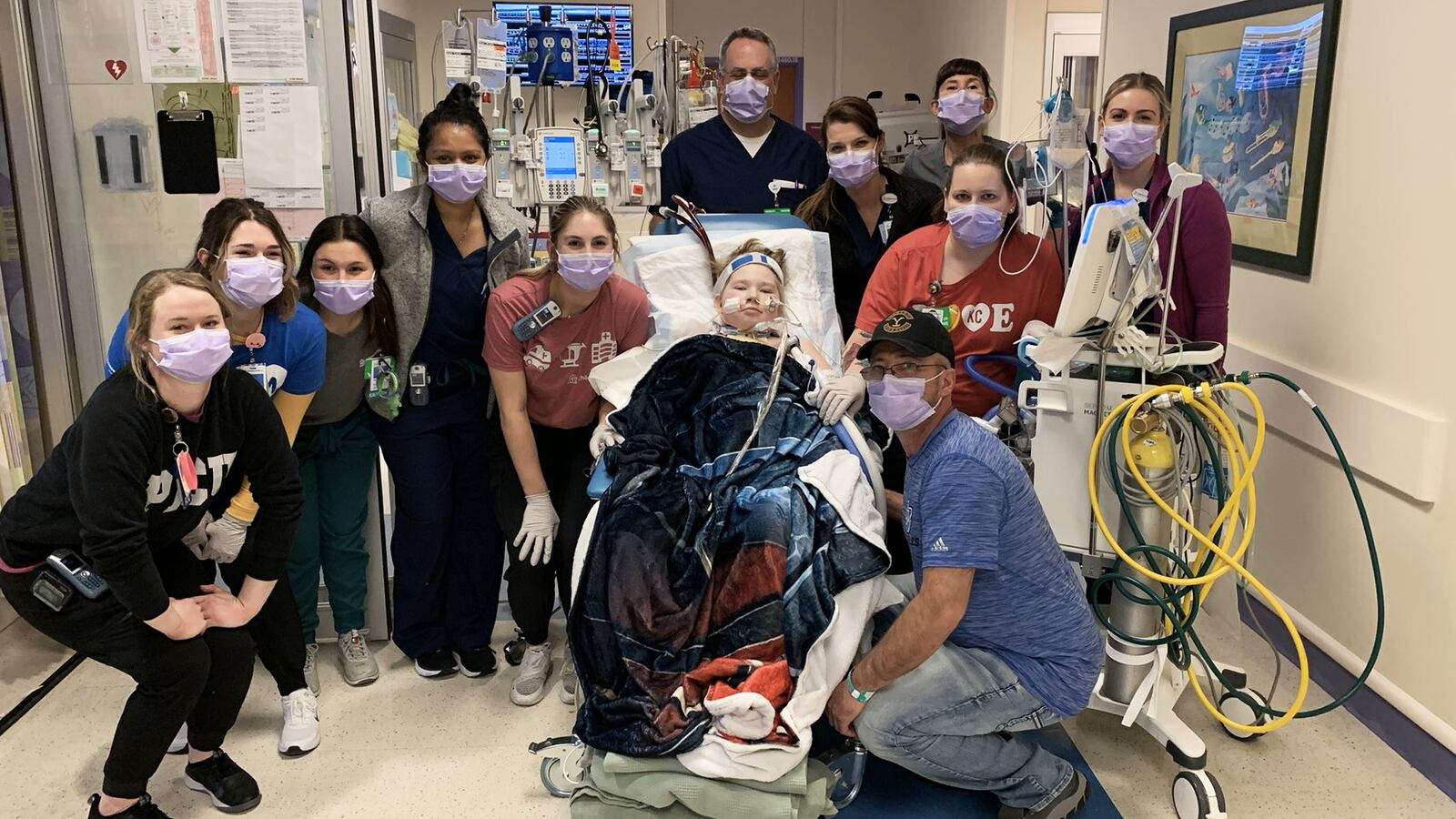
The X-rays showed that COVID-19 had trashed Trevor Hensley’s lungs, and the seventh grader was still struggling to breathe after nine days on maximum oxygen in a Missouri pediatric intensive care unit in early November.
“Something you never want to hear your child say is, ‘I feel like I’m going to die,’” his mother Deb Hensley later told The Daily Beast.
Over the next three months, her sweet-natured son would wage a ferocious fight for his life. Even with the efforts of a remarkable medical team, his battle would at moments seem about to end as grimly as thousands of other COVID cases in ICUs.
“There were times of despair,” Deb recalled.
But Trevor never lost hope.
“Just when we thought we were down and out, he'd do something and prove us wrong and get stronger and keep us going,” Deb said.
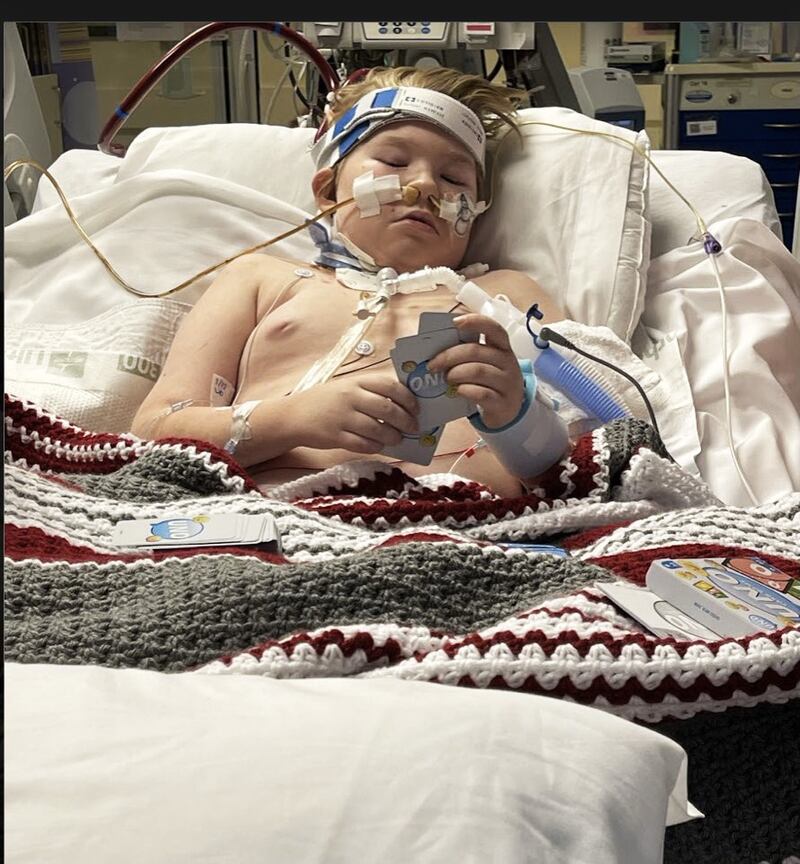
Trevor’s family is pro-vaccine and his mother and father had gotten the jab, as did his older sister, Autumn. They had decided to hold off for a few months with Trevor because at 12 he was the minimum approved age and has a pre-existing condition called phenylketonuria that makes it difficult to metabolize proteins.
In October, Deb caught COVID. The rest of the family also fell ill, but everyone recovered—except for Trevor. His parents took him to Children's Mercy hospital in Kansas City when a fingertip oximeter level dropped to a perilous 85.
At 9 a.m. on Nov. 9, Trevor was sedated and intubated. The doctors warned the Hensleys that if Trevor did not quickly improve they would have to attempt an even more invasive procedure.
“They said, ‘You know, we'll give him two hours if he responds,’” Deb recalled.
The ventilator might as well have been trying to pump air into concrete. Trevor’s blood oxygen level remained perilously low after the allocated time and he was wheeled into an operating room.
A surgeon inserted a large tube, or cannula, through Trevor’s neck into his jugular vein and down to his heart. His blood began running through an artificial lung that removed carbon dioxide and infused it with oxygen in a process called extracorporeal membrane oxygenation, or ECMO.
In a room at the pediatric intensive care unit, Trevor was a small figure surrounded by a mass of tubes and machinery. A team headed by Dr. Jenna Miller began what they call an “ECMO run” with the hope of giving Trevor’s lungs time to heal. Physicians and nurses and respiratory therapists mounted an around-the-clock effort, constantly adjusting the equipment and examining X-rays and sonograms.
“It was hard at the beginning to get him on just the right settings and just the right position with that big cannula and find just the right amount of sedation and he was so, so, so sick,” Miller later told The Daily Beast.
After several days, the team reduced the sedation and Trevor regained consciousness for the first time since being intubated. The doctors explained that children often become agitated when they first awake and are placed in restraints so they do not dislodge the cannula. But Trevor remained almost serene, even though he now found himself with his blood running in and out of a big tube protruding from his neck.
“He woke up and was so calm,” Deb recalled. “He never pulled it, anything. He just was like, ‘All right, we got this.’”
The doctors initially told Deb that Trevor would likely remain on ECMO for up to 10 days. But his lung X-rays continued to be all white, with no indication they were drawing in any air.
“We got through that first week and he just wasn’t improving,” Deb said. “So we just took it day by day. It was a lot of waiting and hoping.”
Around Thanksgiving, the scans showed that a large clot had formed near where the cannula entered Trevor’s heart.
“It was a big debate whether we go in after the clot or sit and wait and hope it does nothing.,” Deb said. “It was very scary. You don’t know if it’s gonna stay there or if it’s gonna block off everything or if it’s gonna go into the machine.”
The parents were able to see the scans on a computer screen in the room. They were told that if they decided to have the clot removed, the surgeon would have only a minute to reconnect the tube.
“We kind of watched it for about 12 hours and they increased his blood thinners and it started to shrink a little bit,” Deb said. “So the decision was to leave it… About every four days we would check to see if it had changed in size or if it moved or anything.”
The blood thinners, administered to prevent other clots from forming, led to bleeding.
“Trevor bled from everywhere:his lungs, his stomach, his bladder, his ECMO site,” Miller said. “So managing all of that was tricky and took weeks.”
He also developed a bacterial infection.
“The doctor said to me, ‘ECMO is a series of complications,’” Deb recalled.
After six weeks, Trevor was still not improving, so Miller decided to try something that had helped adults with COVID, but had not been attempted with a pediatric ECMO patient. Miller met with her team to figure out how they could begin “proning” Trevor without dislodging the cannula.
“We said, ‘What do we have to lose?’” Miller recalled.
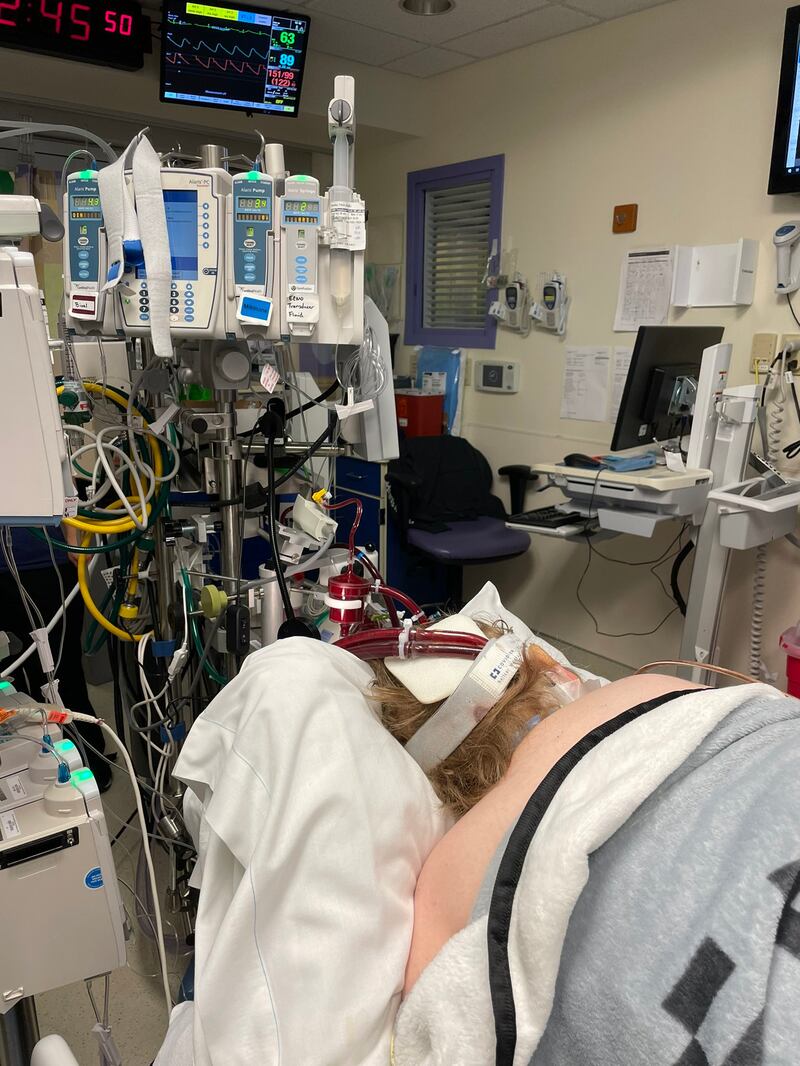
Blankets were piled on Trevor’s chest as a cushion when at least seven team members slowly rolled him over.
“It took seven to eight people to do that every single time safely,” Miller said.
Trevor could not speak because a ventilator was still affixed to him via a tracheostomy, but he and the ECMO team had developed hand signals.
“He’d give us like, ‘Okay, slow down’ or ‘I’m good, keep going,’” Miller said.
The proning gamble paid off when an X-ray showed a small dark area in the upper lobe of Trevor’s right lung.
“You could kind of start to see air there where there was not,” Miller said.
But that was just a start. The ECMO run continued through Christmas and on Trevor’s 13th birthday on Dec. 28. His presents included a virtual reality headset, and he began playing Beat Saber from his bed.
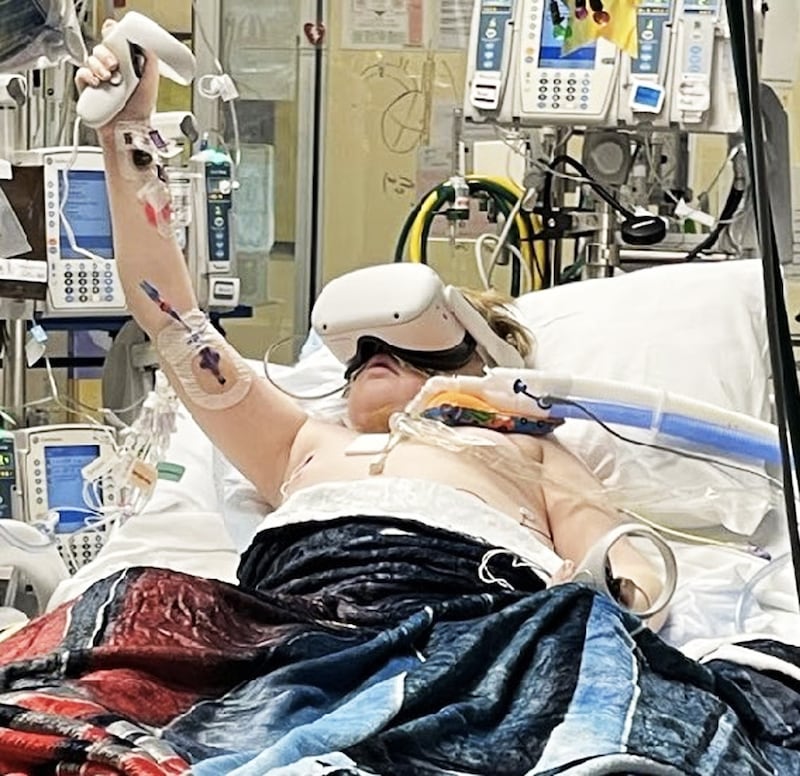
Somebody from the hospital’s children’s services office suggested to Trevor that he could get a visit from a service dog. He wrote a response on a whiteboard.
“No, I want my dog.”
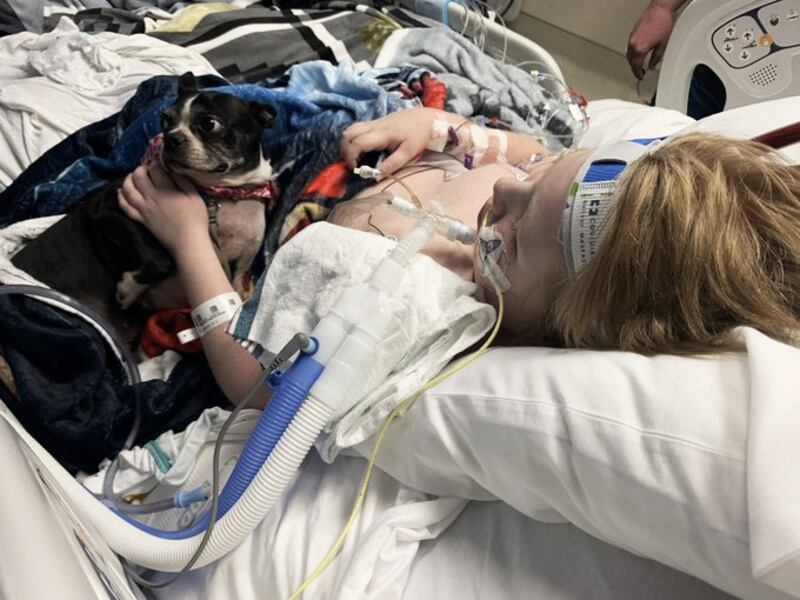
On Jan. 7, Deb distracted Trevor while his father, Dennis placed a surprise in his bed. Trevor looked over to see his Boston terrier, Callie, who had been granted permission for a two-hour visit.
“He reached out with the biggest smile and the biggest blue eyes you've ever seen,” Dennis later said.
Along with proning, the team began shifting Trevor onto a cardiac chair, which starts out flat as a table and then is tilted upwards.
“Once they started sitting him up in that chair, things started instantly getting better,” Dennis recalled. “You could start seeing improvements.”
Deb happened to be home with a cold on Jan. 16, when the team took the latest X-ray.
“His dad called me and was like, you know, so super excited,” she remembered. “He’s like, ‘You gotta look at the text message I just sent you,’ and I opened it up and I see this X-ray.”
Where there had been a white cloud she could see Trevor’s whole lungs, even his diaphragm.
“It was just amazing,” the mother said.
On occasion, the team rolled the cardiac chair from the room along with the ECMO machinery. As many as 11 health-care workers would join in a procession down the hallway,, making sure the lines were secured, checking and adjusting Trevor’s oxygen levels.
“He would actually wave at people as he was going by,” Deb recalled. “It was like a parade.”
Here was a smiling champion of the fight against a virus too many people say does not affect children. He was as brave and inspiring as anyone honored with ticker tape in New York’s Canyon of Heroes.
“There’s people down at the far end… that had never even seen Trevor, but you know, they heard so much about him,” Dennis remembered. “They go, ‘Oh look, it’s Trevor—everybody, wave!’”
He was undergoing physical therapy and a Jan. 18 video captured the encouraging voices of the health-care workers as he lifted kid-sized weights.
“Good job… See, there you go…Excellent, buddy…Fitness videos, here we come!”
On Jan. 23, after 73 days on ECMO, Trevor’s cannula was removed.
“He was nervous,” Deb said. “Afterwards, he was really excited.”
With the tube no longer in his neck, he was returned to a room that suddenly seemed spacious without the ECMO equipment. He asked to have his bed shifted so he could greet people as they went by in the hallway.
“I would say he’s the most caring person you ever met in your life,” Dennis said. “If he knew you and he liked you, you would not get away without getting a hug first. I don't think he’s met anybody he hasn’t liked yet.”
The doctors have told the parents to expect Trevor to be in the ICU for another two months.
“He’s working currently on sitting up unassisted in bed and starting to stand up on his own,” Deb said.
During his time in the hospital , Trevor has dreamed of his horse, a brown and white paint named Jesse.
“He loves his horse,” Dennis said. “If there was a way I could get that horse to the hospital for him, I would do it.”
His medical team is also rooting for him to be reunited with Jesse—outside the hospital.
“I think it’s the one thing they can’t wait to see him do,” his father said. “They want to see him back on that horse.”