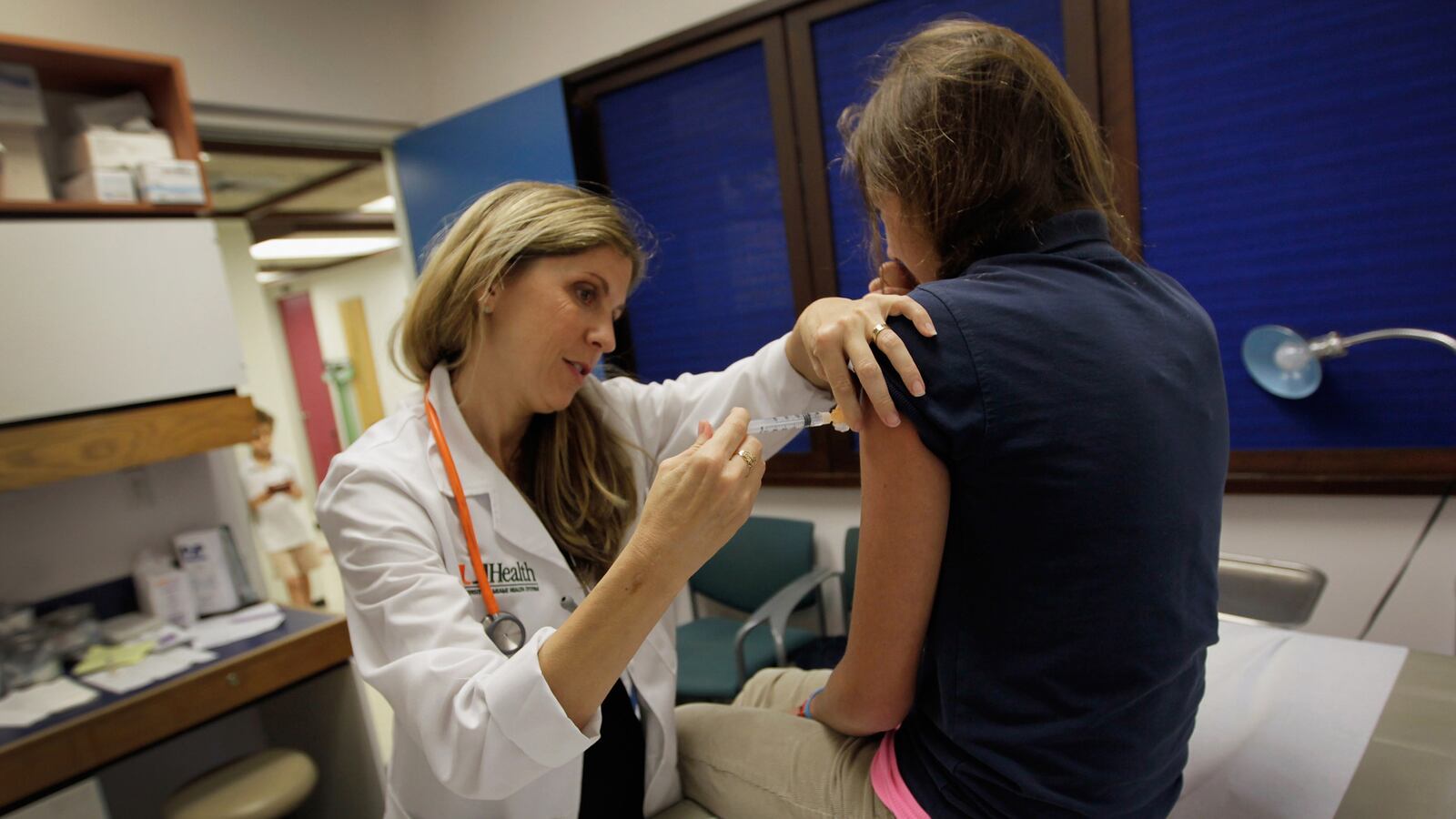
As a doctor, knowing you’re doing your part to make people just a little bit healthier is one of the best things about providing patient care. And seeing a new public health intervention taking effect in real time can be very exciting.
Take the vaccine to prevent human papillomavirus (HPV).
HPV is the virus that causes all warts in humans, including genital warts—the most common sexually-transmitted infection (STI). If you’re a sexually active adult, chances are you will be exposed to one strain or another at some point in your life, though most people never develop noticeable symptoms.
Infection with certain strains of the virus is a major risk factor for women to develop cervical cancer, which was diagnosed in almost 12,000 patients in 2010 and which killed nearly 4,000.
Thankfully, in 2006 two vaccines against HPV were introduced. One protects against the two strains that cause most cases of cervical cancer, while the other confers protection against those strains and two others that are responsible for most cases of genital warts.
I recommend the vaccine to all my patients who are old enough to receive it—both boys and girls. Girls get it to prevent cervical cancer and genital warts. I recommend it for boys for prevention of warts as well, but also to lower their risk of spreading the infection to partners later in life.
Further, there is evidence that HPV can also cause cancer in other locations, including the throat. The recommendation to immunize is an obvious one to me.
What’s been remarkable is how quickly the benefits have become apparent.
As reported in the New York Times, the prevalence of the cancer-causing strains of HPV has dropped in half since the introduction of the vaccine, and that’s with a mere 30% vaccination rate. To see such a drop already is very encouraging, and it makes me happy to be offering something to my patients that will help them avoid a now-preventable cancer.
Unfortunately, as is reported in the Times article, there is still a lot of mistrust about the vaccine in the general population. In a study in the journal Pediatrics from last March, over 40% of parents expressed resistance to vaccinating their children against HPV.
I’ve run into this resistance in my own practice. (Though my practice does not accept patients whose parents refuse to vaccinate them, we do not insist they agree to the HPV vaccine.)
Parents who otherwise have had their children fully immunized remain persistently opposed to the HPV vaccine.
Much of this resistance seems to stem from the vaccine’s novelty.
It hasn’t been on the market for all that long as compared to the others, and many parents tell me they just don’t think it’s been around for enough time to feel comfortable giving it.
Despite evidence that the vaccine is as safe as all the others (which is to say, very safe), there has been enough mistrust spread about the vaccine in the popular media over the past few years to call that conclusion into question.
Some parents also question the need to give the vaccine before their children are sexually active, given that it is meant to protect against an STI.
Once I explain that, like all preventive measures, the HPV vaccine will be most effective before actual exposure to the infection, many agree to let their children receive it.
One concern that has been raised about the vaccine is that it may reduce the perceived risk of sexual activity in teenagers, and thus encourage them to engage in behaviors that they might otherwise have avoided.
However, a new study has just been released that examined this possible effect, and found that patients who received the HPV vaccine did not engage in riskier behaviors as a result.
The study, published this month in Pediatrics, followed group of girls over a six-month period after first receiving the vaccine. At the end of the study period, no difference was found in the participants’ risk behaviors or perceptions about the importance of safer sex.
Receiving the HPV vaccine did not appear to make patients more likely to take risks with their health, despite fears to the contrary.
One surprising finding is that, in participants 16 to 21 years old, there was an erroneous belief that the vaccine protects against STIs other than HPV. Despite this incorrect perception, they indicated they were less likely to initiate sexual intercourse in the coming six months. This effect is difficult to explain, but does indicate that reduced concern about STI infection does not make patients think they have carte blanche to abandon safer sex practices.
As heartening as the reduction in HPV prevalence with the advent of the vaccine is, vaccination rates are still far below where they ought to be. Medical providers still have their work cut out them as they try to overcome the misperceptions about the vaccine’s safety, and its importance as a means of keeping patients healthy even before parents may presume.
The Pediatrics study is also a good reminder that we need to be clear with patients about the kinds of protection the vaccine provides, and the kinds it doesn’t.
It’s good to have one more piece of evidence that the HPV vaccine is a safe, effective and important measure in keeping people healthy. Any new data that help lower barriers to vaccination and that further the efforts to reduce rates of preventable cancers are welcome.