Dr. Vin Gupta was nervous.
The pulmonary and critical care doctor wasn’t worried about getting the COVID-19 vaccine—or the fact he was receiving the shot live, the following morning, on The Today Show. But as he told The Daily Beast that Tuesday afternoon on the phone, the faculty member at the Institute for Health Metrics and Evaluation (IHME) at the University of Washington had been barraged with messages and emails and Twitter mentions from vaccine skeptics, including threats on his life, and invitations to “come make me wear a mask.”
It was more than enough to stir up some anticipatory anxiety about the sort of backlash he might receive after actually getting the shot—and what lay ahead for the country around him.
In the days after he received his first dose of the Pfizer vaccine, Gupta caught the attention of Fox News’ Tucker Carlson and Sen. Ted Cruz. The latter called Gupta part of “a bizarre, lunatic, totalitarian cult” for saying that a vaccination “does not mean you should be participating in things like traveling in the middle of an out-of-control pandemic or that you’re liberated from masks.”
In other words, for reminding people that this coronavirus nightmare isn’t over yet.
“They were flagrantly trying to distort what I was saying to confuse people,” Gupta told The Daily Beast this week. He added that he was “exhausted” by that kind of bad-faith attack, which he called “the public piece” of his job, “because there are people who are trying to make it seem like doctors and nurses are fearmongering.”
Ultimately, the Air Force veteran said he “felt duty-bound to use his platform responsibly and to help reassure.”
Still, disinformation and extremist rhetoric could have a big impact on what the next year of vaccine distribution and pandemic surveillance looks like—and how quickly life might get back to something approaching normal.
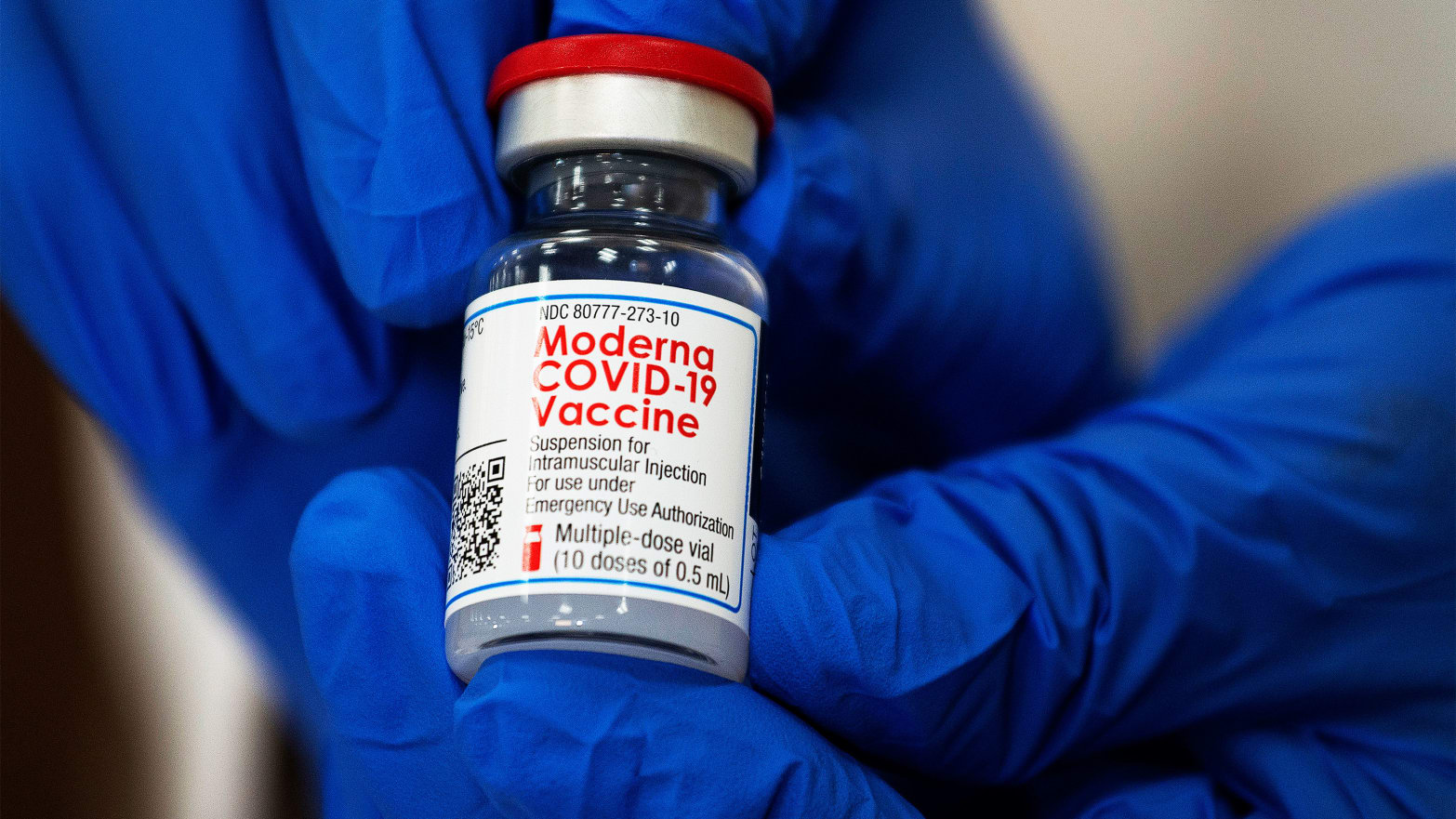
As of this week, there were two COVID-19 vaccines authorized for emergency use in the United States. One was developed by the American pharmaceutical company Pfizer and German firm BioNTech, the other by Massachusetts-based Moderna. There are more coming down the pipeline, like a vaccine by Oxford University and AstraZeneca, which is expected to seek Food and Drug Administration (FDA) authorization in the coming months.
JOSEPH PREZIOSO/AFP via Getty Images
But after a year of economic, physical, and emotional devastation, in which more than 18 million Americans contracted the virus, glaring questions remain, even as help is clearly on the way.
Among them: Will there be lower community transmission earlier in the year, or will only those who have received the vaccine be significantly safer? Will Americans refuse to be vaccinated in large numbers? Will the virus itself mutate more quickly than scientists predict? And will health-care workers finally get a break?
If nothing else, the early reaction to the vaccine in the darkest corners of the internet was an ominous sign.
The Dire Ideal
In the best-case scenario, vaccine batches will continue to be distributed with relatively minor hurdles from here on out. Then, they will quickly be joined by still more vaccines—from the same companies or from others, like AstraZeneca—who can shore up efforts to get the shots to as many Americans as possible. In this scenario, researchers are also able to develop a vaccine that children under the age of 16 can take, which is currently not authorized for the Moderna or Pfizer drugs.
In that case, the entire country might experience some measure of pandemic relief by as soon as the spring. Health-care workers would enjoy a respite from the startling physical and emotional toll of their jobs caring for the hundreds of thousands of Americans who became severely ill and died. There would be significantly fewer severe cases and deaths from COVID, and nowhere would that be clearer than in hospitals.
“I’m thinking that we’re going to see some real differences by April and May,” said Dr. Arnold Monto, an infectious disease expert and the acting chair of the Vaccines and Related Biological Products Advisory Committee that endorsed both vaccines.
He echoed comments from Dr. Anthony Fauci on Monday, when the director of the National Institute of Allergy and Infectious Diseases told The Daily Beast that aggressive vaccinations in May, June, and July could mean an “overwhelming majority” of the population is vaccinated by August.
In this scenario, the big questions about the vaccines will be answered, and the answers will be good ones. Do the vaccines prevent transmission from healthy or moderately ill people to others? Yes. Doctors who catch mild or asymptomatic cases of the virus after getting vaccinated will not spread it to their families. Does immunity last at least one year? Potentially longer? Yes. In other words, we won’t need to handle booster shots—beyond the second initial dose—or scary viral mutations until researchers and frontline workers have had a little room to breathe.
Do you know something we should about the coronavirus, or how your government, school, or business is responding to it? Email Olivia.Messer@TheDailyBeast.com or securely at olivia.messer@protonmail.com from a non-work device.
“I’m fairly optimistic,” said Monto, telling The Daily Beast that because symptomatic cases of the virus spread more readily than do asymptomatic ones, the least-bad answer to that question is possible, and even probable.
In this scenario, though there may be a few relatively small pockets of transmission over the summer—superspreader events or outbreaks—some people could be able to wander around outside of their homes without a mask on, without feeling guilty about it. Still, public health leaders like Fauci have noted that mask use, in general, will be around for a long while.
At least in this future, everyone or nearly everyone who should get the vaccine does get the vaccine, despite anti-vaccination messaging or prior vaccine hesitancy.
In the meantime, researchers will have been able to discover, test, and disseminate more therapies—like monoclonal antibodies—for severe cases of the virus, or to act as prophylactics, and to protect those who haven’t received the vaccine yet.
That said, even in the best-case scenario, when it comes to January and February, mass death is inescapable. As Gupta put it: “The vast majority of people that are going to die from this virus will die irrespective of the vaccine distribution strategy.”
It should be noted that public health experts also suspect a possibly more-transmissible variant of the coronavirus is already on U.S. soil, and that millions of Americans still plan to travel for the holidays. How many millions of people actually travel, which precautions they will take while doing so, and what strains are involved, leave a lot of uncertainty.
In all scenarios, said Dr. Jennifer Horney, founding director and professor in the University of Delaware’s epidemiology program, American hospitals will still be dealing for the next six to eight weeks with the cases contracted on Christmas Day.
“We have to live with the cases we have now for the next few months,” said Horney.
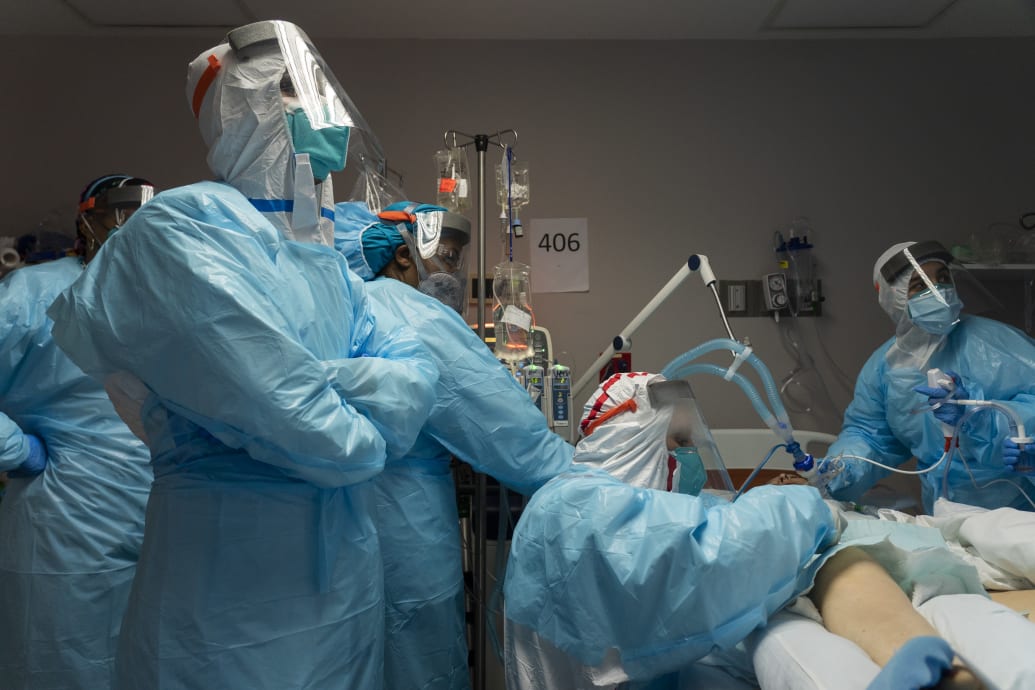
Go Nakamura/Getty Images
The Brutal Setback Scenario
The worst-case scenario for 2021 begins with people still congregating and flouting public health guidelines in January, without having been vaccinated. On that score, Horney is not optimistic.
“I think it’s going to be a good long time in 2021 until we feel any cumulative effect on public health, because we’re still not changing our behavior,” she said. “We still have to live with the coming hospitalizations and death.”
“We’re going to be close to 500,000 deaths by March,” she continued, echoing projections published last week by Gupta’s colleagues at the University of Washington. The leading research group’s models, which have been used by the White House, estimated that 562,000 Americans will have died from the virus by April 1, 2021.
In the worst-case scenario, the big questions about the vaccines will be answered, and the answers are terrible ones. Do the vaccines prevent transmission, in addition to severe infection? No. It turns out the vaccine prevents you from getting sick but it doesn’t prevent you from spreading it to someone who hasn’t had their shots yet. Does immunity last at least one year? Potentially longer? No. We might even be forced to re-evaluate our priority lists in order to provide booster shots to the already-vaccinated by the time the year is out.
Then there’s vaccine hesitancy. There have been several studies on Americans and vaccines, and as of this week, millions still say they won’t take the COVID-19 vaccine. Fauci told The Daily Beast earlier this month that his “primary biggest fear is that a substantial proportion of the people will be hesitant to get vaccinated.”
In this scenario, vaccine skepticism, actual problems with the doses, unforeseen side effects, human error in the logistics of transporting the vaccine, or distribution issues—wasted doses from problems with Pfizer’s required ultra-cold storage, for example—hamper the effort to achieve anything close to herd immunity. Many people don’t get the vaccine until after next year.
One possibility is that “we have so many mutations that the vaccine stops working” in that scenario, said Monto. To be clear, the consensus among experts—including Monto—is that such a situation is very unlikely.
Then, the lower-income countries that were already slated to see the vaccine as late as 2024, per Horney, would take even longer to get their share of the global supply. Community transmission, in this case, would not be controlled the way that it was anticipated to be by the summer, and when cold weather returns in the fall, things still don’t look pre-pandemic “normal.”
In fact, deaths and cases could explode once again.
At the same time, the year-long health problems that people did not feel safe getting checked at annual doctors appointments—mammograms, colonoscopies, skin cancer checks—are once again skipped, and the health-care sector sees one nightmarish year roll into another.
The Messy, Deadly Middle
The Institute for Health Metrics and Evaluation model projects that, with the vaccine rollout, about 34,500 lives will be saved by April 1, 2021. A more rapid rollout would save 55,400 more lives compared to a no-vaccine scenario, it found. The model projects that 100.1 million people are expected to be vaccinated by April 1 in the U.S. With an even faster rollout, however unlikely, the number of vaccinated individuals could reach 194 million.
Dr. Maimuna Majumder, a computational epidemiologist and a faculty member at Harvard Medical School and Boston Children's Hospital's Computational Health Informatics Program, pointed out that the journey to a vaccinated United States will not be linear. Some counties, where the vast majority of the population is elderly, will be safer and free from community transmission sooner than others.
That works in reverse as well, she said.
“We need to be very mindful of the fact that some of the same communities that have been ravaged by this pandemic are also going to be left high and dry by the vaccine,” Majumder told The Daily Beast, noting the health-care inequality that still falls along race lines in the United States. “When we leave some pockets undervaccinated, it means they are going to be vulnerable to outbreaks in the future.”
For public health authorities, it will be paramount, she said, to keep an eye on issues of logistics and the distribution of two doses per vaccine to ensure that everyone who receives one dose receives two. Those problems “are going to disproportionately affect underserved groups,” Majumder added, noting that those areas will likely be plagued by the virus longest.
So what’s realistic, said Majumder, is that some communities will reach lower levels of community transmission, or herd immunity, first. But what about the country as a whole?
“I think there are different phases of this,” said Horney. “Are we going to reach absolute herd immunity given the percentage of people who will take it once it’s completely available? I think that’s going to be a long time.
“But can we in the next 6 months vaccinate everyone who is willing and make things tremendously safer for people?” she asked. “Yes, yes we can.”