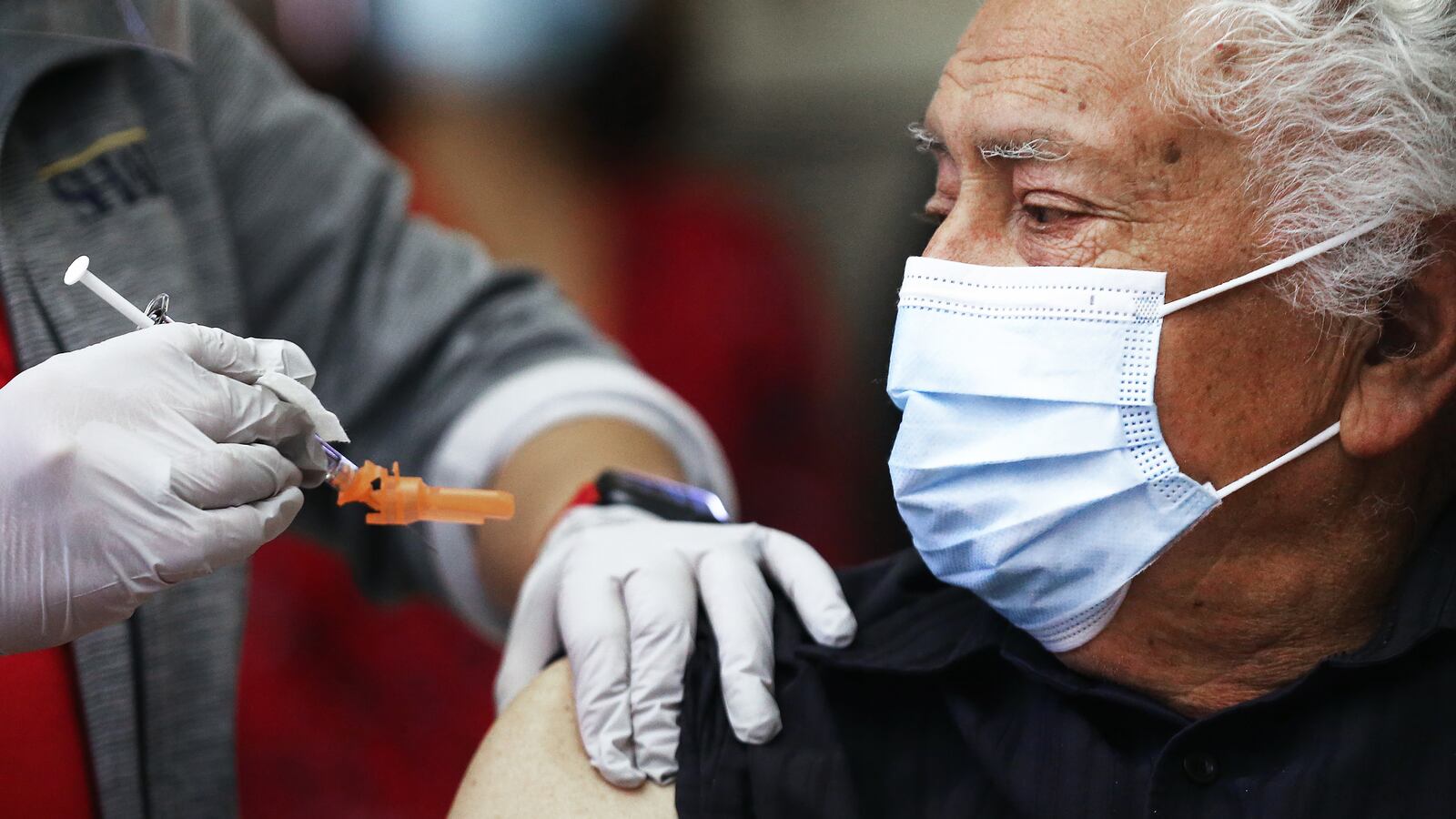
Now in one of the nation's worst coronavirus hotspots, California residents hoped for a speedy vaccine rollout. But less than a month in, hospitals have only administered 35 percent of the 1.3 million doses that have arrived in the state.
So far, only 454,306 doses of vaccine have been administered—just 1 percent of the state’s population—pushing California further behind its original goal to administer 2 million doses by the end of 2020.
“We’re going to start seeing more rapid distribution of vaccines, I can assure you of that,” California Gov. Gavin Newsom said during a Monday news briefing. “That said, it’s gone too slowly, I know, for many of us. All of us, I think, we want to see 100 percent of what’s received immediately administered in people’s arms. We are working aggressively to accelerate our pace.”
California has been plagued by logistical hiccups, including trouble finding enough health officials to administer vaccinations and enough federal funding to create infrastructure for safe and secure vaccine hubs. Local health officials have also blamed a pre-existing health-care delivery structure from the federal government that has never dealt with the strain on such a quickly built and volatile supply chain.
Newsom on Monday said the state would start using “flexible language” designating who is prioritized for vaccines in instances where the doses are set to expire. He also said the state is looking to enlist dentists, pharmacy technicians, and National Guard members to help speed up the process.
“We’re not going to enforce against people trying to do the right thing, and common sense,” he said, breaking from some of his elected colleagues.
California is not alone. Across the country, several states have reported shockingly small numbers of residents who have received their first vaccine despite receiving ample doses.
The worst output in the country, according to the CDC, is in the South. Georgia has only administered 708 doses per 100,000 residents, while Mississippi has given the shot to roughly 733 per every 100,000. In Alabama, only 807 residents have received their first shot out of 100,000 residents, even though almost 85,000 vaccines were distributed to the state.
Kansas is reporting the slowest COVID-19 vaccination rate in the country, having administered about 690 doses per 100,000 residents. State health officials, however, insist a local lag in reporting data to the state is to blame.
The frustration over the sluggish rollout is compounded as cases of the virus keep skyrocketing, prompting some state officials to even threaten hospitals to speed up their roll-out or face losing doses entirely, along with hefty fines.
“We are below where we want to be,” Anthony Fauci, director of the National Institute of Allergy and Infectious Diseases, admitted in an interview with CNN on Monday. “Not being responsible myself for the rollout, I can’t personally guarantee that we’re going to catch up. I hope we do.”
Since December, at least 15,418,500 doses of the Pfizer-BioNTech and Moderna vaccines have been distributed nationwide, the CDC reported. But only about 4.6 million people had received their first shots as of Tuesday morning.
One main factor slowing hospitals down is the strict adherence to CDC guidelines, which suggests prioritizing health-care workers and nursing home residents and staff before other essential workers and people over 75. But at the rate this is happening, the general population won't be vaccinated by spring as public health officials once predicted—a troubling reality given COVID-19 has already killed 350,000 Americans and infected about 20 million.
To make matters worse, while both vaccines can last up to six months frozen, the Pfizer doses are only viable for five days after being thawed. The Moderna vaccine can be kept refrigerated for up to 30 days. Both vaccines require two shots.
Edwin Michael, an epidemiologist at the Center for Global Health Infectious Disease Research at the University of South Florida, stressed to The Daily Beast that hospitals shouldn’t bear the brunt of the blame—because they’re only following state guidelines.
“I think the hospitals have planned for a phased rollout following CDC guidelines,” Michael told The Daily Beast.
“So, it is unfair to place blame on the delayed rollout just on hospitals given the sudden policy changes. The governors needed to have a coordinated plan and greater support in place well before the vaccinations began.”
On Monday, New York Gov. Andrew Cuomo revealed that 300,000 vaccine doses had been administered in three weeks, less than half what was allocated. He threatened fines or disqualification from future vaccine handouts for health-care systems that don’t use up supplies within one week of delivery.
Florida Gov. Ron DeSantis made a similar threat on Monday, saying that “hospitals that are not doing a good job of getting the vaccine out” will see supplies redistributed to providers who are.
“I do not want to see a vaccine sitting around not being used when you could be putting a shot in an arm,” DeSantis said.
According to the CDC, just 260,665 residents in Florida—or 0.8 percent of the state’s population—have been vaccinated, even though 1.1 million doses were distributed.
To speed up the process, some local health officials are even turning to online services, like Eventbrite, to schedule vaccine appointments. According to The Verge, health departments are using the platform, known for selling concert tickets, to easily set up appointments and ensure every dose is administered as quickly as possible.
This electronic assistance may prove helpful in Kansas, a state with the lowest COVID-19 vaccination output. According to the CDC, Kansas has vaccinated 20,100 residents, even though they received over 131,000 doses.
But the Kansas Department of Health and Environment insists the CDC database does not show the state’s full vaccination rollout and insists doses are not sitting on shelves. A health department spokesperson told The Daily Beast on Monday the vaccines were distributed to all 105 counties and there have been delays in reporting.
“What you’re seeing on the data side does not reflect what we’re hearing around the state,” Cindy Samuelson, vice president of member and public relations at the Kansas Hospital Association, told the Kansas City Star. “The experience we’re hearing is that we’re one of the few states that have been able to get vaccines into the hands of every county.”
Several experts told The Daily Beast that states have been left largely to navigate the logistics alone, compounding delays. For months before the two vaccines were authorized, states begged the federal government for additional funding to train health-care workers and create vaccine hub infrastructure. While the Trump administration did provide some funding, officials said it was too little, too late.
“There appears to be no investment or plan in the last mile,” Ashish Jha, dean of the Brown University School of Public Health, wrote on Twitter. “No effort from Feds to help states launch a real vaccination infrastructure. Did the Feds not know vaccines were coming? Shouldn’t planning around vaccination sites, etc not have happened in October or November?”
President Donald Trump, however, has blamed the slow rollout on states after what he called a “successful and very large scale distribution of vaccines” by his administration. Surgeon General Jerome Adams also insisted “this was always going to be the most difficult vaccine rollout in history.”
But Michael insists that the blame game by politicians will not hurry the rollout—and only shows the divide between the government and the public health system.
“Hospitals are under strain and it is essential that the governors also support them with extra resources given that hospitals also have to deal with increasing COVID cases in parallel,” he added.