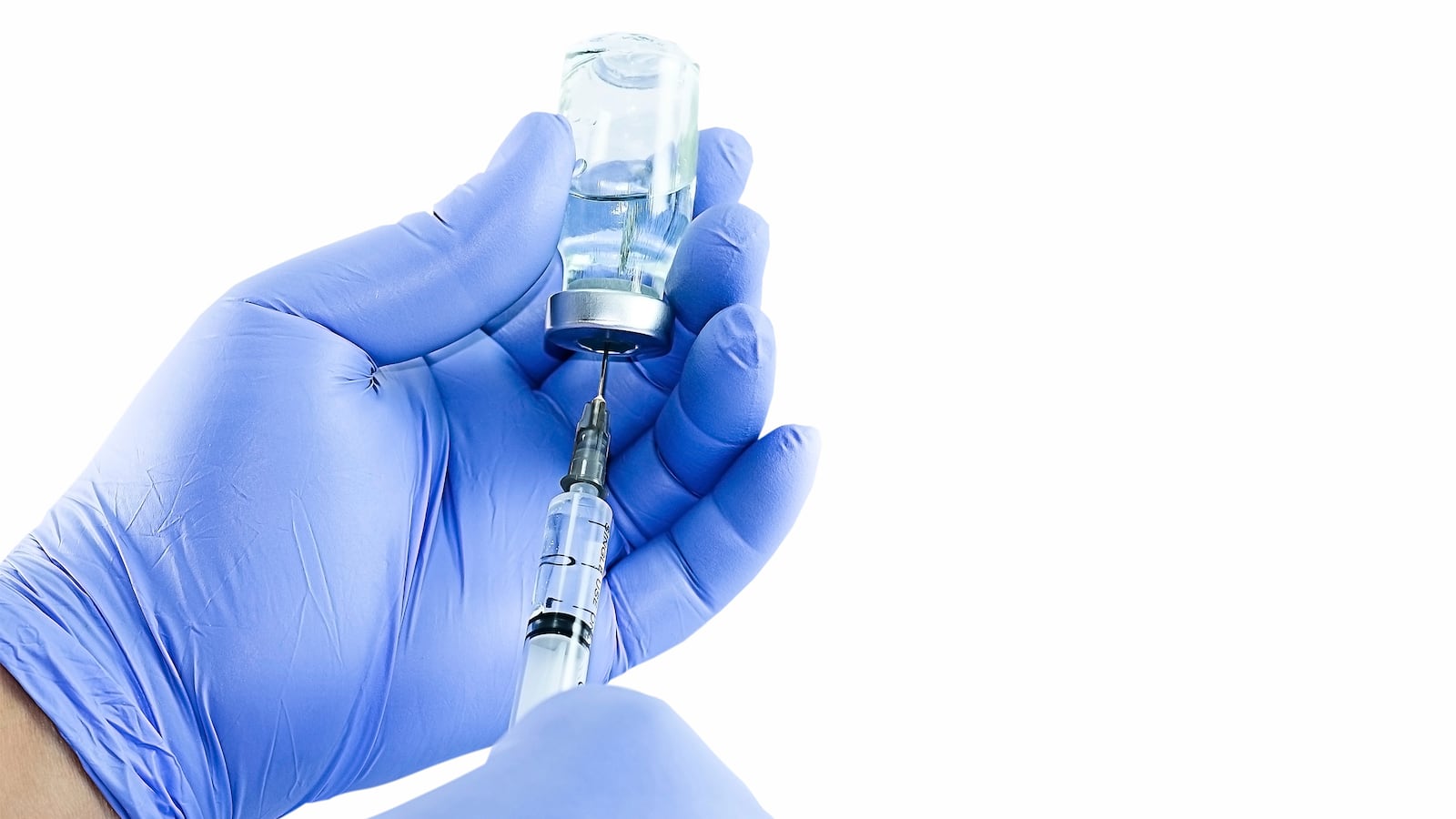
If there were a way to prevent 90 percent of a certain kind of cancer, you’d imagine doctors would go out of their way to encourage their patients to take it.
Unfortunately, when it comes to cervical cancer, you’d be wrong.
According to a new study in the journal Cancer Epidemiology, Biomarkers & Prevention, doctors are not communicating in ways that encourage their patients to receive the vaccine against human papillomavirus (HPV), the virus that causes warts, certain strains of which are a significant risk factor for developing cervical cancer. The vaccine is recommended for both girls and boys starting at 11-12 years of age, and not enough doctors who care for patients of that age are recommending it strongly enough.
The authors of the study surveyed 776 pediatricians and family practitioners and asked about how they discussed HPV vaccination with their patients. Over a quarter do not recommend the vaccination strongly. Many also fail to deliver the recommendation in a timely manner to both girls (26 percent) and boys (39 percent).
This is quite troubling. The United States has a rate of vaccination against HPV far below recommended levels. In 2014, only about 40 percent of girls between ages 13-17 had received all three recommended doses, and for boys of the same age it was even lower at around 22 percent. As the authors of the study note, recommendation from physicians is the single greatest factor in deciding whether or not to vaccinate, and those numbers aren’t going to rise nearly enough if doctors fail to make it a priority.
And a priority it must be. In the year 2012 (the most recent year for which data are available), cervical cancer killed over 4,000 women in this country. Given that there is now an HPV vaccine that is expected to prevent 90 percent of HPV-related cervical cancers, it is baffling that every doctor who takes care of children and adolescents is not recommending it wholeheartedly at every opportunity.
The benefits of vaccination are not limited to cervical cancer, either. About 70 percent of cases of cancers in the tongue and throat are caused by HPV, a fact I routinely mention to parents of boys who wonder why they should vaccinate their kids against cancer in body parts they don’t have. (All of my patients have tongues.) Other strains of the virus included in the vaccine are the ones responsible for most cases of genital warts. In Australia, where resistance to the vaccine is much lower than in the U.S., cases of genital warts dropped by nearly 60 percent in girls and young women and nearly 40 percent in boys and young men following the initiation of a national immunization program.
There is no good reason for our country to miss out on similar benefits.
Most dismaying to me in the new study, however, was the number of physicians who only recommend the vaccine to patients they deem at higher risk. Fifty-nine percent reported curtailing their recommendations in this way. That so many can seemingly misunderstand how primary prevention works is astonishing.
I recommend the HPV vaccine to every single patient starting at age 11, with the rare exception of those with a real medical contraindication to receiving it. Because of both its newness and the lack of imminent threat to other patients that un-vaccinated individuals present while sitting in my waiting room, the HPV vaccine is an exception to our “no non-vaccinators” policy. Yet even in an otherwise uniformly vaccinated patient population, I encounter a lot of resistance to that one, which is in keeping with findings about parents nationwide.
Many question why I would recommend the vaccine for their child even though she or he is not sexually active. Some, perhaps hearing the misinformation promulgated by unreliable sources, fear it is uniquely unsafe or will undermine the chaste lifestyle they hope their teenager will adopt in coming years, neither of which are true. Many simply don’t see the need to give it so young.
While I never try to railroad parents into making a decision they really don’t want, I explain to everyone that the goal of vaccination is to protect all kids as comprehensively as possible before there is any chance they’ve already gotten exposed to a cancer-causing HPV strain. I hasten to reassure them that I’m not recommending the vaccine because I think their kids are or will become high-risk, but since 90 percent of boys and 80 percent of girls can be expected to become exposed to some strain of HPV in their lifetimes (about half of which a high-risk variety), I want every single one of them to be protected. While most infected individuals will clear the infection in a year or two, thousands don’t.
Will a perfectly sexually abstinent lifestyle on the part of both partners before making a lifetime commitment of absolute monogamy confer protection against HPV? Yes. But it’s neither glib nor cynical to advise parents that expecting that outcome is simply unrealistic and impossible to ensure. I would no more recommend vaccinating adolescents after I already suspect they’ve started having sex than I would toss a parachute to someone who’s already leapt out of the plane. That’s just not how good prevention works.
Is it awkward to bring up the topic of a sexually-transmitted infection with parents whose children are not yet old enough to be engaging in sexual activity? You bet. But an unwillingness to have awkward conversations is a sign that you shouldn’t be in primary care. Every patient deserves to be protected against cancer when a means of prevention like the HPV vaccine is safe, effective, and widely available. Providers who fail to advise their patients and their parents likewise are doing them a disservice.