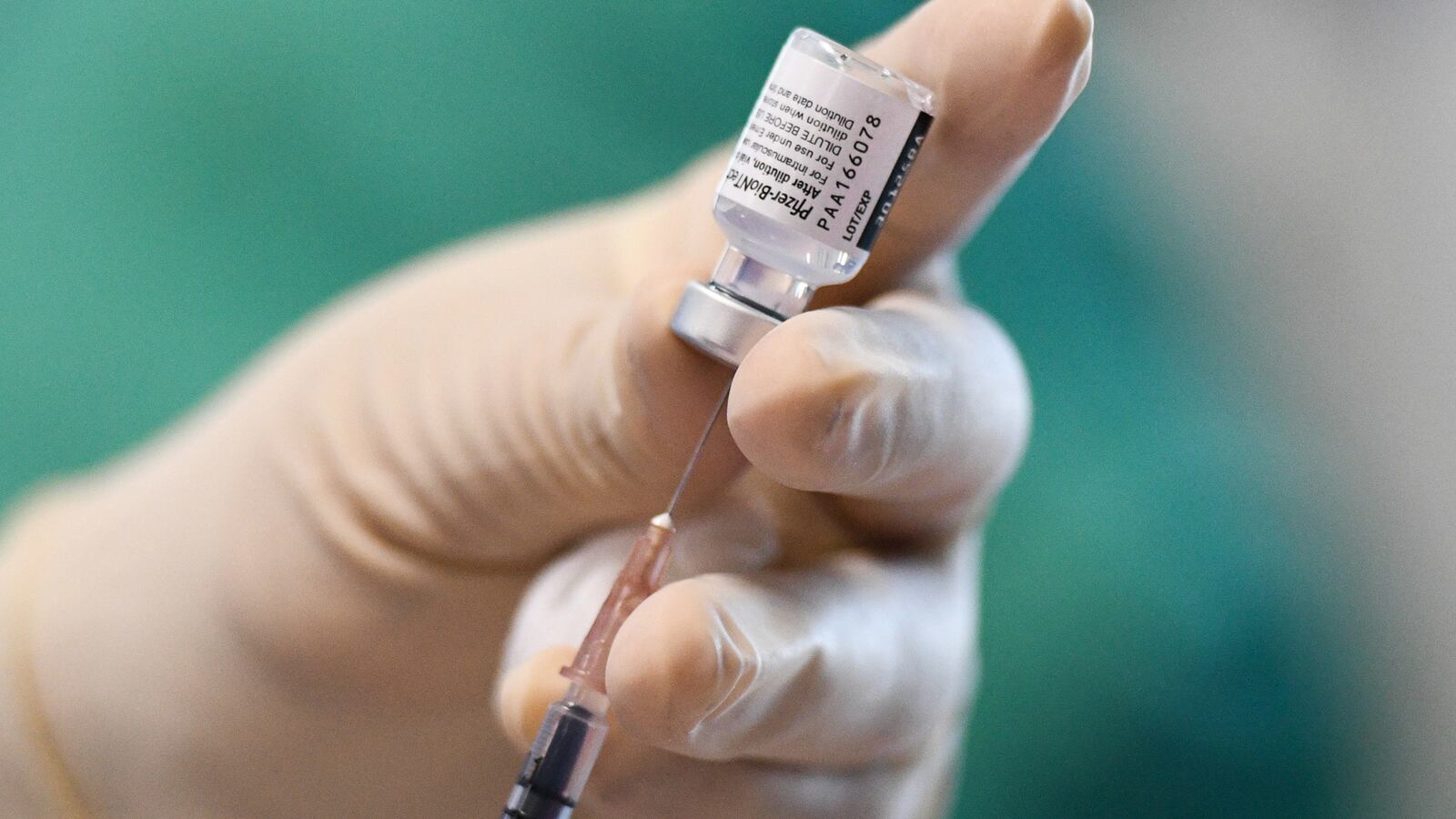
The Biden administration on Wednesday endorsed booster shots for millions of Americans already vaccinated against COVID-19, proposing they begin in earnest by late September as the ultra-contagious Delta variant wreaks national havoc.
The FDA and CDC were still due to sign off on extra shots before most Americans could begin receiving them. And experts broadly endorsed the move given early indications protection offered by safe and effective coronavirus vaccines might wane over time. But coming just days after the feds authorized extra shots for the immunocompromised, and with America’s anti-vaxxer problem showing no signs of abating, the prospect for a smooth rollout was murky at best.
“Based on our latest assessment, the current protection against severe disease, hospitalization, and death could diminish in the months ahead, especially among those who are at higher risk or were vaccinated during the earlier phases of the vaccination rollout,” Centers for Disease Control (CDC) Director Rochelle Walensky and acting Food and Drug Administration (FDA) Commissioner Janet Woodcock said in a joint statement co-signed by a slew of other federal medical experts. “For that reason, we conclude that a booster shot will be needed to maximize vaccine-induced protection and prolong its durability.”
The new guidance dropped just a week after the FDA first authorized a booster shot—but only for several million Americans with weaker immune systems. Among them: cancer patients, recipients of organ transplants, and people with certain immune disorders.
All things being equal, experts The Daily Beast spoke with all supported the idea of an extra shot. As certain viruses evolve over time, they can reduce the effectiveness of vaccines. Periodic boosts can help your immune system maintain a high level of protection.
“It is not unusual to discover that vaccines require boosters,” Jennifer Reich, a University of Colorado sociologist who studies immunization, told The Daily Beast.
But even as the feds began offering new data pointing to the need for boosters on Wednesday, experts said it was hard to say how urgent the need for boosters really is right now when it comes to COVID-19 in the United States. At best, some argued, the FDA has botched the rollout of its booster guidance by expanding its eligibility rules in piecemeal fashion. At worst, it’s risking a run on shots by tens of millions of people who arguably shouldn’t be a priority.
To be very clear, the vaccines with emergency authorization from the FDA—including two-shot messenger-RNA jabs from Pfizer and Moderna and a conventional, single-shot vax from Johnson & Johnson—are highly effective at preventing severe illness and death. Even against the Delta variant.
That protection has also proved at least relatively durable over time. One recent study, the results of which appeared in the science journal Nature in June, found that the mRNA vaccines produced a “robust and prolonged” ability to produce virus-fighting T-cells. The study found that the immune effects of the mRNA vaccine were superior to the effects of a flu vaccine.
This is why some experts questioned the latest guidance. The FDA’s endorsement of extra shots for everyone could, even more than its previous guidance for the immunocompromised, send the wrong message to those still well-protected.
This all at a time when most of the world’s population still doesn’t have access to any vaccine, to say nothing of boosters.
“Without a major increase in supplies, offering third doses to our entire population would create even greater vaccine supply scarcity globally, robbing poor people of the chance to get a life-saving vaccine,” Lawrence Gostin, a Georgetown University global-health expert, told The Daily Beast.
That said, the feds insisted they were simply following the data as we learn more about the Delta variant and the vaccines’ durability. Here’s what you need to know about the booster shot situation in the United States.
Who can get a booster now?
The new authorization, which is still pending, would expand booster eligibility from only three million or so Americans with weak immune systems to many more. But among the newly-eligible population, the FDA is suggesting healthcare workers, residents of long-term care facilities, and the elderly should go first for their extra shot.
If your head is spinning, you’re not alone. Irwin Redlener, the founding director of Columbia University’s National Center for Disaster Preparedness, criticized the FDA for changing its lines on boosters twice over a period of just a week.
“This was pretty much a mini-disaster because it does nothing to enhance public confidence,” Redlener, who is also a Daily Beast contributor, said before the feds made the announcement. “I think there should have been a lot more caution, a lot more warning to the public that the guidance released a week ago might change.”
To be very clear, immunocompromised Americans should absolutely get a booster shot, as the feds recommended last week. Redlener was adamant about the benefits of an extra shot for people with weaker immune systems. But for the rest of us vaccinated folk, the reasoning behind a booster is a bit murkier.
Are there boosters for all the vaccines?
No. So far, the FDA’s still-pending booster authorization seems like it will only apply to the mRNA vaccines from Pfizer and Moderna. The feds have not cleared recipients of the single-dose Johnson & Johnson jab to get an extra shot of that vaccine, even if they are immunocompromised.
That said, Johnson & Johnson is studying a booster. “Data from this study will be available in the coming weeks,” Alison Fennell, a company spokesperson, told The Daily Beast. FDA authorization could follow.
Are the boosters the same formulation as the original shots?
At present, yes. Now, the pharmaceutical industry is developing improved versions of the COVID vaccines that might hold up better against specific lineages. But the FDA hasn’t yet OK’ed those new jabs for widespread use.
If you had side effects from the first or second shot, will you get them again?
Possibly. The mRNA boosters are, after all, identical to the initial doses. When Moderna tested boosters on trial subjects, the most common side effects were fatigue, headache, and muscle and joint pain.
What do we know about effectiveness?
Much of this information is coming from the companies themselves, in absence of an abundance of independent studies.
Moderna studied boosters earlier this year and released its initial findings in May. An additional dose of the company’s existing mRNA-1273 vaccine, taken six to eight months after the first, “increased neutralizing titers against SARS-CoV-2 and two variants of concern [Beta and Gamma] in previously vaccinated clinical trial participants,” the company stated.
In other words, according to its manufacturer, a booster can extend immunity.
Pfizer and its partner firm BioNTech conducted their own study of boosters and announced early results on Monday. “Safety and immunogenicity data in individuals who received a third dose of the Pfizer-BioNTech vaccine (BNT162b2) show a favorable safety profile and robust immune responses,” the companies stated. “The booster dose elicited significantly higher neutralizing antibody titers against the initial SARS-CoV-2 virus (wild type), and the Beta and Delta variants, compared to the levels observed after the two-dose primary series.”
“A booster dose given within six to 12 months after the primary vaccination schedule may help maintain a high level of protection against COVID-19,” Pfizer and BioNTech added.
The question, of course, is whether the extra immunity is necessary when the initial two doses hold up pretty well over time for most people, and when a large majority of the world’s population—at least two-thirds—hasn’t been vaccinated at all.
Data Wallensky cited Wednesday indicated that, over time, the ability of the mRNA vaccines to prevent all COVID infections declined somewhat—from 92 percent protection to 80 percent after a few months. The feds also cited data pointing to a sharper decline in protection against infection among some of the most vulnerable Americans, at nursing homes, as the Delta variant took hold.
What doesn’t seem to change—at least nearly as much—is the ability of the vaccines to prevent serious infection and hospitalization, and death. The data, much of it from the Mayo Clinic, pointed to stable protection against severe illness and hospitalization through July, at which point many people were five or six months out from their initial shot. The feds cautioned, however, that the hospitalization data in question may only have offered a limited perspective on the Delta variant.
The question is if the vaccines are still keeping the vast majority of people out of hospitals after six months, is it worth it to hurry up and get those people boosted? The alternative, at least in theory, is to use that same mRNA to give someone their first shot rather than juicing the (still robust) immunity of an already-vaccinated individual.
Does the United States have enough supply?
Locally, yes. The U.S. government spent billions of dollars securing priority access to shipments of vaccines from the leading manufacturers. As of this week, the feds have received a total of 417 million doses for immediate use, according to the Centers for Disease Control and Prevention (CDC). States had administered 358 million of those doses, leaving 59 million doses close at hand.
With around 700,000 Americans getting a first or second dose every day over the past week, those 59 million doses could last a couple of months, even taking into account the possible spoilage of old doses. Fresh shipments are already paid for, and according to The New York Times, the feds also have 100 million more doses in longer-term reserve.
Does this mean other countries won’t get enough?
Possibly. And that’s one of the main arguments against boosters. While it’s unlikely the U.S. will run out of vaccines, every dose that our government buys is a dose a foreign government can’t buy. After all, vaccine producers are making doses as fast as they can to meet massive demand all over the world.
It’s not for no reason that Tedros Adhanom Gebreyesus, the head of the World Health Organization, has called for a moratorium on boosters. “I understand the concern of all governments to protect their people from the Delta variant, but we cannot accept countries that have already used most of the global supply of vaccines using even more of it, while the world’s most vulnerable people remain unprotected,” he said.
It’s always an option for the U.S. government to ship some of its own doses abroad. The feds have already donated at least 110 million doses to 60 countries, according to a White House release. The Biden administration has announced a plan to donate another 500 million doses to 100 countries this month. But if Americans get boosters by the millions, like the FDA recommends they do, that could eat into global supply.
The question is, is it justifiable, or even a smart public-health strategy, for Americans to get an extra dose when most of the world still can’t get an initial one? The optics are already clear: “The announcement to offer third doses to our entire population is tone deaf to the rest of the world, who can’t even get a single dose for health workers,” Gostin said.
Will we need a new booster every time there’s a new variant spreading?
That’s the billion-dollar question. In the case of diseases such as measles, mumps, and rubella, it’s enough to get a two-dose vaccine just once in a lifetime. For others that are caused by viruses that mutate quickly—the flu, for instance—fresh shots are necessary every year.
So far, COVID is more like measles than the flu. That is to say, it has evolved to produce new lineages, but none of those lineages significantly evade the vaccines. New lineages are coming, of course. With so many billions of totally unvaccinated people all over the world, SARS-CoV-2 has plenty of opportunities to spread and mutate.
It could be years before we finally suppress COVID globally, assuming we ever do. Unless and until that happens, it’s always possible the novel coronavirus will mutate into a lineage that can evade the vaccines. If and when that happens, we’ll need new jabs.
The good news is that mRNA technology lends itself to quick upgrades. Swap out one kind of RNA for another, and you’ve produced a whole new vaccine.
The problem, in the event SARS-CoV-2 figures out how to dodge the current vaccines, isn’t adapting the jabs to the disease. It’s convincing millions of Americans, many of whom were reluctant to get their initial shots, to go back and get vaccinated again. All while keeping up the pressure on the unvaccinated population to go in for their first dose.
“Our ongoing need for vaccines and boosters is in part fueled by low levels of vaccines in communities, which allow for community spread of the virus and an increasing number of variants,” Reich said. “So ironically, those who want to see fewer vaccines and vaccine requirements might actually be the ones driving the need for more vaccines.”
Booster shots make sense, and you should go and get one when the feds say it’s your turn. But perhaps even more obvious is that if you or someone you know is unvaccinated and want the confusing, rapid-fire booster guidance to end, get vaccinated.
As ever, it’s the only way out of this nightmare.