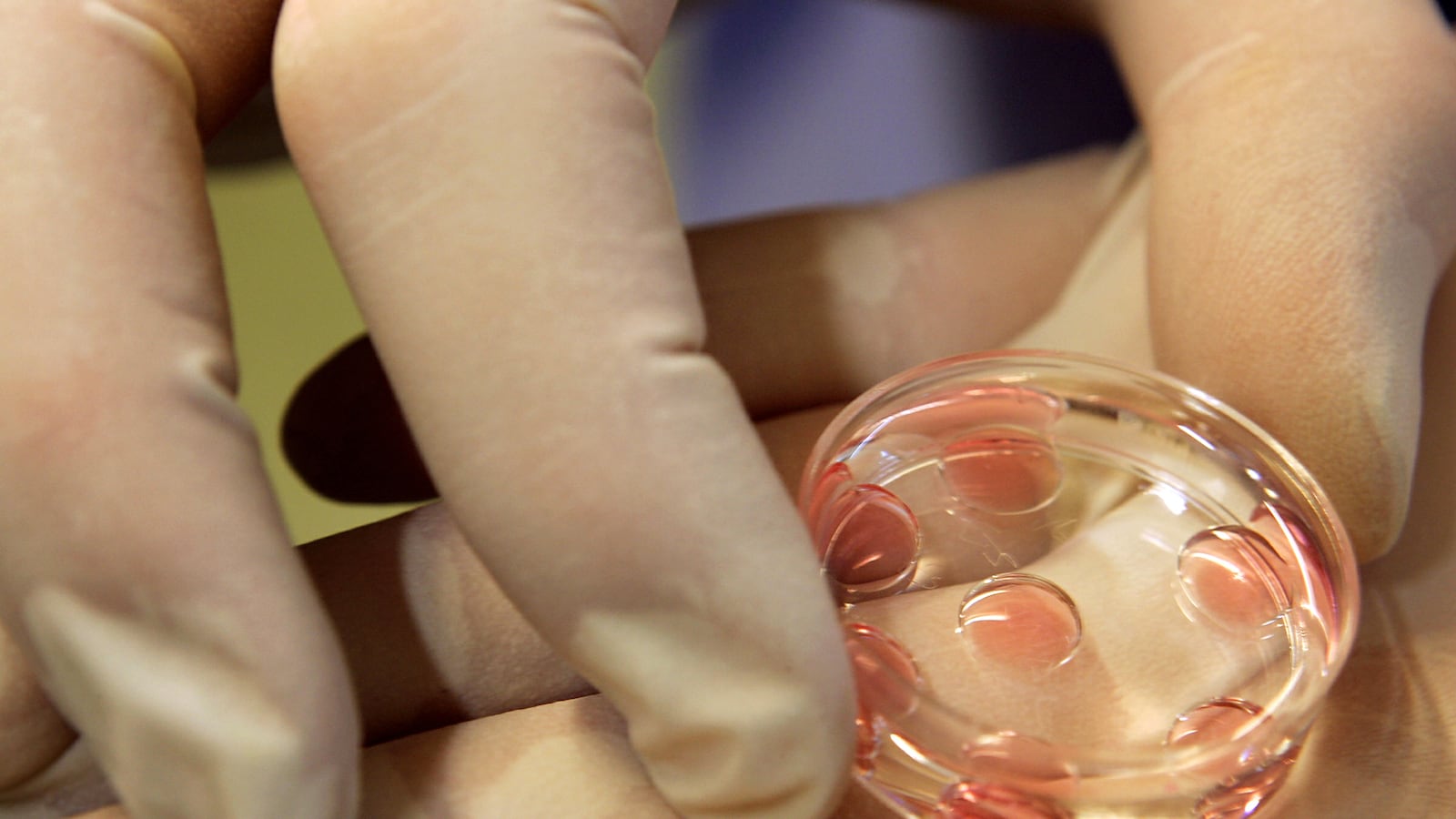
A new startup claims it can help women get pregnant by using artificial intelligence to grade their eggs—a technology that could save couples thousands of dollars and months of frustration on failed attempts at in vitro fertilization.
The company, Future Fertility, has developed an AI analysis tool to test the quality of human eggs before they’re used in IVF. According to the company, the technology can currently predict whether or not an egg will be fertilized 90 percent of the time. Eventually, they hope to predict pregnancy outcomes based on a single picture of an egg.
“There’s a lot of missing information for physicians and for patients and we believe strongly that artificial intelligence can solve this riddle,” Dr. Dan Nayot, the company’s medical director, told The Daily Beast. “That’s the technology we’ve created here.”
The innovation, if it works, would be a welcome one. The average IVF cycle currently costs about $10,000 and results in a successful birth only 20 to 35 percent of the time. Once a woman is over 35, her chances are even lower than that. For most people looking to conceive, the process is both costly and exhausting.
Rene Bharti, the chairman of Future Fertility, knows the frustration well. He first dreamed up the technology while he and his wife were trying to conceive via IVF. Their doctor—Dan Nayot—told them a scoring system existed for embryos and sperm, but not for eggs. Combining Nayot’s medical experience and Bharti’s background in AI, the two founded Future Fertility in order to change that.
The AI program, Violet, is named after Bharti’s now 15-month-old daughter.
“I’m lucky enough that if we had to do four or five cycles [of IVF] I probably could get away with paying for it,” Bharti said. “But there are a lot people that… it’s a lot of money and it’s a game-changer, potentially.”
Charles Bormann, a chemist at Northwestern University, said his lab is currently testing a similar product and has seen comparable success rates. He called artificial intelligence “the future of IVF,” saying it could pick up on differences in eggs that humans cannot perceive, much less write into an algorithm. He suggested it could even help prospective mothers before the fertilization process starts, by guiding them in how many eggs to freeze.
Other experts are more skeptical. Norbert Gleicher, medical director of the Center for Human Reproduction, said he was unimpressed with Future Fertility’s claim that they can successfully predict fertilization 90 percent of the time.
“Every experienced embryologist who looks at an egg after retrieval can tell you whether the egg will be fertilized or not,” said Gleicher, who has taught obstetrics at Yale and New York University. “I wouldn’t spend a dollar on that.”
Future Fertility says internal tests prove Violet is more successful in predicting fertilization than an embryologist alone, and added that it is 65 percent successful in determining whether an embryo will survive more than five days. (They said they could not provide this data for review because of HIPPA law.) After the product is rolled out to more IVF clinics, Nayot said, they hope the technology will learn to predict outcomes even further down the line. The company says it hasn’t finalized pricing yet but it will most likely be determined on a country-by-country and clinic-by-clinic basis.
Still, Gleicher is doubtful that the product will make much of a difference. He said he has seen countless companies launch “innovative” IVF products in recent years, but none were able to substantially improve outcomes.
“Unfortunately we have witnessed a lot of startups in this arena coming and going with claims that are not true,” he said. “Sometimes the longer they stay in business the more negative impact they wind up having on IVF.”
One such failed start-up was OvaScience, which burst onto the scene in 2016 with the promise of extending women’s fertility windows. At one point, the company was valued at $1.8 billion. By 2018, after many of the company’s promises failed to pan out, its stock was essentially worthless.
Future Fertility’s embryology director, Jim Meriano, and Nayot, its medical director, both work with Dr. Robert Casper—one of the first endocrinologists to offer OvaScience’s product, even before it was approved by the FDA. At the time, fellow fertility experts raised questions about whether the technology was safe.
The Violet technology was trained, in part, at Casper, Nayot, and Meriano’s clinic. Nayot says the product is completely different from what OvaScience was developing, and is solely a diagnostic tool. He added that the company will be doing prospective studies to validate the accuracy of their predictions.
But even Borman, the scientist who called Future Fertility the “future of IVF,” urged caution in assessing new products.
“I just think people are very vulnerable when they're struggling with fertility,” he said. “So I think people are willing to pay whatever to have any sort of advantage, and that is not how you should be trying to market this technology.”