years traveling, reading, and pestering anyone he could find who knew something about public health and had the technical know-how to help him. “I don’t think I even took any notes,” he says. “I just kept asking questions. I’d end up at the World Health Organization and ask them 20 questions about a trip I’d just taken to Kenya and watching immunization campaigns,” Koska says. “It was very random. But it built up a picture for me.”
Seventeen years after the idea first dawned on him, Koska sold his first syringe.
During that time, his efforts to popularize it did not make him any friends. Rival manufacturers, Koska suspects, were not especially pleased with his crashing the market. His first licensee in the developing world was suddenly and mysteriously bought out by an anonymous party and then bulldozed to the ground. Another factory in India simply failed to sell any. Finally, in late 2001, UNICEF placed an order. And soon after, he saw one of his syringes being used for the first time in Cambodia. (UNICEF has since made it a requirement of its campaigns to only use auto-disable syringes.)
Today, Koska runs Star Syringe, the company that owns his patents, alongside a nonprofit called Safe Point, which he started in 2006 for lobbying and education. His licensees are on the verge of selling their 2 billionth unit. Production is up to about 2 million a day, giving Star Syringe a 1 to 2 percent market share of all the syringes manufactured around the world, auto-disable and standard.
But beyond the worldwide numbers, Koska says that the real effect can be seen in places like the hospital in Tanzania, where the average stay has plummeted from seven days to three.
The only change it made was switching syringes.
Joshua Robinson is a freelance writer based in Manhattan. His work has appeared in The New York Times, The Wall Street Journal, The Washington Post, and Sports Illustrated.