
U.S. News
Real Heroes, True Crime, Sharp Opinion




Around 100 protesters were arrested on Saturday at a pro-Palestine encampment at Northeastern University, but not the one whose hate speech got everything shut down.
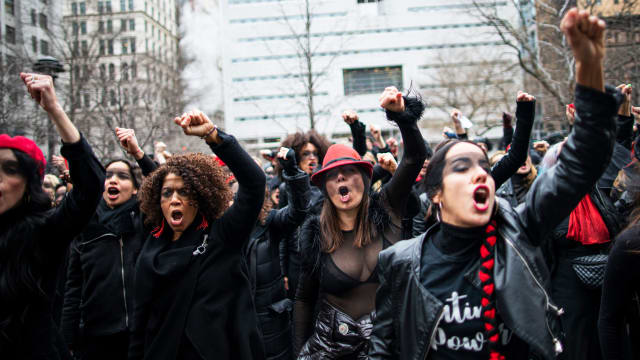
What #MeToo did—and what overturning convictions cannot take away—is reshape understanding of sexual assault and harassment as both pervasive and related more to power than sex.

A debate over how the university is handling the pro-Palestinian encampments is raging in Facebook groups.

The Trump Organization calls Trump Tower “one of the most iconic commercial properties anywhere in the world...” Have they visited the place lately?

The 48-year old woman threatened to call child protective services on a girl wearing a mini skirt.

The celebrity hotspot paid out millions of dollars based on false invoices, it claims.

Weinstein will be in Manhattan Supreme Court next Wednesday, less than a week after the state’s highest court overturned his 2020 rape conviction.