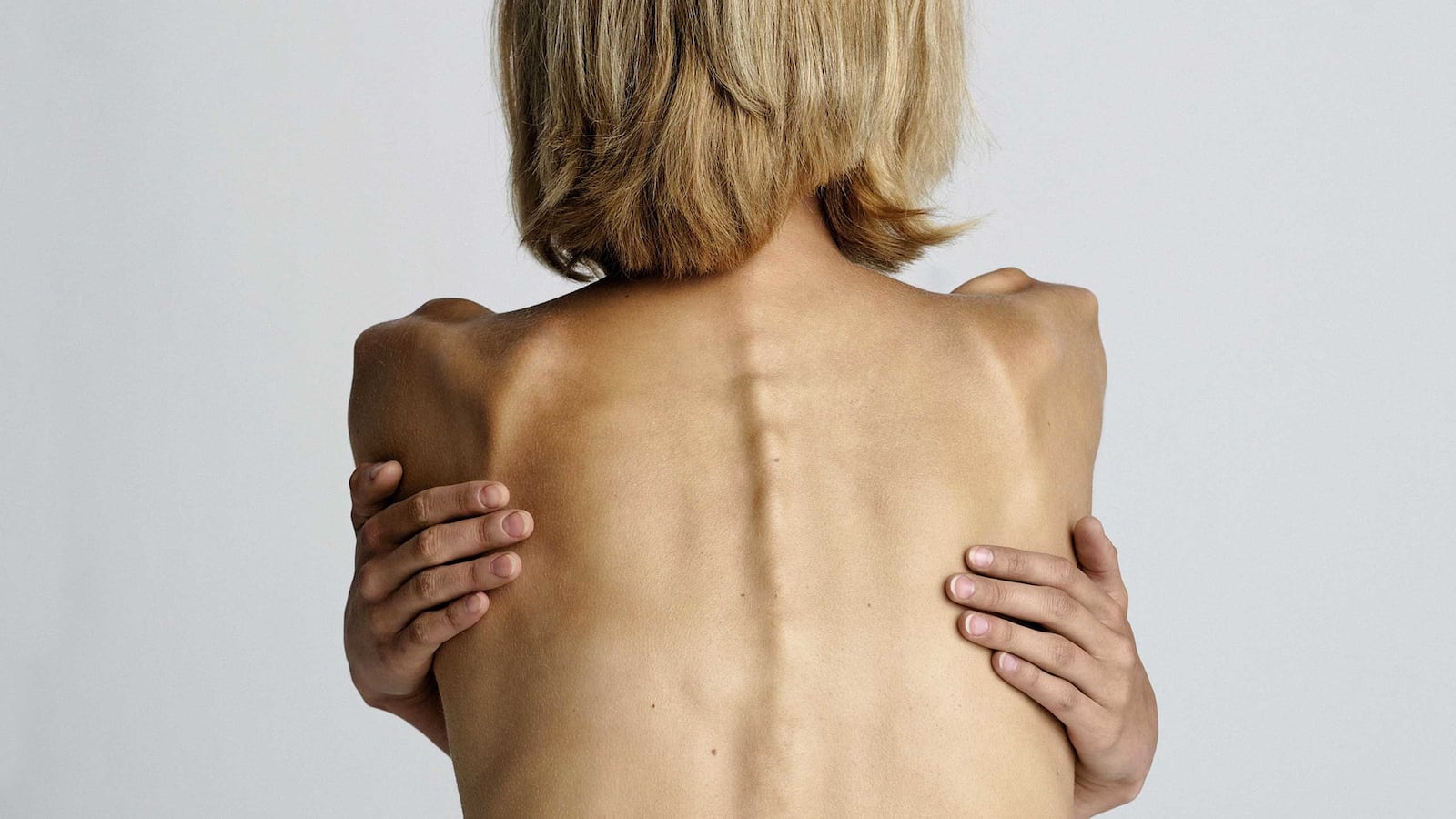
Researchers and doctors have begun using deep brain stimulation (DBS) to treat anorexia nervosa. In just a tiny handful of cases so far, neurosurgeons have implanted electrodes into the nucleus accumbens in the brains of patients. The nucleus accumbens plays a significant role in producing pleasure and motivation.
“For those with severe enduring anorexia nervosa—by which I mean at least seven years of illness—there is a terrible lack of effective or evidence-based treatments, and a lack of hope for full recovery,” said Rebecca Park, associate professor and consultant psychiatrist at Oxford University who specializes in eating disorders and has helped lead research on DBS. “Our research and that of others suggests that DBS might be developed as a novel means of helping the most severely affected. At present it is an experimental treatment, with no guarantee of benefit.”
DBS has been used to treat Parkinson’s and other movement disorders. In the past 15 years, it has also been studied in mental disorders, particularly obsessive-compulsive disorder and depression. It’s considered a last-resort treatment. The risks can include bleeding from surgery, seizures, as well as speech and motor issues. Its benefits, however (depending on the disorder) can be substantial as well.
Dr. Finza Latif is a child and adolescent psychiatrist at Children’s National Health System. She also leads an outpatient eating disorders clinic. “We know risks but we don’t know benefits for anorexia at this point. We don’t have good data,” said Latif. “DBS targets certain area of the brains, but we don’t have a good brain mapping of anorexia. A DBS treatment might affect other brain functions.”
Last Thursday, Julian Savulescu and Hannah Maslen, a professor of philosophy and a post-doctoral fellow at Oxford, respectively, wrote a blog post raising ethical issues with the use of DBS as a treatment for anorexia.
While they have cautious optimism about the procedure, they are particularly concerned about whether patients can truly consent to the procedure. DBS is only being researched right now; it is not used clinically. But Maslen and Savulescu worry that because it is likely to be used as a treatment of last resort, people with anorexia may only be agreeing to DBS in order to avoid being force-fed. In that case, they argue, their consent for DBS is not freely given.
I interviewed Maslen and Savulescu by email, and they co-wrote their responses. “In terms of the way the patient perceives the choices, they might therefore think that they are being forced to choose between DBS or the possibility that they will be fed against their will,” they commented. “Since the option of maintaining their status quo situation (i.e. neither undergoing surgery nor being fed) is made unavailable to them (or so they believe), there is a sense in which they are being coerced.”
“All our studies are accompanied by a thorough and rigorous ethical assessment,” specified Park. “We would not accept onto our trial anyone who is not assessed as fully consenting, capacitous, and voluntary.”
The question of consent and anorexia quickly becomes complicated. Unlike other mental disorders, such as depression, people with anorexia often don’t want to be treated. They enjoy their high degree of self-control. Should we treat people with anorexia who don’t wish to be treated—even if being untreated means they might die?
Latif stressed that anorexia is much more treatable earlier, partly because the patient is still living with parents or guardians and thus is more compelled to follow a treatment he or she might not choose.
“Is anorexia more like a major depressive disorder with suicidal thoughts, when we’d intervene against someone’s consent? Or is it more a behavioral disorder?” she reflected. “Getting informed consent can be additionally difficult because privation affects thought processes. It affects the ability to fully understand risks and benefits.”
Maslen and Savulescu are particularly interested in protecting the medical autonomy of people with anorexia as much as possible. “Whether anorexic patients should ever be treated against or in the absence of their will is a deeply challenging ethical problem that requires more attention. In England and Wales and some other jurisdictions the decision is sometimes made by a judge,” they wrote.
They consider the effects of privation on cognition as important, but still emphasize the need to respect autonomy. “Even if competence is lost in the end stages of anorexia, when cognitive function is severely impaired, it is retained early in the illness. Many anorexics are as competent as the rest of us, in all domains except eating, at least early in the illness,” they point out.
“One idea is to have anorexics complete living wills or advance directives about things like force feeding, or DBS, if their condition deteriorates, before they become ‘end stage’. People ought to be able to make decisions about force feeding and DBS, and we ought to try to find windows when they are competent to make such decisions.”
Another concern Maslen and Savulescu raised in the blog post was that DBS treats only the brain, while anorexia itself is a complex psychosocial disorder. While DBS targets the nucleus accumbens, it increases the rewards of eating. But the problem is not usually that people with anorexia don’t enjoy eating, it’s that they practice excessive self-control over eating. Thus, DBS treatments may miss part of the problem with anorexia.
Park and others do plan to target other areas of the brain, and she does not see DBS as a cure-all. “All interventions such as DBS on neural circuits should be accompanied by psychosocial interventions,” said Park. “They should not be seen in isolation as a magic bullet. Rather, it is hoped that they will facilitate change and gradual recovery in those who have become rigidly stuck in a trap of compulsive eating disorder behaviors, and have tried all other recommended forms of treatment to no avail.”
Maslen and Savulescu emphasize the importance of respecting how much of our identities can be bound up with food and what we eat. “Our concern was that anorexia is likely to be more complicated than a simple lack of desire for food. To the extent that there are other underlying psychological or social factors implicated in the illness, great care must be taken to assess how these interact with and are affected by any changes in basic appetite,” they wrote. “If the anorexic patient has a deeply held desire to manage what they eat, the desirability of food could come into conflict with this.”
Park’s and others’ research has suggested there may be connections between our experience of reward and excessive self-control. A therapy that helps regulate the processing of reward, then, might also mitigate the compulsive control seen in patients with anorexia nervosa.
“We are currently focusing on a neural target which has been found of benefit in other compulsive disorders, such as severe intractable OCD and addictions. There is good evidence that anorexia nervosa has some aspects in common with these disorders,” Park pointed out.
“If we had as good an understanding of the brain as we do the heart, we might predict the effect of a treatment,” said Latif. “However, with brain treatments, for now we just don’t know what the overall effects might be.”
Maslen and Savulescu said, “This is a paradigm case of thinking holistically both about causation and treatment: we ought to embrace all of the biological, psychological and social factors in causation and treatment. What matters, we think, is whether an intervention works.”