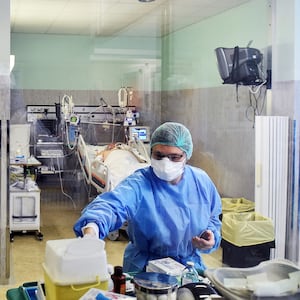
At one Queens hospital, 13 patients being treated for the novel coronavirus died in a mere 24 hours, as dozens more sick New Yorkers lined up outside in the cold waiting to get tested. Across town, construction workers in Manhattan have been working around the clock to build a makeshift morgue outside Bellevue Hospital, anticipating a surge of virus victims, while doctors inside are scrambling to secure more medical supplies.
The Federal Emergency Management Agency estimated that all of the intensive care beds in the city will be filled by Friday.
“Hospitals in New York are under siege—that’s probably the simplest way I can describe it,” an NYU Langone doctor told The Daily Beast. “We have never seen anything like this, and we are so unprepared for the need that seems to grow daily. Honestly, I’m terrified.”
As the epicenter of the coronavirus outbreak in the United States, New York City’s hospital system has been overwhelmed by patients, with physicians seemingly unable to keep up with the tidal wave of new cases that continue to surge daily as government officials rush to put a band-aid on the problem.
To date, over 385 people have died and 37,258 individuals have been infected with the virus across the city of 8.6 million, accounting for a quarter of all cases nationwide, New York Gov. Andrew Cuomo said Thursday. Within the last 24 hours, the number of people hospitalized has jumped 40 percent and over 100 have people died.
“New York City hospitals right now are on the brink of what I would call being maxed out in terms of their available capacity,” former Food and Drug Administration Commissioner Scott Gottlieb told CNBC on Wednesday. “New York has another about five weeks to go for this between now and when they’re going to hit peak hospitalizations, so the fact that they’re stretched right now is worrisome.”
While the cases account for fewer than 1 percent of the Empire State’s population, hospitals are overwhelmed, understaffed, and short on supplies—unable to keep up with a hospitalization rate that Cuomo said is “moving faster than initial estimates.” Health officials project that 140,000 New Yorkers will need to be hospitalized on account of the coronavirus over the next two weeks, which exceeds the state’s supply of hospital beds by 35 percent.
Cuomo confirmed fears of city hospitals overrun with coronavirus cases on Thursday, stating that under almost any realistic scenario of this pandemic, New York State would be overwhelmed by the number of patients.
“We’re adding to the hospital capacity every way we can,” Cuomo said. “Almost any scenario that is realistic will overwhelm the capacity of the current healthcare system. We cannot get the curve down low enough so that we don’t overwhelm the hospital’s capacity. We have to increase hospital capacity.”
To combat the lack of space, the Jacob K. Javits Convention Center has been repurposed as a makeshift overflow hospital facility, and Cuomo said officials are considering transforming dorms and hotels into emergency medical wards.
City universities are also taking extraordinary measures to fight the outbreak, as Columbia University and New York University announced Thursday that they will allow medical students to graduate early so they can pitch in with the response effort.
Cuomo added that urgently needed medical supplies have been distributed across the state for immediate needs—including one million surgical masks to New York City. Mayor Bill de Blasio previously said the federal government was sending 2,000 ventilators to the city—but that’s hardly enough to cover the 15,000 needed to continue helping residents.
“People forget, we are just at the beginning of the bell curve of what is to come here,” one Manhattan medical social worker told The Daily Beast. “The overwhelming idea at our hospital is that this is a bit of a war, and we need to pace ourselves.”
This “war” is most evident at Elmhurst Hospital Center: a 545-bed public facility in Queens that lost 13 patients within 24 hours this week. The hospital, which de Blasio said has seen a “disproportionately high number of cases,” has since begun transferring parents to other hospitals. New Yorkers waiting for treatment on Thursday morning were forced to stand outside the facility in a line organized by metal barricades that stretched around the block.
“Elmhurst is at the center of this crisis, and it’s the number one priority of our public hospital system right now,” a spokesperson for the New York City Health Department told The Daily Beast. “The frontline staff is going above and beyond in this crisis, and we continue surging supplies and personnel to this critical facility to keep pace with the crisis.”
The spokesperson added that while the deaths are “consistent with the number of ICU patients being treated there,” city officials are “increasing the effective capacity of the hospital on a daily basis by sending more doctors, nurses, ventilators, and PPE to meet demand.”
Outside Bellevue Hospital in Midtown Manhattan, construction and city medical examiner workers have been scrambling to fulfill another contingency plan in anticipation of the surge of coronavirus victims: a temporary morgue.
The building of the makeshift morgue—a grim reality of mass casualty events—was part of the city’s emergency declaration that de Blasio signed on March 13.
“I know the morgues push a really strong emotional button, obviously. We’re all humans,” de Blasio said in a Wednesday statement. “It’s a very troubling thing to see, and it makes it very immediate, very visceral. It’s going to be very, very painful.”
In addition to the makeshift morgue, Bellevue has a refrigerator truck that has yet to be activated in case of “any overflow,” a spokesperson told The Daily Beast. An identical truck at the Elmhurst Hospital Center is already active.
On the frontlines of this highly infectious virus are health care professionals who are facing a shortage of necessary supplies—forcing many doctors and nurses to treat patients without adequate protective equipment.
At Mount Sinai West in Manhattan, a nurse who had been treating infected patients died from the virus just one week after he tested positive, the hospital said in a statement to The Daily Beast. Kious Jordan Kelly, a nursing manager at the hospital in his 40s, was hospitalized on March 17 and died Tuesday.
“We are deeply saddened by the passing of a beloved member of our nursing staff. The safety of our staff and patients has never been of greater importance and we are taking every precaution possible to protect everyone,” the hospital said in a statement. “But this growing crisis is not abating and has already devastated hundreds of families in New York and turned our frontline professionals into true American heroes. Today, we lost another hero—a compassionate colleague, friend, and selfless caregiver.”
Muni Tahzib, a nurse at a CityMD walk-in clinic in Chelsea, contracted the virus after treating patients. After testing positive on Monday, Tahzib told The Daily Beast that while she is suffering a high fever and can barely breathe, she’s “mostly bummed for not being able to help my colleagues on the frontlines.”
“It’s vicious here in New York,” Tahzib said. “A number of my colleagues are going down.”
While she said she is not worried about recovering from the coronavirus—after working during many “humanitarian disasters” over the last decade—she worries for health-care professionals who are supposed to continue to treat infected New Yorkers with limited medical supplies.
“How is this going to happen? You can bring 15,000 ventilators, but the reality is we don’t have 15,000 intensive care doctors and nurses who can do this work,” she said, noting that before she fell sick, she and her colleagues were working up to seven 12-hour shifts a week.
Another Mount Sinai nurse told The Daily Beast that hospital doctors and nurses have been forced to use trash bags as productive gear—prompting daily arguments with infectious disease nurses and supply room supervisors over the distribution of limited resources to patients and staff.
“My chest hurts from arguing and crying,” she said. “The people at the top... have no idea what it is like. They wear nice suits and sit in their offices making phone calls and in conference rooms in meetings all day.”
“Put scrubs on and come and join us in our fight and then we can... come up with a better plan as to how together we will win this fight,” she added.
An ER doctor from the same hospital system reiterated those concerns, stating that within the last week, Mount Sinai has seen a “dramatic increase” in cases that has forced staff to learn as they go.
“We’re building space where we never knew we had space, repurposing formerly closed wards,” the doctor said. “We’re opening up spaces we have not used in years to care for patients.”
She added, “Unfortunately right now people who are in our waiting room have a very hard time staying six feet away, so that’s a dangerous place to be.”
Three Manhattan medical social workers told The Daily Beast that fear and anxiety among hospital staff and patients has reached an all-time high.
Patients are nervous to go into hospitals for fear of contracting the virus inside—or that their diagnosis will mean life-long financial ruin. Doctors, on the other hand, are nervous about potentially bringing the virus back home to their families and neighbors.
“As social workers, we are definitely the resident therapists for every single provider and patient here,” one social worker said with a laugh. “Medical social work is the link between a person’s medical world and the rest of their world. From what we’ve seen the last couple of weeks, everyone’s world is filled with anxiety of what is to come.”
One gynecologist at a New York City hospital added that while she has seen a shift at her public hospital over the last couple of weeks—especially as supplies began to dwindle and her pregnant patients grew fearful of giving birth amid a pandemic—she is proud of her colleagues for remaining focused and continuing to serve the community.
The doctor, who currently is not treating patients who are diagnosed with COVID-19, said she heard a rumor on Thursday that she may be deployed to a neighboring hospital to work on the frontlines, as many other physicians have been asked to do.
“Everyone’s a little anxious, but this is what you take an oath to do, so you just have to do it,” she said. “We just have to be supportive with each other, and that’s really it. Everyone just has a sense of duty.”
One medical social worker, however, was not so optimistic.
“We have a lot of frustrated doctors right now,” one said. “Honestly, leadership in this city had lots of clear information about how to get ahead of this pandemic, or at least handle it in a safe, effective way. They failed and the New York City health care system is going to suffer.”
—With reporting by Rachel Olding