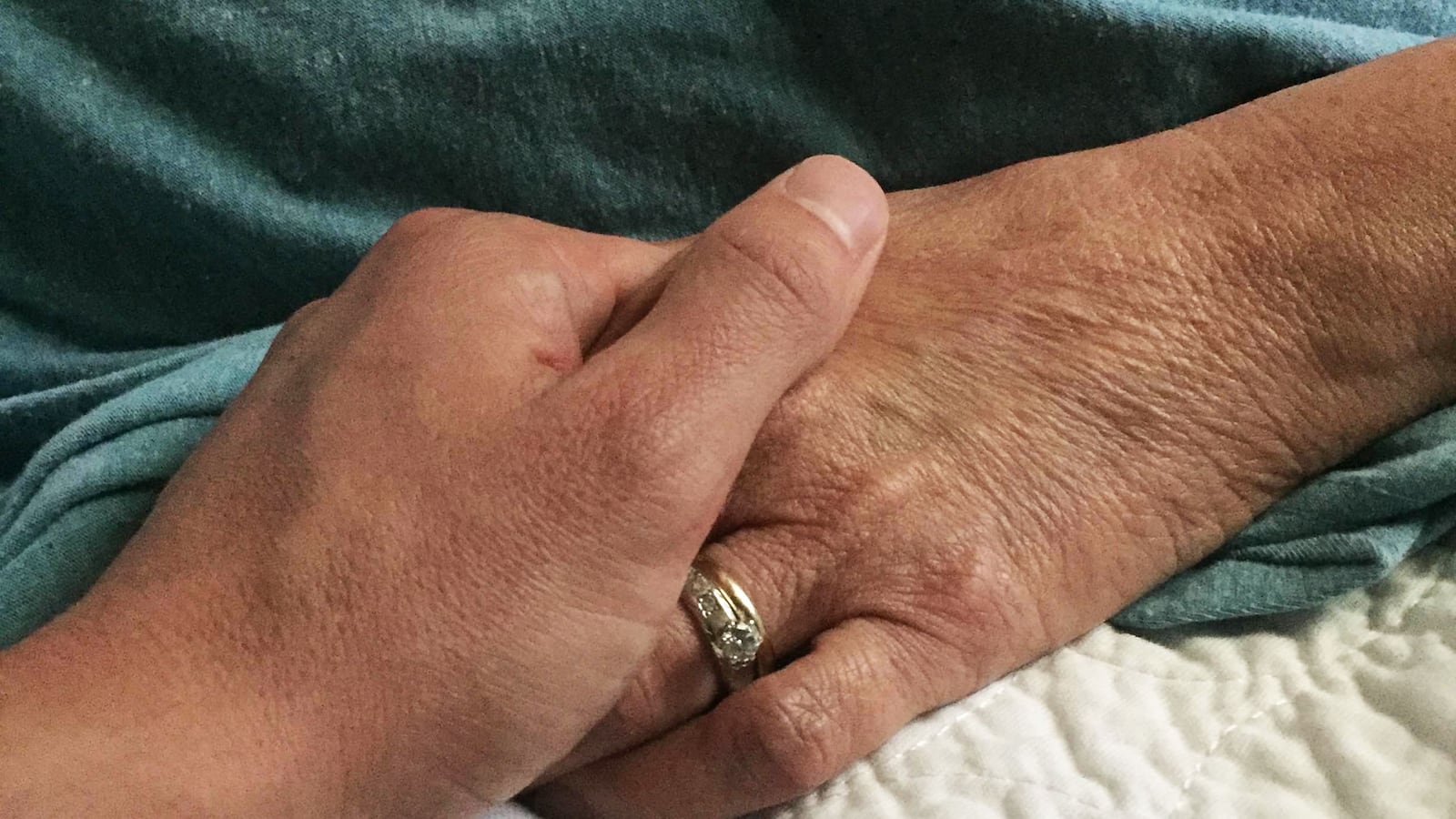
At the end of my mother’s life, when her breathing slowed to stillness, the fingers at her wrist to feel her pulse for the last time were mine.
For the past several years, my mother had been receiving treatment for ovarian cancer. Thanks to catching it early and enrollment in a series of clinical trials, her quality of life and overall health were pretty good. We maintained hope that hers would be more of a manageable chronic illness than one that would ultimately become terminal.
And then a couple of months ago she began to feel dizzy. Her doctors back home thought it may have been related to some kind of infection, but her symptoms didn’t improve with treatment. Instead, she began to have headaches, and then nausea.
A short time later, an MRI and a lumbar puncture confirmed the news we had hoped never to hear—Mom’s cancer had spread to the lining around her brain. It was estimated that she had only a few weeks ahead of her. A couple of treatment options were held out for her to consider, but none offered more than a short extension of her life, if any, and all carried side effects she wanted to avoid.
In the end, she opted to receive palliative care—medical practice that focuses on relief and quality of life for the seriously, and often terminally, ill—at home.
I was scheduled to go on vacation with my husband and kids at the same time this change in Mom’s health was discovered. We pulled out the virtual GPS pin from Cape Cod and planted it in my Missouri hometown to join my parents, along with my brother who had already flown to be with them.
Mom’s symptoms progressed far more rapidly than even the poor prognosis she’d been given had predicted. Midway through our second day of driving, Dad contacted me to say Mom could no longer really have a conversation. We drove straight past our planned stop in Ohio, my husband and kids got a hotel room after 15 hours in the car, and I arrived back at my childhood home a little past midnight.
Though my work as a physician has never been directly with hospice patients, I knew enough about pain management to feel comfortable erring on the side of Mom’s comfort. Of my few complaints with my family’s experience with palliative care, one is that there weren’t clearer parameters for how proactive to be about managing her symptoms. She had already started spitting out pills by the time I got there, and Dad didn’t know at what point to start the liquid morphine.
Once I arrived, we had her on a schedule of medication for pain and anxiety. Knowing we were able to keep her comfortable in the last days is one of the things that meant most to us.
When I first arrived, Mom could acknowledge I was there by kissing my hand when I rested it on her cheek, but otherwise didn’t have much ability to interact meaningfully. The second day I was there, however, she seemed to emerge from the enveloping confusion and was able to see the people who had gathered to be with her.
The obvious joy she took at seeing her grandchildren at her bedside comprises my last happy memories of her, along with hearing her murmur about how much she loved my brother and me. I am incredibly grateful that my children could play in the summer sun jumping through the sprinkler in the same backyard I did growing up, but spend time with Grandma inside, too.
The next day she roused a bit to identify a song she liked from the music we kept playing, and to speak about some memory of watching the Cardinals play back in the 1960s. After that, she simply slept. She stopped eating the small chunks of watermelon my Dad cut up for her, and wouldn’t swallow ice chips.
Gradually her breathing slowed and became more irregular. Gradually I heard fluid accumulate in her lungs.
There were moments that felt foreign and unsettling to me, both as a son and a doctor, to sit and watch her condition deteriorate, and know there were interventions that could have taken over the functions of her failing body. A ventilator could have pushed breath into her, and a bedside nurse could have suctioned those secretions from her airways. An IV could have delivered the fluids she could no longer take by mouth.
But those interventions would not have prolonged her life, merely her physiology. The vibrant, eccentric women who had raised me, often driven me nuts, and recapped old Leave It to Beaver episodes for my oldest son when he asked for stories had already gone.
Caring for Mom at home also meant abandoning any squeamishness about all that would be required to look after her. Whatever impulse I possessed to glance away when hygienic needs had to be met had to be abandoned. Yet once that counterproductive gesture toward modesty had been discarded, it felt right to share with my father and brother all of these final responsibilities. It was one last way to show her we loved her, even if she could no longer perceive it.
In those final days, the hospice nurse who came to our home was wonderful. In Larissa MacFarquhar’s moving profile for The New Yorker of a woman who does the same kind of work, she writes “Some hospice workers believe that working with the dying is the closest you can get on earth to the presence of God.” While I would not presume to speak for the nurse who helped us care for Mom, it was undeniable that she did so with compassion and dedication. Even when there was little more to do, her visits were a comfort. It helped to have someone reassure us we were doing all we could to ease this final task of life.
As the pauses in Mom’s breathing drew longer, we lit candles rather than keeping the lights turned low overnight. We no longer left any gaps, even for a few minutes, in our shifts at her bedside.
Early one morning, after catching a few hours of sleep after staying up all night talking with my brother as we sat with Mom, Dad came into my old bedroom to wake me. It was time.
I walked back to her bedside, along with my uncle, my dad, and my brother. I watched her chest rise very slightly one last time. I felt her cool hands, and put my fingers over her radial artery. I felt one final beat, and then nothing more.
I cried. I called my husband. Someone called the hospice nurse, who showed up a short time later with two colleagues to prepare Mom’s body for its last departure from our home. I hugged her, and thanked her for all she had done for our family.
By happenstance, in the hours afterward I came across a review out of the UK about home palliative care, and about how it doubles the chances that patients will be able to die at home, which is what about 50 percent say they would want. It also found that home palliative care had no effect on the grief suffered by caregivers.
I cannot speak for the grieving process for any other person. The sorrow I feel at my mother’s death is doubtless different from my father’s, my uncle’s, my brother’s, or her friends’, despite it being the same person we all mourn. Every person, every patient, and every family is different.
But for my part, I am comforted to know Mom had the death she did, even though it was years and years and years too soon. She was surrounded by people who loved her, and who got to tell her so as often as they wanted. She was attended to by those who cared about her the most, and in the place she knew best. She went peacefully, and without pain.
It is the end she chose for herself. It’s what I would choose, too.